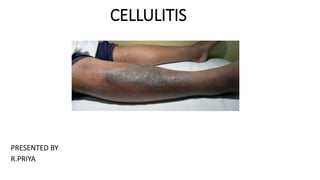
Cellulitis
•Transferir como PPTX, PDF•
7 gostaram•7,050 visualizações
Cellulitis is a bacterial infection of the deep dermis and subcutaneous tissue. It is most commonly caused by S. pyogenes and S. aureus.5 Bacteria may gain access to the dermis via a break in the skin barrier in healthy adults, whereas the hematogenous route is more common in immunocompromised patients. The affected skin is usually erythematous, swollen, painful, and warm to the touch. Severe cellulitis can be complicated by bullae, pustules, or necrotic tissue. Damage to lymphatic vessels can lead to recurrent episodes of cellulitis.6 In areas of the world endemic for lymphatic filariasis, it is important to rule out this disease in cases of recurrent bouts of lower-extremity cellulitis and lymphangitis.
Denunciar
Compartilhar
Denunciar
Compartilhar
Recomendados
Recomendados
Mais conteúdo relacionado
Mais procurados
Mais procurados (20)
Pyelonephritis, ACUTE PYELONEPHRITIS, CHRONIC PYELONEPHRITIS, 

Pyelonephritis, ACUTE PYELONEPHRITIS, CHRONIC PYELONEPHRITIS,
Semelhante a Cellulitis
Semelhante a Cellulitis (20)
Mais de Priya
Mais de Priya (20)
Último
Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Escort ServiceModels Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...

Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...GENUINE ESCORT AGENCY
🌹Attapur⬅️ Vip Call Girls Hyderabad 📱9352852248 Book Well Trand Call Girls In Hyderabad Escorts Service
Escorts Service Available
Whatsapp Chaya ☎️ : [+91-9352852248 ]
Escorts Service Hyderabad are always ready to make their clients happy. Their exotic looks and sexy personalities are sure to turn heads. You can enjoy with them, including massages and erotic encounters.#P12Our area Escorts are young and sexy, so you can expect to have an exotic time with them. They are trained to satiate your naughty nerves and they can handle anything that you want. They are also intelligent, so they know how to make you feel comfortable and relaxed
SERVICE ✅ ❣️
⭐➡️HOT & SEXY MODELS // COLLEGE GIRLS HOUSE WIFE RUSSIAN , AIR HOSTES ,VIP MODELS .
AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME
★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE
★
SATISFACTION,UNLIMITED ENJOYMENT.
★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE PROFILes Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & HOTEL Star Hotel Service .In Call & Out call
SeRvIcEs :
★ A-Level (star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without condom
★ANAL SERVICES.
🌹Attapur⬅️ Vip Call Girls Hyderabad 📱9352852248 Book Well Trand Call Girls In...

🌹Attapur⬅️ Vip Call Girls Hyderabad 📱9352852248 Book Well Trand Call Girls In...Call Girls In Delhi Whatsup 9873940964 Enjoy Unlimited Pleasure
9630942363 THE GENUINE ESCORT AGENCY VIP LUXURY CALL GIRLS
HIGH CLASS MODELS CALL GIRLS GENUINE ESCORT BOOK
BOOK APPOINTMENT - 9630942363 THE GENUINE ESCORT AGENCY
BEST VIP CALL GIRLS & ESCORTS SERVICE 9630942363 VIP CALL GIRLS ALL TYPE WOMEN AVAILABLE
INCALL & OUTCALL BOTH AVAILABLE BOOK NOW
9630942363 VIP GENUINE INDEPENDENT ESCORT AGENCY
VIP PRIVATE AUNTIES
BEAUTIFUL LOOKING HOT AND SEXT GIRLS AND PARTY TYPE GIRLS YOU WANT SERVICE THEN CALL THIS NUMBER 9630942363
ROOM ALSO PROVIDE HOME & HOTELS SERVICE
FULL SAFE AND SECURE WORK
WITHOUT CONDOMS, ORAL, SUCKING, LIP TO LIP, ANAL, BACK SHOTS, SEX 69, WITHOUT BLOWJOB AND MUCH MORE
FOR BOOKING
9630942363Call Girls Ahmedabad Just Call 9630942363 Top Class Call Girl Service Available

Call Girls Ahmedabad Just Call 9630942363 Top Class Call Girl Service AvailableGENUINE ESCORT AGENCY
Último (20)
Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...

Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...
Andheri East ) Call Girls in Mumbai Phone No 9004268417 Elite Escort Service ...

Andheri East ) Call Girls in Mumbai Phone No 9004268417 Elite Escort Service ...
Model Call Girls In Chennai WhatsApp Booking 7427069034 call girl service 24 ...

Model Call Girls In Chennai WhatsApp Booking 7427069034 call girl service 24 ...
All Time Service Available Call Girls Marine Drive 📳 9820252231 For 18+ VIP C...

