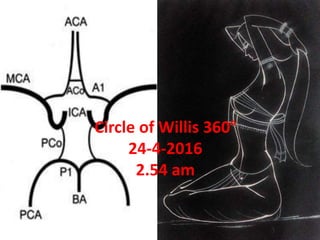
Circle of willis 360°
- 1. Circle of Willis 360° 24-4-2016 2.54 am
- 2. Great teachers – All this is their work . I am just the reader of their books . Prof. Paolo castelnuovo Prof. Aldo Stamm Prof. Mario Sanna Prof. Magnan
- 3. For Other powerpoint presentatioins of “ Skull base 360° ” I will update continuosly with date tag at the end as I am getting more & more information click www.skullbase360.in - you have to login to slideshare.net with Facebook account for downloading.
- 4. Circle of willis in anterior & lateral skull base view ??? is intracerebral carotid
- 6. In anterior skull base approach
- 7. Middle cranial fossa approach
- 8. In anterior skull base approach - Type C Modified Transcochlear Approach – after cutting the tentorium With mild retraction of the temporal lobe, the bifurcation of the internal carotid artery (ICA) into the anterior (ACA) and middle cerebral (MCA) arteries is seen. The ipsilateral (ON) and contralateral (ONc) optic nerves are seen. The oculomotor nerve (III) is embraced by the posterior cerebral artery (PCA) superiorly and the superior cerebellar artery (SCA) inferiorly
- 9. http://www.ajnr.org/content/27/8/1770/F2.expansion.html Classification of the anatomic variations in the circle of Willis. In the “textbook” type, both the precommunicating segment of the anterior cerebral artery (A1) and that of the posterior cerebral artery (P1) were normal in size. The next group included both right and left A1 hypoplasia. Because no significant difference between cerebral arteries on the right and left sides has been established,5,18 we combined right and left A1 hypoplasia into A1 hypoplasia. The next group included right and left P1 hypoplasia, which again were treated as a single category, P1 hypoplasia. “Other” type included a combination of A1 hypoplasia and P1 hypoplasia, bilateral P1 hypoplasia, as well as other unclassified variations. ACA indicates anterior cerebral artery; ACo, anterior communicating artery; MCA, middle cerebral artery; ICA, internal cerebral artery; PCo, posterior communicating artery; PCA, posterior cerebral artery; BA, basilar artery
- 10. http://www.ajnr.org/content/27/8/1770/F3.expansion.html Relative contribution of proximal arteries to total volume flow in variations in the circle of Willis. Values signify mean percentage ± SD. The upper left value corresponds to the relative contribution of the right internal carotid artery in the “textbook” type or of the internal carotid artery ipsilateral to hypoplastic A1 or P1 in the other variations. The upper right value corresponds to the relative contribution of the left internal carotid artery in the “textbook” type, or of the internal carotid artery contralateral to hypoplastic A1 or P1 in the other variations. The value at the bottom corresponds to the relative contribution of the basilar artery. * The value for A1 hypoplasia variation was significantly smaller than those for “textbook” type and P1 hypoplasia variation. The value for P1 hypoplasia variation was significantly larger than that for “textbook” type. ** The value for A1 hypoplasia variation was significantly larger than that for “textbook” type. *** The value for P1 hypoplasia variation was significantly smaller than that for “textbook” type.
- 11. http://stroke.ahajournals.org/content/30/12/2671/F2.expansion.html Scheme of anatomic variations of the posterior part of the CW: variant types a through c are complete, whereas the remainder are incomplete. a, Bilateral PCoA present. b, PCA originating predominantly from the ICA. This type is known as a unilateral fetal-type PCA (FTP), indicated by the arrows; the PCoA on the other side is present. c, Bilateral FTP, with both P1 segments patent. d, Unilateral PCoA present. e, Hypoplasia or absence of both PCoAs, with isolation of the anterior and posterior circle parts at this level. f, Unilateral FTP, with hypoplasia or absence of the P1 segment. g, Unilateral FTP, with hypoplasia or absence of the contralateral PCoA. h, Unilateral FTP, with hypoplasia or absence of the P1 and PCoA. i, Bilateral FTP, with hypoplasia or absence of both P1 segments. j, Bilateral FTP, with hypoplasia or absence of one P1 segment.
