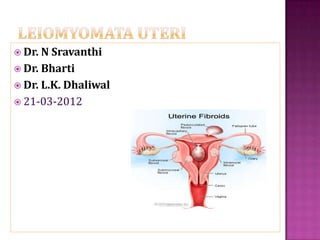
Leiomyomata uteri
- 1. Dr. N Sravanthi Dr. Bharti Dr. L.K. Dhaliwal 21-03-2012
- 2. A LEIOMYOMA is a benign monoclonal tumour composed of smooth muscle cells but containing various amounts of fibrous connective tissue. Its well circumscribed but not encapsulated. Various terms to refer these tumors : fibromyoma, myofibroma, leiomyofibroma, fibroleiomyoma, Myoma Fibroma Fibroid
- 3. Most common benign tumours of uterus and female pelvis. In 20 – 40 % women in reproductive age group. About one third of hospital admissions to gynecology services. Reported to occur in 77% of uteri obtained from TAH specimens The hysterectomy specimens from premenopausal women - 7.6 myomas; postmenopausal women - 4.2 myomas
- 4. Precise cause is unknown Genetic factors – 40% have chromosomal abnormalities (t:12,14), (del 7) (trisomy 12) Hormones Estrogen and progesterone appear to promote development Growth factors TGF – β, bFGF, EGF, PDGF, IGF, PRL
- 5. Age (increases with age) Ethnicity ( African women 2.9 times than White ) Endogenous hormonal factors Weight ( 21% increased risk with every 10kg rise body weight) Diet and Exercise and Obesity Family history/genetic predisposition(first degree relative- 2.5 times increases risk) Oral contraceptives(no definite relationship) Menopausal HRT: Therapy will not stimulate growth Parity( nulliparous > multiparous ) Smoking (reduced) Tissue injury
- 6. Benign tumors that originate from smooth muscle cells of the uterus Range in size from seedlings to large uterine tumors solitary or multiple Depending on the location Within the myometrium (intramural) Externally extending to the serosa (sub serous) internally impinging on the uterine cavity (submucous)
- 8. Disseminated peritoneal leiomyomatosis, Benign metastasizing leiomyoma, Intravenous leiomyomatosis, Parasitic leiomyoma, and Retroperitoneal leiomyomatosis
- 10. In one-third of patient Usually menorrhagia, but also can present as metrorhhagia or as menometrorrhagia. Associated with any type of fibroids, but there is a distinct clinical pattern with each type. Bleeding is more common and severe in in submucous fibroids.
- 11. The submucous leiomyoma bleeds freely at menstruation and may also bleeds between periods If the submucous myoma is pedunculated, there is usually a constant, thin, blood-tinged discharge in addition to the menorrhagia. Intramural myoma beginning to encroach the uterine cavity can also present as menorrhagia. Intramural fibroid near serosa, pedunculated serous tumours can also present with abnormal bleeding.
- 13. a) Increased surface area b) Local hyperestrogenism in areas adjacent to the submucous tumor, endometrial hyperplasia and endometrial polyps. c) Thinning and ulceration of the endometrial surface d) Interference with myometrial and spiral arteriolar(basalis portion) contractility e) Congestion and Endometrial venule ectasia
- 14. Urgency Frequency Urinary incontinence Acute retention Overflow incontinence Constipation/ Tenesmus
- 15. Abdominal and pelvic discomfort, Feeling of heaviness in pelvis, Dyspareunia Spasmodic dysmenorrhoea Torsion in pedunculated myoma Red degeneration Diffuse adenomyosis Concomitant pelvic disease: ovarian pathology, PID, endometriosis, urinary tract or intestinal pathology
- 16. In 5-10% of infertile women Only 2-3% of infertility may attributed to them(provided other causes have been excluded) “Removal of fibroids that distort the uterine cavity may be indicated in infertile women, where no other factors have been identified, and in women about to undergo in vitro fertilization treatment.” SOGC CLINICAL PRACTICE GUIDELINES No. 128,May 2003
- 17. Mechanisms: Interference with sperm transport, ovum capture Displacement of cervix Deformity of uterine cavity Distorted adnexal anatomy Obstruction of proximal fallopian tubes Interference with implantation Increased or disordered uterine contractility Local inflammation Impaired blood flow
- 18. Common during pregnancy OCPs containing high dose of estrogens HOWEVER – “Rapid growth in post-menopausal women is highly suggestive of malignancy” Sarcomatous change in leiomyoma Sarcoma Carcinoma endometrium Estrogen secreting ovarian neoplasm
- 19. Incidence of leiomyosarcoma in hysterectomy specimens of women receiving surgical treatment for fibroid 0.1% in reproductive age group 1.7% after age of 60 years Leiomyosarcoma in a series of hysterectomies performed for presumed uterine leiomyomas. Am J Obstet Gynecol 1990;162:968–76
- 20. Careful history regarding symptoms. Bimanual pelvic examination : (enlarged, irregularly shaped, firm, and non-tender uterus )
- 21. Ultrasound (TAS and TVS) best initial test based on its noninvasive nature and cost- efficiency. lowest sensitivity and specificity concentric, solid, hypo echoic masses anechoic components - from necrosis. Calcifications are hyper-echoic, with sharp acoustic shadowing
- 23. Provides contrast Better defines submucous myomas, polyps, endometrial hyperplasia, or carcinoma Precisely defines the location, attachment of the submucous fibroids and also determines whether it is amenable to hysteroscopic resection Limitation of detection of leiomyomata is o.5 cm diameter.