All Time Service Available Call Girls Marine Drive 📳 9820252231 For 18+ VIP C...
Independent Call Girls Service Mohali Sector 116 | 6367187148 | Call Girl Ser...

Independent Call Girls Service Mohali Sector 116 | 6367187148 | Call Girl Ser...
Top Rated Hyderabad Call Girls Erragadda ⟟ 9332606886 ⟟ Call Me For Genuine ...

Top Rated Hyderabad Call Girls Erragadda ⟟ 9332606886 ⟟ Call Me For Genuine ...
Call Girls Service Jaipur {8445551418} ❤️VVIP BHAWNA Call Girl in Jaipur Raja...

Call Girls Service Jaipur {8445551418} ❤️VVIP BHAWNA Call Girl in Jaipur Raja...
Call Girls Rishikesh Just Call 9667172968 Top Class Call Girl Service Available

Call Girls Rishikesh Just Call 9667172968 Top Class Call Girl Service Available
Call Girls Hosur Just Call 9630942363 Top Class Call Girl Service Available

Call Girls Hosur Just Call 9630942363 Top Class Call Girl Service Available
Call Girls Hyderabad Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Hyderabad Just Call 8250077686 Top Class Call Girl Service Available
Call Girls Service Jaipur {9521753030 } ❤️VVIP BHAWNA Call Girl in Jaipur Raj...

Call Girls Service Jaipur {9521753030 } ❤️VVIP BHAWNA Call Girl in Jaipur Raj...
🌹Attapur⬅️ Vip Call Girls Hyderabad 📱9352852248 Book Well Trand Call Girls In...

🌹Attapur⬅️ Vip Call Girls Hyderabad 📱9352852248 Book Well Trand Call Girls In...
Jogeshwari ! Call Girls Service Mumbai - 450+ Call Girl Cash Payment 90042684...

Jogeshwari ! Call Girls Service Mumbai - 450+ Call Girl Cash Payment 90042684...
Independent Call Girls In Jaipur { 8445551418 } ✔ ANIKA MEHTA ✔ Get High Prof...

Independent Call Girls In Jaipur { 8445551418 } ✔ ANIKA MEHTA ✔ Get High Prof...
Call Girls Kolkata Kalikapur 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Girl Se...

Call Girls Kolkata Kalikapur 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Girl Se...
Call Girls Ahmedabad Just Call 9630942363 Top Class Call Girl Service Available

Call Girls Ahmedabad Just Call 9630942363 Top Class Call Girl Service Available
Coimbatore Call Girls in Coimbatore 7427069034 genuine Escort Service Girl 10...

Coimbatore Call Girls in Coimbatore 7427069034 genuine Escort Service Girl 10...
Most Beautiful Call Girl in Bangalore Contact on Whatsapp

Most Beautiful Call Girl in Bangalore Contact on Whatsapp
Russian Call Girls Lucknow Just Call 👉👉7877925207 Top Class Call Girl Service...

Russian Call Girls Lucknow Just Call 👉👉7877925207 Top Class Call Girl Service...
(Low Rate RASHMI ) Rate Of Call Girls Jaipur ❣ 8445551418 ❣ Elite Models & Ce...