- 12. Pcom absent in post- craniopharyngioma case
- 14. Cisternal / Intracranial ICA [ICA i]
- 15. Anatomically speaking, the paraclinoid segment of the internal carotid artery is not fully intracavernous, and it is separated from the cavernous sinus by the extension of the dura covering the inferior surface of the anterior clinoid process (Reisch et al. 2002 ) . Note carotid cave , cavernous sinus , upper & lower dural rings
- 16. Oculomotor cistern Cranial nerve III enters the roof included in its own cistern (oculomotor cistern). Oculomotor cistern goes upto anterior clinoid tip
- 17. The mOCR is located just medial to the paraclinoidal-supraclinoidal ICA transition and inferior to the distal cisternal segment of the ON(Labib et al. 2013 ). Cl clivus, ICAc cavernous portion of the internal carotid artery, ON optic nerve, PG pituitary gland, PS planum sphenoidale, TS tuberculum sellae, yellow asterisks upper dural ring, blue arrowheads lower dural ring, white asterisk lateral optico-carotid recess, white circle medial optico-carotid recess, white arrow ophthalmic artery, black arrows middle clinoid process, red arrows lateral tubercular crest, yellow arrows endocranial region corresponding to MCP
- 18. Cadaveric dissection image demonstrating the close anatomical relationship of the posterior clinoid (PC) with both the intracranial carotid artery (ICCA) and the posterior genu of the intracavernous carotid artery (P. CCA). AL, anterior lobe of the pituitary gland; PL, posterior lobe of the pituitary gland; BA, basilar artery. green dotted triangle area for entry of the endoscope into the interpeduncular fossa
- 19. Posterior clinoidectomy in cisternostomy in head injury video – by Dr. Iype Cherian - click https://www.youtube.com/watch?v =vNaEFMrdgfw
- 20. Aneurysms of initial intracranial carotid
- 21. Opthalmic artery – Retrograde branch of Intracranial carotid Branches of the cavernous internal carotid artery ( ICA ), a rare variation: ophthalmic artery passing through the superior orbital fissure
- 22. In the lateral border of the chiasmatic cistern the first part of the ICAi is visible. Note Optic tract here which is above Posterior clinoid process [ PCP ]
- 23. In the lateral border of the chiasmatic cistern the first part of the ICAi is visible. Dry bone dissection image taken with a 30-degree endoscope demonstrating the fovea ethmoidalis (FE) and cribriform plate (CP) junction with the planum sphenoidale (PS). This is marked approximately by the posterior ethmoidale artery (PEA). ISS, intersinus septum of sphenoid sinus; ON, optic nerve; CCA, anterior genu of the intracavernous carotid artery.
- 24. Supra-clinoidal carotid=1st part of intracranial carotid
- 25. APAs anterior perforating arteries, ICAi intracranial portion of the internal carotid artery, OT optic tract, SF Sylvian fi ssure,
- 26. A 1 [ ACA ] crosses above the Optic tract , not Optic nerve . Left subchiasmatic cistern
- 27. ACA anterior cerebral artery, APAs anterior perforating arteries, FOA fronto-orbital artery, FOV fronto-orbital vein, FPA fronto-polar artery, ICAi intracranial segment of the internal carotid artery, MCA middle cerebral artery, OlfT olfactory tract, OlfV olfactory vein, ON optic nerve, PS pituitary stalk, TL temporal lobe, black asterisk anterior communicating artery
- 28. ICA dividing into ACA and MCA
- 29. Optic tract [ OT ]
- 33. Fig. 2.1 Drawing showing the skin incision (red line), the craniotomy and the microsurgical intraoperative view of the subfrontal unilateral approach. This approach provides a wide intracranial exposure of the frontal lobe and easy access to the optic nerves, the chiasm, the carotid arteries and the anterior communicating complex
- 34. Fig. 2.4 Intraoperative microsurgical photograph showing contralateral extension of the tumor (T) dissected via a unilateral subfrontal approach. Note on the left side the falx cerebri (F) and the mesial surface of the left frontal lobe (FL)
- 35. Fig. 2.5 Drawing showing the skin incision (red line), the craniotomy and the microsurgical anatomic view of the subfrontal bilateral route. This approach provides a wide symmetrical anterior cranial fossa exposure and easy access to the optic nerves, the chiasm, the carotid arteries and the anterior communicating arteries complex
- 36. Supraorbital approach - Fig. 3.2 Illustrations comparing the incision and bony exposure in a supraorbital craniotomy with those in a pterional craniotomy. a The supraorbital craniotomy utilizes the subfrontal corridor and involves a frontobasal burr hole and removal of a small window in the frontal bone. b The pterional craniotomy utilizes a frontotemporal incision and removal of the frontal and temporal bones andsphenoid wing. The pterional craniotomy primarily exploits the sylvian fissure