- 24. More sensitive(64%) and specific(88%) than US Evaluation of number , size, and position of sub- mucosal, intramural fibroids and sub serous fibroids. Allows precise myoma mapping - Helpful in planning surgery May differentiate adenomyosis from myomas. (adenomyosis is associated with junctional zone thickness of more than 15mm (or 12 mm in a non-uniform junctional zone). Focal, not well-demarcated, high-intensity or low-intensity areas in the myometrium also correlate with adenomyosis) Expensive modality
- 25. FIGO classification system (PALM-COEIN) for causes of abnormal uterine bleeding in nongravid women of reproductive age
- 26. International Journal of Gynecology and Obstetrics 113 (2011) 3–13
- 28. Women who are mildly or moderately symptomatic with fibroids – observation may allow the treatment to be deferred, perhaps indefinitely. “As women approach menopause, there is limited time for new symptoms and after menopause the bleeding stops and the fibroids decrease in size.” Except for women with Severe anemia from fibroid related menorrhagia Or hydronephrosis from ureteric obstruction from a massively enlarged fibroid uterus
- 29. Risk of malignancy is less than 0.1%. “There is currently no evidence to substantiate performing a hysterectomy for an asymptomatic leiomyoma for the sole purpose of alleviating the concern that it may be malignant.” SOGC CLINICAL PRACTICE GUIDELINES No. 128,May 2003
- 30. GnRH AGONISTS : Treatment reduces the uterine volume, fibroid volume(30%), and bleeding with resultant increase in hemoglobin. Menses return in 4-8weeks after discontinuation, and uterine size returns to pre-treatment levels within 4-6 months SIDE EFFECTS : hot flushes, vaginal dryness, transient frontal headaches, arthralgia, myalgia, insomnia, edema, emotiona l lability, depression, and decreased libido. SURGICAL DRAWBACK S: potential difficulties with enucleation of the myoma and longer intra- operative times, an inability to distinguish and remove smaller myomas at risk to regrow
- 31. “The hypo-estrogenic state induced by GnRH agonists causes significant bone loss after six months of therapy” Low doses of estrogen and progestins may be added in an effort to reduce the side effects and inhibit bone loss and allow long term use. GnRH Agonists as temporary treatment for Peri-menopausal women may be considered.
- 32. GnRH antagonists : (Ganirelix) immediate suppression of endogenous GnRH. Progesterone mediated treatment : Mifepristone (RU 486 ) RISK OF ENDOMETRIAL HYPERPLASIA Progesterone releasing IUD : LNG-IUS may reasonable for selected women with fibroid associated menorrhagia( <12 weeks, regular cavity) Decrease in mean estimated blood loss and increase in hemoglobin but no decrease in uterine volume Progesterone receptor modulators: ASNOPRISNIL
- 33. Serious medical conditions, such as severe anemia or ureteral obstruction, often need to be addressed surgically. Surgical intervention may also be indicated in women who have myomas that are associated with menorrhagia, pelvic pain or pressure, or urinary frequency or incontinence that compromises quality of life. Women with large symptomatic myomas who have completed childbearing are most often recommended to have a hysterectomy.
- 34. Abnormal uterine bleeding not responding to conservative treatments Infertility when there is distortion of the endometrial cavity or tubal obstruction Recurrent pregnancy loss (with distortion of the endometrial cavity) Pain or pressure symptoms (that interfere with quality of life) Urinary tract symptoms (frequency and/or obstruction) Anemia secondary to chronic blood loss High level of suspicion of pelvic malignancy Growth after menopause ACOG, VOL. 104, NO. 2, AUGUST 2004
- 35. Myomectomy should be considered as alternative to hysterectomy . May be considered in women with large fibroids and wish to retain uterus and desire child bearing.
- 36. Pre operative correction of anemia: Iron supplementation Blood transfusion Erythropoietin alfa/ epoetin GnRH Agonist Treatment: mitigate the bleeding Result in increase in hemoglobin.
- 37. MANAGING BLOOD LOSS : Pre operative GnRH agonists treatment Hypotensive anaesthesia Vasopressin(20U in 20 ml NS) - as effective as vascular occlusion for controlling blood loss Tourniquets : Bonney’s myomectomy clamp Ring forceps Elastic rubber catheter(around cervix) Rumel’s Type tourniquet
- 38. Adequate exposure of the operative field. Avoid traumatic instrumentation and injury to the serosa. Sutures on serosal surface should be of fine absorbable non reactive material. Evaluate the size, number and location of myomas, and their proximity to the endocervical canal, uterine vessels, and fallopian tubes. Careful planning of uterine incisions. Aim should be removal of all myomas through a single incision made in anterior uterine corpus and in the midline to avoid vascular areas and broad ligament laterally
- 41. Traditionally used for submucous myomas. When submucous myoma becomes pedunculated myoma can be delivered gradually through the dilated cervix. After satisfactory pre-op. preparation, and broad spectrum antibiotics, vaginal myomectomy should be performed in the operating room. One should avoid too much of downward traction(may cause uterine fundal inversion). Pedicle is identified and clamped as high as possible within the uterine cavity and ligature is applied. In case of brisk bleeding tamponade with inflated Foley’s balloon can be done.
