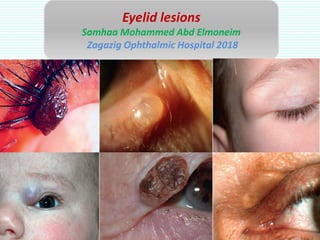
Lid lesions
- 1. Eyelid lesions Samhaa Mohammed Abd Elmoneim Zagazig Ophthalmic Hospital 2018
- 2. Epidermis Keratin layer Granular layer Brickle cell layer Basal layer Dermis Bl vs Lymphatics Fibroblast, CT Macrophage Mast cells Adnexa deep in dermis & tarsus
- 3. Histological terminology Atypia: abnormal appearance of individual cells (abnormal mitosis). Dysplasia: alteration in size, morphology & organization. Hyerkeratosis (increased keratin layer). Dyskeratosis: keratinization other than epidermis. Acanthosis: thickened brickle cell layer. Parakeratosis: retension of nuclei in keratin layer. Carcinoma in situ (intraepidermal carcinoma, Bowen disease).
- 4. General consideration • Epidermal, adenxal or dermal lesion. • Benign lesions (less induration, ulceration, limited growth, uniform color, preservation of lid margin structure, regular outline. • Biopsy is required if it is suspicious. • Incisional/ excisional biopsy. • Excision/ marsuplialization/ laser, cryo ablation. • Suspicion neads total excision with safety margin 3mm
- 5. Benign Cysts (chalazion, zeis, moll, sebaceous , milia, comedone, epidermal inclusion, dermoid) Epidermal (squamous papilloma, seborhoeic keratosis, actinic keratosis) Pigmented (freckle, congenital naevus, acquired melanocytic naevus) Adenxal (syringoma, pilomatricoma) Miscellaneous (capillary hgoma, portwine, pyogenic granuloma, NF, xanthelasma) Malignant BSC SCC, kerato acanthoma. SGC Site Size Surface Surrounding Edges LN
- 6. Small non translucent at ant margin, from lash follicle, obstructed sebaceous gland. (cyst of zeis) Cystic translucent non tender at ant. lid margin. (apocrine hydrocystoma, cyst of Moll)
- 7. Epidermis implantation into dermis, 2ry to trauma, surgery. Firm, nodular SC containing keratin. (Epidemal inclusion cyst) Sequestrated skin during embryonic development, typically attached to periosteum at lateral brow at suture fusion. (Dermoid)
- 8. Tiny, white round papules. Retention of keratin due to blockage of pilosebaceous unit. (Milia) Lipogranuloma, meibomian cyst. Rosacea, blepharitis are association.exclude EOR in children & malignancy in eldery. (Chalazion) Keratin plugs within dilated orifice of follicles in acne . Fulgaris. open (backhead), closed (whitehead) (Comedones)
- 9. Benign Cysts (chalazion, zeis, moll, sebaceous , milia, comedone, epidermal inclusion, dermoid) √ Epidermal (squamous papilloma, seborhoeic keratosis, actinic keratosis) Pigmented (freckle, congenital naevus, acquired melanocytic naevus) Adenxal (syringoma, pilomatricoma) Miscellaneous (capillary hgoma, portwine, pyogenic granuloma, NF, xanthelasma) Malignant BSC SCC, keratoacanthoma SGC Site Size Surface Surrounding Edges LN
- 10. Peduculated, sessile, hyperkeratotic cutaneous horn. Acanthosis, hyperkeratosis. Slowly progressive increase in eldery. HPV. B. (squamous cell papilloma)
- 11. Proliferation of basal layer of epithelium with expansion of squamous epith. Pigmentd ̎ stuck on ̎ appearance. Shave biopsy é cyo, laser, chemical peeling can be done. (Seborrheic keratosis (basal cell papilloma) Slowly progressing in sun damaged skin. Nodular, wart or cutaneous horn. Low potential of malignancy to SCC (carcinoma insitu). Excision or cryo. (Actinic keratosis) Insitu = no penetration of basment membrane of epi thelium / demis