- 38. Fig. 4.6 a Craniotomy. b When the flap has been removed the lesser wing of the sphenoid is drilled down to optimize the most basal trajectory to the skull base. c Dural opening. DM dura mater, FL frontal lobe, MMA middle meningeal artery, LWSB lesser wing of the sphenoid bone, SF sylvian fissure, TL temporal lobe, TM temporal muscle, ZPFB zygomatic process of the frontal bone
- 39. Fig. 4.8 Intradural exposure; right approach. Before (a) and after (b) opening of the Sylvian fissure. A1 first segment of the anterior cerebral artery, AC anterior clinoid, FL frontal lobe, HA Heubner’s artery, I olfactory tract, III oculomotor nerve, ICA internal carotid artery, LT lamina terminalis, M1 first segment of the middle cerebral artery, MPAs perforating arteries, ON optic nerve, P2 second segment of the posterior cerebral artery, PC posterior clinoid, PcoA posterior communicating artery, SF sylvian fissure, TL temporal lobe, TS tuberculum sellae
- 40. Fig. 4.9 Intradural exposure; right approach. a Instruments enlarging the optocarotid area. b Displacing medially the posterior communicating artery, exposing the contents of the interpeduncular cistern. AC anterior clinoid, AchA anterior choroidal artery, BA basilar artery, FL frontal lobe, ICA internal carotid artery, III oculomotor nerve, OA left ophthalmic artery, ON optic nerve, OT optic tract, P2 second segment of the posterior cerebral artery, PC posterior clinoid, PcoA posterior communicating artery, Ps pituitary stalk, SCA superior cerebellar artery, SHA superior hypophyseal artery, TE tentorial edge, TL temporal lobe
- 41. Fig. 4.10 Intradural exposure; right approach; enlarged view. A1 first segment of the anterior cerebral artery, A2 second segment of the anterior cerebral artery, AC anterior clinoid, AcoA anterior communicating artery, BA basilar artery, FL frontal lobe, HA Heubner’s artery, ICA internal carotid artery, III oculomotor nerve, LT lamina terminalis, M1 first segment of the middle cerebral artery, OA left ophthalmic artery, ON optic nerve, P2 second segment of the posterior cerebral artery, PC posterior clinoid, PcoA posterior communicating artery, SCA superior cerebellar artery, SHA superior hypophyseal artery, TE tentorial edge, TL temporal lobe, TS tuberculum sellae
- 42. Posteior clinoid can be approached in optico-carotid triangle [ 3mm ] OR lateral carotid triangle
- 43. Posteior clinoid can be approached in optico-carotid triangle [ 3mm ] OR lateral carotid triangle
- 44. Pcom is seen in optico-carotid triangle – can be injured in cisternostomy while cutting lillequet membrane
- 45. Fig. 4.11 Intradural exposure; right approach; close-up view ofthe interpeduncular fossa. AchA anterior choroidal artery, BAbasilar artery, DS dorsum sellae, III oculomotor nerve, IV trochlear nerve, P1 first segment of the posterior cerebral artery,P2 second segment of the posterior cerebral artery, PC posteriorclinoid, PcoA posterior communicating artery, Ps pituitary stalk, SCA superior cerebellar artery, TE tentorial edge
- 46. Endoscope-assisted microsurgery [ 45° endoscope in a corridor between the carotid artery and the oculomotor nerve ]-- Fig. 4.12 Intradural exposure; right approach; microsurgical (a) and endoscopic (b–d) views. AchA anterior choroidal artery, BA basilar artery, C clivus, FL frontal lobe, ICA internal carotid artery, III oculomotor nerve, ON optic nerve, P1 first segment of the posterior cerebral artery, P2 second segment of the posterior cerebral artery, PC posterior clinoid, PCA posterior cerebral artery, PcoA posterior communicating artery, SCA superior cerebellar artery, TE tentorial edge, TL temporal lobe, Tu thalamoperforating artery; green dotted triangle area for entry of the endoscope into the interpeduncular fossa
- 47. Cadaveric dissection image demonstrating the close anatomical relationship of the posterior clinoid (PC) with both the intracranial carotid artery (ICCA) and the posterior genu of the intracavernous carotid artery (P. CCA). AL, anterior lobe of the pituitary gland; PL, posterior lobe of the pituitary gland; BA, basilar artery. green dotted triangle area for entry of the endoscope into the interpeduncular fossa
- 48. Fig. 4.12 Intradural exposure; right approach; microsurgical (a) and endoscopic (b–d) views. AchA anterior choroidal artery, BA basilar artery, C clivus, FL frontal lobe, ICA internal carotid artery, III oculomotor nerve, ON optic nerve, P1 first segment of the posterior cerebral artery, P2 second segment of the posterior cerebral artery, PC posterior clinoid, PCA posterior cerebral artery, PcoA posterior communicating artery, SCA superior cerebellar artery, TE tentorial edge, TL temporal lobe, Tu thalamoperforating artery; green dotted triangle area for entry of the endoscope into the interpeduncular fossa
