Cranial nerves examination
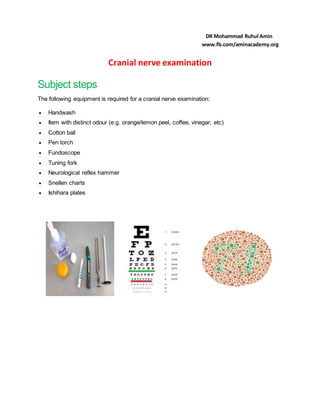
- 1. Cranial nerve examination Subject steps The following equipment is required for a cranial nerve examination: Handwash Item with distinct odour (e.g. orange/lemon peel, coffee, vinegar, etc) Cotton ball Pen torch Fundoscope Tuning fork Neurological reflex hammer Snellen charts Ishihara plates DR Mohammad Ruhul Amin www.fb.com/aminacademy.org
- 2. *Ask the pt to sit edge of the bed,face to face,see any obious findings(ptosisi,squint ,asymmetry,proptosis) Cranial nerve Examination Cranial nerve I 1..Evaluate the patency of the nasal passages bilaterally 2.Do u hv any difficulty in sense of smell. ? (use perfume) 3.Asking the patient to breath in through their nose while the examiner occludes one nostril at a time. Cranial nerve II Visual acuity (with Snellen charts. If the patient normally wears glasses or contact lenses, then this test should be assessed both with and without their vision aids) 1. Stand the patient at 6 metres from the Snellen chart. 2. If patient normally uses distance glasses, ensure they wear them for the assessment. 3. Ask the patient to cover one eye & read to the lowest line they can manage. 4. Visual acuity is recorded as chart distance (numerator) over number of lowest line read (denominator). 5. Record the lowest line the patient was able to read (e.g. 6/6 which is equivalent to 20/20). 6. You can have the patient read through a pinhole to see if this improves vision. 7. Repeat above steps with the other ey Colour vision: Assess colour vision using Ishihara charts Visual fields (Sit directly facing the patient, approximately 1 metre away) 1. Ask the patient to cover their left eye with their left hand. 2. You should cover your left eye and be staring directly at the patient (mirror the patient).
- 3. 3. Ask patient to focus on your face & not move their head or eyes during the assessment. 4. Ask the patient to tell you when they can see your fingertip wiggling. 5. Outstretch your arms, ensuring they are situated at equal distance between yourself & the patient. 6. Position your fingertip at the outer border of one of the quadrants of your visual field. 7. Slowly bring your fingertip inwards, towards the centre of your visual field until the patient sees it. 8. Repeat this process for each quadrant – at 10 o’clock /2 o’clock / 4 o’clock / 8 o’clock. 9. If you are able to see your fingertip but the patient cannot, this would suggest a reduced visual field. 10. Map out any visual field defects you detect. 11. Repeat the same assessment process on the other eye Test for central scotoma: Fundoscopy Preparation 1. Darken the room. 2. The patient should have their pupils dilated with short-acting mydriatic eye drops. 3. Ask the patient to fixate on a distant object 3rd ,4th ,6th nerves 3=eye mov, eye lid move, pupil,size,,symmetry 4=eye move 6=eye move (are involved in movements of the eye) Ptosis,squint: Note any evidence of ptosis – oculomotor nerve pathology Eye movements 1. Ask the patient to keep their head still & follow your finger with their eyes. 2. Move your finger through the various axis of eye movement (“H” shape). 3. Ask the patient to report any double vision.
- 4. 4. Observe for restriction of eye movement & note any nystagmus Cover test 1. Ask patient to focus on a target (e.g. your pen top). 2. Cover one of the patient’s eyes. 3. Observe the uncovered eye for movement: o No movement = normal response o Eye moves temporally = divergent squint o Eye moves nasally = convergent squint 4. Repeat the cover test on the other eye Pupils Size – normal size is approximately 2-4mm in diameter (bright light) Position – assess pupil alignment ,misalignment noted in strabismus Pupillary reflexes Direct reflex– shine torch into eye – look for pupillary constriction in that eye Consensual reflex – shine torch into eye – look for pupillary constriction in opposite eye Swinging light test– move light in from side of each eye rapidly –relative afferent pupillary defect (RAPD Accommodation reflex: 1. Ask patient to focus on a distant point (clock on a wall / light switch). 2. Place your finger/object approximately 15cm in front of the eyes. 3. Ask the patient to switch from looking at the distant object to the nearby finger / object. 4. Observe the pupils, you should see constriction & convergence bilaterally (involved in sensory supply to the face and motor supply to the muscles of mastication)
- 5. The Trigeminal nerve (CN V) -facial sense -corneal ref -taste Sensory test: 3 division of nerves, Corneal reflex ** motor test: ask the patient to clench their teeth together, observing and feeling the bulk of the masseter and temporalis muscle **open their mouth against resistance ** perform the jaw jerk The Facial nerve (CN VII) supplies motor branches to the muscles of facial expression Sensory test: Ant 2/3rd of tongue-taste Post 1/3rd of tongue-through glossoph nerve Finally-external auditory meatus –ramsay hunt syndrome and hyperacusis the Vestibulocochlear nerve (CN VIII) Vestibulardivision:vertigo,dizziness,giddiness Cochleardicvision: Ext ear-wax ,rash Rub fingers The Glossopharyngeal nerve (CN IX) g-gag reflex provides sensory supply to the palate. It can be tested with the gag reflex or by touching the arches of the pharynx.
- 6. The Vagus nerve (CN X) provides motor supply to the pharynx-palate ele vation the Accessory nerve (CN XI) gives motor supply to the sternocleidomastoid and trapeziusmuscles. To test it, ask the patient to shrug their shoulders and turn their head against resistance. The Hypoglossal nerve (CN XII) . provides motor supply to the muscles of the tongue