(Low Rate RASHMI ) Rate Of Call Girls Jaipur ❣ 8445551418 ❣ Elite Models & Ce...
Cellulitis
- 2. INTRODUCTION Skin is the largest organ of human body. Skin is first line of defence system of human body. It forms a barrier and protects internal organs from external foreign bodies including bacteria, viruses, fungi etc. Skin has three layers- Dermis, Epidermis and Hypodermis. The tissue beneath the skin is called Subcutaneous tissue. This consists of fats and collagen which regulate body temperature and protect the body. Normally there are many types of bacteria on skin which may enter our body through cracks, breaks, cuts, injuries, ulcers etc. They can then multiply and spread to cause infection of skin called Ceulitis.
- 3. DEFINITION Cellulitis is a bacterial infection involving the inner layers of the skin.[1] It specifically affects the dermis and subcutaneous fat Cellulitis may spread rapidly. Affected skin appears swollen and red and may be hot and tender. Without treatment with an antibiotic, cellulitis can be life-threatening. Cellulitis usually affects the skin on the lower legs, but it can occur in the face, arms and other areas. It occurs when a crack or break in your skin allows bacteria to enter.
- 4. TYPES Typical presentation of all skin infections •Soft tissue redness •Warmth and swelling •Pain/tenderness Mild Cellulitis •Features above •No systemic features •No significant co-morbidities Moderate Cellulitis •Features above with moderate swelling and tenderness •Systemic features (eg fever, tachycardia) Severe Cellulitis •Features above with severe swelling or tenderness •Large body surface area involved (eg larger than the patient’s handprint) •Marked systemic features (eg fever or hypothermia, tachycardia, tachypnoea, altered conscious state, unwell appearance, hypotension — this is a late sign). See Sepsis Features suggestive of necrotising fasciitis include: •severe pain out of keeping with apparent severity of infection •rapid progression •marked systemic features (eg high fever with rigors, tachycardia, tachypnoea, hypotension, confusion, vomiting). See Sepsis
- 5. CAUSES Cellulitis is caused by bacteria that enter and infect the tissue through breaks in the skin. GroupA Streptococcus and Staphylococcus are the most common causes of the infection and may be found on the skin as normal flora in healthy individuals. Insect or spider bite, blistering, an animal bite, tattoos, pruritic (itchy) skin rash, recent surgery, athlete's foot, dry skin, eczema, injecting drugs (especially subcutaneous or intramuscular injection or where an attempted intravenous injection "misses" or blows the vein),
- 6. RISK FACTOR •The most common causes are Group A streptococcus (GAS) and Staphylococcus aureus. Impetigo (commonly called "school sores") •Highly contagious infection of the epidermis, particularly common in young children Causative organisms are GAS and S. aureus •May be associated with scabies Staphylococcal scalded skin syndrome (SSSS) •Blistering skin disorder induced by the exfoliative (epidermolytic) toxins of S. aureus. Primarily affects neonates and young children Necrotising fasciitis •Rapidly progressive soft tissue infection characterised by necrosis of subcutaneous tissue •Causative organisms include GAS, S. aureus, anaerobes and is often polymicrobial •It causes severe illness with a high mortality rate (~25%) •Recent infection with varicella is a risk factor
- 7. RISK FACTOR •Injury. Any cut, fracture, burn or scrape gives bacteria an entry point. •Weakened immune system. Conditions that weaken your immune system — such as diabetes, leukemia and HIV/AIDS — leave you more susceptible to infections. Certain medications also can weaken your immune system. •Skin conditions. Conditions such as eczema, athlete's foot and shingles can cause breaks in the skin, which give bacteria an entry point. •Chronic swelling of your arms or legs (lymphedema). This condition sometimes follows surgery. •History of cellulitis. Having had cellulitis before makes you prone to develop it again. •Obesity. Being overweight or obese increases your risk of developing cellulitis. • suffered poliomyelitis • Chickenpox and shingles often result in blisters that break open, providing a gap in the skin through which bacteria can enter. • Lymphedema, which causes swelling on the arms and/or legs, can also put an individual at risk. • Predisposing factors include skin abrasions, lacerations, burns, eczematous skin, chickenpox, etc. although the portal of entry of organisms is often not seen
- 9. SIGNS AND SYMPTOMS •Red area of skin that tends to expand •Swelling •Tenderness •Pain •Warmth •Fever •Red spots •Blisters •Skin dimpling
- 10. DIAGNOSTIC EVAUATION History Physical examination use of bedside ultrasonography blood cultures are positive in fewer than 5% of all cases •Swab for Gram stain (charcoal / gel / bacterial transport swab and slide) and culture if discharge present •Blood culture is not useful in mild/moderate cellulitis •Consider imaging (eg ultrasound) if abscess, deep infection or foreign body suspected
- 11. MANAGEMENT •Covering your wound. Properly covering the affected skin will help it heal and prevent irritation. Follow your doctor’s instructions for dressing your wound and be sure to change your bandage regularly. •Keeping the area clean. Follow your doctor’s recommendations for cleaning the affected skin. •Elevating the affected area. If your leg is affected, lie down and elevate your leg above your heart. This will help reduce swelling and ease your pain. •Applying a cool compress. If the affected skin is hot and painful, apply a clean washcloth soaked in cool water. Avoid chemical icepacks, as these can further irritate damaged skin.
- 12. MANAGEMENT
- 13. COMPLICATION Recurrent episodes of cellulitis may damage the lymphatic drainage system and cause chronic swelling of the affected limb. Rarely, the infection can spread to the deep layer of tissue called the fascial lining. Necrotizing fasciitis is an example of a deep-layer infection. It's an extreme emergency.
- 14. PREVENTION •Wash your wound daily with soap and water. Do this gently as part of your normal bathing. •Apply a protective cream or ointment. For most surface wounds, an over-the-counter ointment (Vaseline, Polysporin, others) provides adequate protection. •Cover your wound with a bandage. Change bandages at least daily. •Watch for signs of infection. Redness, pain and drainage all signal possible infection and the need for medical evaluation. People with diabetes and those with poor circulation need to take extra precautions to prevent skin injury. Good skin care measures include the following: •Inspect your feet daily. Regularly check your feet for signs of injury so you can catch infections early. •Moisturize your skin regularly. Lubricating your skin helps prevent cracking and peeling. Do not apply moisturizer to open sores. •Trim your fingernails and toenails carefully. Take care not to injure the surrounding skin. •Protect your hands and feet. Wear appropriate footwear and gloves. •Promptly treat infections on the skin's surface (superficial), such as athlete's foot. Superficial skin infections can easily spread from person to person. Don't wait to start treatment.