- 49. Fig. 4.13 Intradural exposure; right approach; microsurgical (a) and endoscopic omolateral (b) and contralateral (c) views. A1 first segment of the anterior cerebral artery, AC anterior clinoid, ICA internal carotid artery, FL frontal lobe, III oculomotor nerve, LT lamina terminalis, M1 first segment of the middle cerebral artery, OA left ophthalmic artery, ON optic nerve, PcoA posterior communicating artery, SHA superior hypophyseal artery, TE tentorial edge, TS tuberculum sellae
- 50. Fig. 4.13 Intradural exposure; right approach; microsurgical (a) and endoscopic omolateral (b) and contralateral (c) views. A1 first segment of the anterior cerebral artery, AC anterior clinoid, ICA internal carotid artery, FL frontal lobe, III oculomotor nerve, LT lamina terminalis, M1 first segment of the middle cerebral artery, OA left ophthalmic artery, ON optic nerve, PcoA posterior communicating artery, SHA superior hypophyseal artery, TE tentorial edge, TS tuberculum sellae
- 52. Pterional
- 67. https://www.scienceopen.com/document_file/84699ab2-4980-4f70-a5b0- c8d95a1fb6a2/PubMedCentral/84699ab2-4980-4f70-a5b0-c8d95a1fb6a2.pdf FIGURE 4. The capsule of the cystic craniopharyngioma was firmly attached to the left hypothalamus, the stalk was dislocated to the right side (Patient 6). The outgrowth of the craniopharyngioma from proximal stalk is recognizable A. Complete removal of the capsule was possible, but produced subpial blood injection over the left hypothalamic surface B. MRI scan revealed a small ischemic injury in the left hypothalamus C. This patient had transient sleep disorder, moderate hyperphagia and memory problems (see also a supplemented video material 1).
- 68. FIGURE 2. In this cystic craniopharyngioma (Patient 5), the stalk was centrally infiltrated close to the pituitary and could not be preserved A. The incipient third ventricle entrance is seen from intracavitary view. The slit into the third ventricle is still covered with tumour capsule B. Complete removal of the capsule opened the third ventricle C. Petehiae in the hypothalamus bilaterally resulted from apparently gentle traction and blunt dissection of the capsule away from the hypothalamus D. Psychoorganic change, disorientation and memory deficits were noticed in less than a week after surgery, the transient sleep disorder become apparent in the second week postoperatively (see also a supplemented video material 2).
- 69. FIGURE 3. Large craniopharyngioma (Patient 3) produced unilateral hydrocephalus by obstructing the right formen of Monro A. The dome was filled with soft cholesterine cristals B, which were easily removed. Lower limbus of the right foramen of Monro is seen through the empty third ventricle D. Despite bilateral preservation of anteromedial hypothalamus C and stalk preservation E, the patient developed panhypopituitarism and diabetes insipidus with long lasting psychoorganic change
- 70. Fronto-temporal orbitozygomatic transcavernous approach COM= Caratico-occulomotor membrane , DR = dural ring
- 74. Fig. 4.15 Microsurgical view; extradural anterior clinoidectomy. a Exposure and drilling of the anterior clinoid process and optic canal under microscope magnification. b Widened space after complete removal of the AC. AC anterior clinoid, eON extracranial intracanalar optic nerve, FD frontal dura, ICA internal carotid artery, iON intraorbital optic nerve, LWSB lesser wing of sphenoid bone, OC optic canal, OR orbit roof, SOF superior orbital fissure, TD temporal dura
- 75. Fig. 4.16 Microsurgical view; intradural anterior clinoidectomy. a, b After the dura above the anterior clinoid process has been transected in a “T” shape (a), we usually drill always parallel tothe optic nerve and to the carotid artery (b). c The distal ring is finally exposed. A1 precommunicating anterior cerebral artery, AC anterior clinoid, AchA anterior choroid artery, Ch optic chiasm, DR distal ring, fl falciform ligament, FL frontal lobe, ICA internal carotid artery, M1 first tract of the middle cerebral artery, ON optic nerve, PC posterior clinoid, PCOA posterior communicating artery, TS tuberculum sellae
- 76. Fig. 4.16 Microsurgical view; intradural anterior clinoidectomy. a, b After the dura above the anterior clinoid process has been transected in a “T” shape (a), we usually drill always parallel tothe optic nerve and to the carotid artery (b). c The distal ring is finally exposed. A1 precommunicating anterior cerebral artery, AC anterior clinoid, AchA anterior choroid artery, Ch optic chiasm, DR distal ring, fl falciform ligament, FL frontal lobe, ICA internal carotid artery, M1 first tract of the middle cerebral artery, ON optic nerve, PC posterior clinoid, PCOA posterior communicating artery, TS tuberculum sellae
- 78. FTOZ – Fronto-temporal orbitozygomatic approach
- 79. FTOZ – Fronto-temporal orbitozygomatic approach