- 12. Benign Cysts (chalazion, zeis, moll, sebaceous , milia, comedone, epidermal inclusion, dermoid) √ Epidermal (squamous papilloma, seborhoeic keratosis, actinic keratosis) √ Pigmented (freckle, congenital naevus, acquired melanocytic naevus) Adenxal (syringoma, pilomatricoma) Miscellaneous (capillary hgoma, portwine, pyogenic granuloma, NF, xanthelasma) Malignant BSC SCC, keratoacanthoma SGC Site Size Surface Surrounding Edges LN
- 13. Increase melanin in epidermal basal layer, increase with sun exposure. (Freckle) Uncommon usually small. Rare variant is kissing/ split naevus, may contain numerous hair. Large one (giant hairy naevus ) has malignant transformation 15%. (Congenital melanocystic naevus)
- 14. Uncommon usually small. Rare variant is kissing/ split naevus, may contain numerous hair. Large one (giant hairy naevus ) has malignant transformation 15%. (Congenital melanocystic naevus)
- 15. Junctional (low malignant potential) Compound (lower) Intrademal (No) Acquired melanocytic naevi
- 16. Benign Cysts (chalazion, zeis, moll, sebaceous , milia, comedone, epidermal inclusion, dermoid) √ Epidermal (squamous papilloma, seborhoeic keratosis, actinic keratosis) √ Pigmented (freckle, congenital naevus, acquired melanocytic naevus) √ Adenxal (syringoma, pilomatricoma) Miscellaneous (capillary hgoma, portwine, pyogenic granuloma, NF, xanthelasma) Malignant BSC SCC, keratoacanthoma SGC Site Size Surface Surrounding Edges LN
- 17. Hair bulb proliferation. Mobile purple hard nodule with/out calcification. (Pilomatricoma) From eccrine sweat gland. Multiple bilateral papules. (Syringioma)
- 18. Unilateral mobile raised bright red lesion, increase with strain. Blanch. Involved skin with strawberry appearance. Systemic association if multiple?. Resolve at 1y. Ttt with steroid injection, BB topical & systemic, surgery. (Capillary haemangioma) Congenital malformation of dermal bl vs. 10% with systemic association as SWS. Well defined facial pink patch. Not blanch. Unilateral with 5th n. Darken with age. Glaucoma screening. Early ttt with laser. (Potwine haemangioma)
- 19. Bl vs, granulation tissue. Tender rapidly growing. Trauma, infection, surgery, idiopathic. (Pyogenic granuloma) Isolated NF in normal individual, plexiform in NF1, S-shaped ptosis. Difficult excision. (plexiform NF) Intracellular lipid. Bil yellowish SC plaques, at medial aspect. (Xanthelasma)
- 20. Benign Cysts (chalazion, zeis, moll, sebaceous , milia, comedone, epidermal inclusion, dermoid) √ Epidermal (squamous papilloma, seborhoeic keratosis, actinic keratosis) √ Pigmented (freckle, congenital naevus, acquired melanocytic naevus) √ Adenxal (syringoma, pilomatricoma) √ Miscellaneous (capillary hgoma, portwine, pyogenic granuloma, NF, xanthelasma) √ Malignant BSC SCC, keratoacanthoma SGC Site Size Surface Surrounding Edges LN
- 21. Nodular Ulcerative Sclerosing • The most common skin malignancy, 90% in head & neck. The most common lid malignancy. Locally malignant. • Inferior, medial, superior, lateral. Medial is the worst. • Arise from basal layer of epith.., extend downward with pallisade arrangemnt of lobules. (BCC) Locally malignant= arise from BM of epi dermis/thelium. Extend downward with surrounded pallisade cell pattern
- 22. • Fair skin, immunesuppresion, eldery. • Rapidly growth, with keratinization, LN. • Well defined DD: BSC. • Actinic keratosis, carcinoma in situ (Bowen), keratoacantoma DD. (SCC) Nodular Ulcerative Cutaneous horn