- 42. Mainly for submucous myomas. Successful in treating the menstrual symptoms. Menorrhagia is controlled in 90% patients. Usually performed under laparoscopic guidance to prevent inadvertent perforation. In selected women who are not desirous of future fertility, endometrial ablation may be efficacious in treating abnormal bleeding.
- 44. LESS POST OPERATIVE PAIN, SHORTER HOSPITAL STAY AND SHORTER RECOVERY THAN ABDOMINAL MYOMECTOMY Limitations : Difficult to remove in certain locations. Large or multiple fibroids. When myomas are embedded deep in the myometrium. Retrieval of myomas could be a problem, morcellation may be required Larger myoma can be removed vaginally through a posterior colpotomy incision. Conversion to laparotomy rate 7.5% Complication rate 3.8%
- 49. Significant disadvantage is post- operative pelvic adhesions Overall rate 35 -40% Rate of adhesion per myomectomy site 15 – 20% Rate of adhesion on adnexa 25% Risk factors for adhesion: Use of uterine sutures Posterior uterine wall myomas Prior existence of pelvic adhesions
- 50. A. INTERCEED : Oxidized regenerated cellulose can be placed over uterine corpus to protect the tubes and ovaries from the denuded peritoneal surfaces and uterine incision.
- 51. B. GORE-TEX (Polytetrafluoroethylene surgical membrane) : Non absorbable barrier Can be sutured over the uterine incisions C. SEPRAFILM : Bioresorbable membrane Sodium hyaluronate and carboxymethyl cellulose Reduce the incidence, severity, extent and areas of uterine adhesions after myomectomy. D. GnRH ANALOGUES
- 52. Percutaneous cannulation of femoral artery Embolization of uterine artery and its branches accomplished by injecting gelatin sponges, Poly Vinyl alcohol particles, tris-acryl gelatin microspheres via catheter until occlusion/ or slow flow. Total radiation exposure (approx 5cGy). Effects on early ovarian failure, fertility and pregnancy are unclear. Appropriate candidates for UAE include women who have symptoms severe enough to warrant hysterectomy or myomectomy.
- 55. CONTRAINDICATIONS : Active pelvic infection Severe contraction medium allergy Arteriovenous malformations Desire for future pregnancy Pedunculated myoma Undiagnosed pelvic mass.
- 56. COMPLICATIONS : Post-procedural pain Post embolisation syndrome Early Ovarian Failure(controversial) Effects on Fertility and Pregnancy (possibility of decreased ovarian reserve and potential for increased pregnancy complication, women who wish to conceive should not be treated with UAE)
- 57. Uses high-intensity ultrasound waves that are focused into a small area of between 4 – 16mm, to produce heat and energy, which kills the tumor cells. Concurrent MRI allows precise targeting of the tissue as well as to monitor the temperature of treated tissues Not recommended for women wishing future fertility ADVANTAGES: Very low morbidity Rapid recovery with return to normal life
- 60. Observed in 2.7% - 12.6% of pregnant women EFFECTS OF PREGNANCY: Most do not increase in size during pregnancy. Pregnancy has a variable and unpredictable effect on myoma growth, likely dependent on individual differences in genetics, circulating growth factors, and myoma-localized receptors. A reduction in myoma size was observed 4 weeks after delivery.
- 61. EFFECTS ON PREGNANCY: Very rarely lead to an unfavorable pregnancy outcomes. Cesarean section more common among women with fibroids.(23% Vs 12%) However , there is increases risks of preterm delivery(19.2% Vs 12.7%) Placenta previa(3.5% Vs 1.8%) Post partum hemorrhage(49.1% Vs 21.4%) Malpresentation “Uterine rupture during pregnancy or delivery as a consequence of abdominal myomectomy appears to be rare.”
- 62. Although new myomas may grow after myomectomy, most women will not require additional treatment. Myomas detected after myomectomy, often referred to as recurrence, either are the result of persistence of myomas left at the time of surgery or are newly developed myomas.
- 63. Clinical exam alone may not be effective in assessing the incidence of new appearance of myomas, because women who return to the gynecologist are more likely to have gynecologic problems associated with new myomas than are women who remain asymptomatic
- 64. Routine ultrasound follow-up is sensitive but detects many clinically insignificant myomas. Meaningful information for a woman with myomas considering treatment is her approximate risk of developing symptoms that would require yet additional treatment.
- 65. Age Subsequent childbearing Number of myomas initially removed Gonadotropin-releasing hormone agonists Laparoscopic myomectomy
- 71. Most leiomyomata are asymptomatic.