- 81. Fig. 7.13 a Intraoperative photograph shows good exposure of the left tentorial anterior and middle incisura obtained through the pretemporal and subtemporal corridors. In this patient the basilar apex is well above the superior margin of the dorsum sellae. b Same patient. A more lateral exposure showing the pontomesencephalic junction surface and the neurovascular structures in the ambient cistern. c Intraoperative photograph of another patient showing structures in the left lateral incisural space from the subtemporal corridor. d Same patient. More lateral view. e Same patient. More posterior exposure. The lifting of the free edge of the tentorium shows the trochlear nerve entering the tentorium. The junction between the P2a and P2p segments (P2a, P2p) of the posterior cerebral artery is shown. ACA anterior cerebral artery, AChA anterior choroidal artery and tiny perforating vessels, BA basilar artery, DS dorsum sellae, FET free edge of tentorium, ICA internal carotid artery, LM Liliequist’s membrane, LON left optic nerve, ON oculomotor nerve, OT optic tract, PCA posterior cerebral artery, PComA posterior communicating artery, PLChA posterolateral choroidal artery arising from the P2a–P2p junction, PS pituitary stalk, RON right optic nerve, SCA superior cerebellar artery, TN trochlear nerve in the arachnoidal covering
- 82. Fig. 7.13 a Intraoperative photograph shows good exposure of the left tentorial anterior and middle incisura obtained through the pretemporal and subtemporal corridors. In this patient the basilar apex is well above the superior margin of the dorsum sellae. b Same patient. A more lateral exposure showing the pontomesencephalic junction surface and the neurovascular structures in the ambient cistern. c Intraoperative photograph of another patient showing structures in the left lateral incisural space from the subtemporal corridor. d Same patient. More lateral view. e Same patient. More posterior exposure. The lifting of the free edge of the tentorium shows the trochlear nerve entering the tentorium. The junction between the P2a and P2p segments (P2a, P2p) of the posterior cerebral artery is shown. ACA anterior cerebral artery, AChA anterior choroidal artery and tiny perforating vessels, BA basilar artery, DS dorsum sellae, FET free edge of tentorium, ICA internal carotid artery, LM Liliequist’s membrane, LON left optic nerve, ON oculomotor nerve, OT optic tract, PCA posterior cerebral artery, PComA posterior communicating artery, PLChA posterolateral choroidal artery arising from the P2a–P2p junction, PS pituitary stalk, RON right optic nerve, SCA superior cerebellar artery, TN trochlear nerve in the arachnoidal covering
- 83. Fig. 7.13 a Intraoperative photograph shows good exposure of the left tentorial anterior and middle incisura obtained through the pretemporal and subtemporal corridors. In this patient the basilar apex is well above the superior margin of the dorsum sellae. b Same patient. A more lateral exposure showing the pontomesencephalic junction surface and the neurovascular structures in the ambient cistern. c Intraoperative photograph of another patient showing structures in the left lateral incisural space from the subtemporal corridor. d Same patient. More lateral view. e Same patient. More posterior exposure. The lifting of the free edge of the tentorium shows the trochlear nerve entering the tentorium. The junction between the P2a and P2p segments (P2a, P2p) of the posterior cerebral artery is shown. ACA anterior cerebral artery, AChA anterior choroidal artery and tiny perforating vessels, BA basilar artery, DS dorsum sellae, FET free edge of tentorium, ICA internal carotid artery, LM Liliequist’s membrane, LON left optic nerve, ON oculomotor nerve, OT optic tract, PCA posterior cerebral artery, PComA posterior communicating artery, PLChA posterolateral choroidal artery arising from the P2a–P2p junction, PS pituitary stalk, RON right optic nerve, SCA superior cerebellar artery, TN trochlear nerve in the arachnoidal covering
- 84. THE FULLY ENDOSCOPIC SUBTEMPORAL APPROACH [ from Shahanian book ] - The traditional middle fossa subtemporal approach requires long- standing placement of retractors on the temporal lobe; therefore, potential injury to the temporal lobe can occur (e.g., hematoma and edema resulting in aphasia, hemiparesis, or seizures). This concern should not be a problem with the described approach because temporal lobe retractors are not used. (L) a Epidermoid tumor. b Atraumatic suction. c Brainstem. d Occulomotor (III) nerve. e Posterior cerebral artery (PCA). f Superior cerebellar artery (SCA). g Trochlear (IV) nerve. (N) a Epidermoid tumor. b Atraumatic suction. c Left-curved tumor forceps. d Occulomotor (III) nerve. e Posterior cerebral artery (PCA). f Posterior communicating (PCOM) artery. g Superior cerebellar artery (SCA). h Brainstem. i Trochlear (IV) nerve.