- 23. • Rare tumor, from meibomian gland, zeis gland. • 5-10% mortality rate. • More in UL • Pale foamy vaculated lipid containing cytoplasm, large hyperchromatic nuclei. • Nodular (DD chalazion). • Pagetoid (DD chronic post blepharitis) (SGC) Nodular Pegatoid
- 24. • Fair skin with sun exposure. • Rapidly growing then regressed over 3m. • Keratin filled crater. • Definte ttt is required. (Keratoacanthoma)
- 25. • Lentigo maligna (melanoma in situ). • MM invading dermis. • Rapidly growing, variable pigmentation, ill defined, ulceration. (lentigo maligna & melanoma) Lentigo maligna Nodular melanoma MM
- 26. Benign Cysts (chalazion, zeis, moll, sebaceous , milia, comedone, epidermal inclusion, dermoid) √ Epidermal (squamous papilloma, seborhoeic keratosis, actinic keratosis) √ Pigmented (freckle, congenital naevus, acquired melanocytic naevus) √ Adenxal (syringoma, pilomatricoma) √ Miscellaneous (capillary hgoma, portwine, pyogenic granuloma, NF, xanthelasma) √ Malignant BSC √ SCC, keratoacanthoma √ SGC √ Site Size Surface Surrounding Edges LN
- 27. Describe DD (B/ M, melanotic/ non) (how to think ??): • Age (BCC, SCC, SGC, MM, KA) • Race (BCC, SCC, actinic Keratosis, basal cell papilloma • Rapid growth, ulcer (BCC, SCC, KA, SGC, MM) • Papillomatous surface (BCC, SCC, SCP, BCP, KA) • Color (pigmented in BCC, BCP, MM) • LN (SCC, SGC, MM) Ulcerative BCC Rare Pdf : • Xeroderma pigmentosa (AR, BCC, SCC, SGC, sun exposed skin damage bird like facies. • Gorlin-Goltz $ (AD, eye, bone, skin, face deformities, medulloblastoma, breast c, lymphoma. • Muir-Torre $ skin, GIT malignancy.
- 28. Describe DD (how to think ??): • Age (BCC, SCC, SGC, MM, KA) • Race (BCC, SCC, actinic Keratosis, basal cell papilloma • Rapid growth, ulcer (BCC, SCC, KA, SGC, MM) • Papillomatous surface (BCC, SCC, SCP, BCP, KA) • Color (pigmented in BCC, BCP, MM) • LN (SCC, SGC, MM) Rare Pdf : • Xeroderma pigmentosa (AR, BCC, SCC, SGC, sun exposed skin damage bird like facies. • Gorlin-Goltz $ (AD, eye, bone, skin, face deformities, medulloblastoma, breast c, lymphoma. • Muir-Torre $ skin, GIT malignancy.
- 30. Merkel cells are for light touch sensation. Rare highly malignant violaceous/ red nodule with intact skin. Difficult Dx. Excision ttt. (Merker cell tumour) Dermal vascular malignant tumour, in HIV & AIDS pt. Associated systemic dis., bluish or red in color. Excision, radiotherapy + ttt cause. (Kaposi sarcoma)
- 33. BCC SCC
- 36. Benign Cysts (chalazion, zeis, moll, sebaceous , milia, comedone, epidermal inclusion, dermoid) √ Epidermal (squamous papilloma, seborhoeic keratosis, actinic keratosis) √ Pigmented (freckle, congenital naevus, acquired melanocytic naevus) √ Adenxal (syringoma, pilomatricoma) √ Miscellaneous (capillary hgoma, portwine, pyogenic granuloma, NF, xanthelasma) √ Malignant BSC √ SCC, keratocanthoma √ SGC √ Site Size Surface Surrounding Edges LN
- 37. Lid defect surgical protocol Partial thickness defect (direct closure, Z, V/Y plasty, flap or graft) Anterior lamellar Posterior lamellar defect Full thickness defect Small defect < 1/3 lid ( direct closure +/- canthyolysis ) Moderate 1/3 -1/2 lid ( Tenzel rotational myocutaneous flap ) Severe > 1/2 lid ( Hughes for LL, Cutler- Beard bridge for UL ) V Severe ( Mustrade cheek rotational flap )
- 38. Surgical videos