- 85. Q) a Occulomotor (III) nerve. b Internal carotid artery (ICA). c Posterior cerebral artery (PCA). d Superior cerebellar artery (SCA). (P) a Ipsilateral optic (II) nerve. b Internal carotid artery (ICA). c Occulomotor (III) nerve. d Dura overlying anterior clinoid process.
- 86. ACA
- 87. The recurrent artery of Heubner usually origins from the post-communicating segment of the anterior cerebral artery (ACA). It doubles back the ACA to reach the medial part of the Sylvian fi ssure, below the anterior perforated substance. Sometimes its path is so long that the artery loops below the basal surface of the frontal lobes. Not frequently more than one recurrent arteries can be present (Rhoton 2003 ). According to Lang the artery is double in about 30% of cases (Lang 1995 ) .
- 89. 3rd ventricle entry by - Supra optic chiasmic route – by Lamina terminalis
- 90. Recurrent artery of heubner originates near Acom (A) The middle cerebral artery (MCA) gives rise to the lateral lenticulostriate arteries (LLA) at the bifurcation complex. The medial lenticulostriate arteries (MLA) arise from the proximal section of A1. At the juncture of A1-AComm-A2 the recurrent artery of Heubner (RAH) is given off. AComm completes the anterior portion of the circle of Willis and has several perforating vessels ( Acomm Perf) that head posteriorly. In the first 5 mm of A2 the orbitofrontal ( OF) artery is given off with the frontopolar (FP) artery staying more medial. (B) A clinical picture after removal of a tuberculum sella meningioma with a well-defined display of the anterior cerebral arteries.
- 91. Recurrent artery of heubner [ R-RAH ] originates near Acom
- 95. MCA
- 97. Pcom
- 98. In parasellar pituitary 3rd n & 4th n & Pcom present in Postero-superior cavernous compartment
- 99. a,b Intraoperative image of the fenestration of deep cystic membrane using different microsurgical instruments (forceps and scissors). Asterisks posterior communicating artery and anterior choroidal artery. c Fenestration of the cisternal layer (cross Liliequist’s membrane). d Intraoperative picture at the end of the procedure http://www.springerimages.com/Images/MedicineAndPublicHealth/1-10.1007_s00381-004-0940-4-0
- 100. ACA anterior cerebral artery, AchA anterior choroidal artery, BA basilar artery, Cl clivus, DS diaphragma sellae, ICAi intracranial portion of the internal carotid artery, OA ophthalmic artery, ON optic nerve, PcomAf posterior communicating artery (fetal configuration), PcomAn posterior communicating artery (normal configuration), PG pituitary gland, PS pituitary stalk, P1 fi rst segment of the posterior cerebral artery, SCA superior cerebellar artery, SHAs superior hypophyseal arteries, TS tuberculum sellae, IIIcn oculomotor nerve The PcomA is the most variable vessel of Willis’s circle. If PcomA is wider than P1, it is said to be of the fetal type. This happens in about 20 % of cases. In 1 % of cases, it is absent (Lang 1995 ) .
- 101. Relationship of PcomA & 3rd nerve – parallel or cross each other
- 102. Posteior clinoid can be approached in optico-carotid triangle [ 3mm ] OR lateral carotid triangle
- 103. Posteior clinoid can be approached in optico-carotid triangle [ 3mm ] OR lateral carotid triangle
- 104. Pcom is seen in optico-carotid triangle – can be injured in cisternostomy while cutting lillequet membrane
- 105. A 1 [ ACA ] crosses above the Optic tract , not Optic nerve . Left subchiasmatic cistern
- 106. Relationship of PcomA & 3rd nerve – parallel or cross each other in Kernochan's Notch diagram http://en.wikipedia.org/wiki/Kernohan%27s_notch
- 107. Relationship of PcomA & 3rd nerve
- 108. Relationship of PcomA & 3rd nerve
- 109. Division of PComA
- 110. Endoscopic third ventricle from posteriorly -- a. Infundibular recess b. tuber cinereum c. mammillary bodies left posterior communicating artery (a), mammillary body (b), and right posterior hypoplasic communicating artery (c) --- measurement performed between the posterior communicating arteries using Geogebra software (a-b = 11.3 mm),
- 112. In the descriptive analysis of the 20 specimens, the PCoAs distance was 9 to 18.9 mm, mean of 12.5 mm, median of 12.2 mm, standard deviation of 2.3 mm.
- 113. http://www.ajnr.org/content/27/8/1770/F2.expansion.html Classification of the anatomic variations in the circle of Willis. In the “textbook” type, both the precommunicating segment of the anterior cerebral artery (A1) and that of the posterior cerebral artery (P1) were normal in size. The next group included both right and left A1 hypoplasia. Because no significant difference between cerebral arteries on the right and left sides has been established,5,18 we combined right and left A1 hypoplasia into A1 hypoplasia. The next group included right and left P1 hypoplasia, which again were treated as a single category, P1 hypoplasia. “Other” type included a combination of A1 hypoplasia and P1 hypoplasia, bilateral P1 hypoplasia, as well as other unclassified variations. ACA indicates anterior cerebral artery; ACo, anterior communicating artery; MCA, middle cerebral artery; ICA, internal cerebral artery; PCo, posterior communicating artery; PCA, posterior cerebral artery; BA, basilar artery
- 114. http://www.ajnr.org/content/27/8/1770/F3.expansion.html Relative contribution of proximal arteries to total volume flow in variations in the circle of Willis. Values signify mean percentage ± SD. The upper left value corresponds to the relative contribution of the right internal carotid artery in the “textbook” type or of the internal carotid artery ipsilateral to hypoplastic A1 or P1 in the other variations. The upper right value corresponds to the relative contribution of the left internal carotid artery in the “textbook” type, or of the internal carotid artery contralateral to hypoplastic A1 or P1 in the other variations. The value at the bottom corresponds to the relative contribution of the basilar artery. * The value for A1 hypoplasia variation was significantly smaller than those for “textbook” type and P1 hypoplasia variation. The value for P1 hypoplasia variation was significantly larger than that for “textbook” type. ** The value for A1 hypoplasia variation was significantly larger than that for “textbook” type. *** The value for P1 hypoplasia variation was significantly smaller than that for “textbook” type.
- 115. http://stroke.ahajournals.org/content/30/12/2671/F2.expansion.html Scheme of anatomic variations of the posterior part of the CW: variant types a through c are complete, whereas the remainder are incomplete. a, Bilateral PCoA present. b, PCA originating predominantly from the ICA. This type is known as a unilateral fetal-type PCA (FTP), indicated by the arrows; the PCoA on the other side is present. c, Bilateral FTP, with both P1 segments patent. d, Unilateral PCoA present. e, Hypoplasia or absence of both PCoAs, with isolation of the anterior and posterior circle parts at this level. f, Unilateral FTP, with hypoplasia or absence of the P1 segment. g, Unilateral FTP, with hypoplasia or absence of the contralateral PCoA. h, Unilateral FTP, with hypoplasia or absence of the P1 and PCoA. i, Bilateral FTP, with hypoplasia or absence of both P1 segments. j, Bilateral FTP, with hypoplasia or absence of one P1 segment.
- 116. Right Pcom absent
- 117. Pcom absent in post- craniopharyngioma case
- 119. AchA anterior choroidal artery Usually, the AchA arises from the ICA as a single artery, in most cases close to the PcomA. In rare cases (2 %), it arises from the PcomA or the MCA (Lang 1995 ; Rhoton 2003 ) . In the great majority of cases, it arises from the cisternal segment of the ICA lateral to the optic tract and passes below or along the optic tract (usually medially to it) to get the lateral surface of the cerebral peduncle.
- 122. ACA anterior cerebral artery, AchA anterior choroidal artery, BA basilar artery, Cl clivus, DS diaphragma sellae, ICAi intracranial portion of the internal carotid artery, OA ophthalmic artery, ON optic nerve, PcomAf posterior communicating artery (fetal con fi guration), PcomAn posterior communicating artery (normal con fi guration), PG pituitary gland, PS pituitary stalk, P1 fi rst segment of the posterior cerebral artery, SCA superior cerebellar artery, SHAs superior hypophyseal arteries, TS tuberculum sellae, IIIcn oculomotor nerve The PcomA is the most variable vessel of Willis’s circle. If PcomA is wider than P1, it is said to be of the fetal type. This happens in about 20 % of cases. In 1 % of cases, it is absent (Lang 1995 ) .
- 124. In the great majority of cases, it arises from the cisternal segment of the ICA lateral to the optic tract and passes below or along the optic tract (usually medially to it) to get the lateral surface of the cerebral peduncle.
- 126. Vertebral & Basillar artery
- 128. MINIMALLY INVASIVE RETROSIGMOID APPROACH (MIRA) - Port of entry to Endoscopic Lateral Skull Base
- 129. Lilliquits membrane present over the basillar artery & 3rd N. origin area
- 130. The basilar artery (BA) can be seen very tortuous , not always straight
- 131. Cadaveric dissection image demonstrating structures seen following dissection of the lower third of the clivus. Note how the basilar arteries and vertebral arteries can be extremely tortuous in their course.
- 132. Note 1. Basillar artery is kinky , not always straight 2. observe bilateral hypoglossal canals Cadaveric dissection following the removal of the apical and alar ligaments, and the odontoid process has been drilled away (OP). This re veals the strong and thick transverse portion of the cruciform ligament (CL). Behind this is located the tectorial membrane (TM). ET, eustachian tube; SP, soft palate; HC, hypoglossal canal; VA, vertebral artery; BA, basilar artery.
- 133. The pontomedullary junction. 1. The exit zones of the hypoglossal and abducent nerves are at the same level [ same vertical line when view from Transclival approah ( through lower clivus ) ] 2. The abducent nerve exits from the pontomedullary junction, and ascends in a rostral and lateral direction toward the clivus.
- 134. A closer view of the anterior border of the pontomedullary stem and the vertebral artery junction and origin of the basilar artery. Perforating arteries arise from the vertebral and basilar arteries. The endoscope is focusing on the hypoglossal nerve area. The posterior inferior cerebellar artery arises from the vertebral artery in the background, and runs between the two bundles of the hypoglossal nerve.
- 135. Fig. 26a, b Right side. The root fibers of the hypoglossal nerve (12) collect in two bundles, which pierce the dura in two dural pori. The hypoglossal nerve is situated more anteriorly and medially than the root fibers of the lower cranial nerves. The arterial relationship is the vertebral artery, with perforating arteries to the brain stem. The curved vertebral artery displaces and stretches the hypoglossal nerve fibers.
- 136. Through lateral skull base - The curved vertebral artery displaces and stretches the hypoglossal nerve fibers. Through anterior skull base
- 137. Through lateral skull base - The curved vertebral artery displaces and stretches the hypoglossal nerve fibers. Through lateral skull base - The opposite vertebral artery exits from the dural porus and stretches /raises the hypoglossal nerve.
- 138. Transcochlear approach leads to Lower clivus AAAM anterior atlanto-axial membrane, AAOM anterior atlanto-occipital membrane, AIM anterior intertrasversarius muscle, Cl clivus, C1 atlas, C1TP transverse process of C1, C2 axis, ET eustachian tube, JF jugular foramen, JT jugular tubercle, HC hypoglossal canal, ICAc cavernous portion of the internal carotid artery, LCapM longus capitis muscle, LColM longus colli muscle, PG pituitary gland, RCAM rectus capitis anterior muscle, RCLM rectus capitis lateralis muscle, blue-sky arrow apical ligament, green arrow external ori fi ce of the hypoglossal canal, black arrow lateral atlanto-occipital ligament, black asterisk foramen lacerum
- 139. Note CL [Lower clivus ] in these photos after drilling of cochlea The clivus bone (CL) can be seen medial to the internal carotid artery (ICA). JB Jugular bulb In the lower part of the approach, the glossopharyngeal nerve (IX) can be seen. V Trigeminal nerve, VIII Cochlear nerve, AICA Anterior inferior cerebellar artery, CL Clivus bone, DV Dandy’s vein, FN Facial nerve, FN(m) Mastoid segment of the facial nerve, FN(t) Tympanic segment of the facial nerve, GG Geniculate ganglion, ICA Internal carotid artery, JB Jugular bulb, MFD Middle fossa dura, SCA Superior cerebellar artery, SS Sigmoid sinus
- 141. Note CL [Lower clivus ] in these photos after drilling of cochlea Note the contralateral vertebral artery [ CVA ] in below photo
- 142. Two cerebellar lobes and the medullary stem. The posterior inferior cerebellar artery encircles the medullary stem. The opposite vertebral artery exits from the dural porus and raises the hypoglossal nerve.
- 143. HC = hypoglossal canal , JT= Jugular Tubercle
- 145. COMBINED APPROACHES 1. Retrolabyrinthine Subtemporal Transapical Approach 2. Retrolabyrinthine Subtemporal Transtentorial Approach Retrolabyrinthine Subtemporal Transapical Approach Retrolabyrinthine Subtemporal Transtentorial Approach
- 146. A view of the cerebellopontine angle through the retrolabyrinthine approach Note the narrow field and limited control. Posterior fossa dura (PFD) structures exposed through the standard retrolabyrinthine approach. A view of the posterior fossa dura through the combined retrolabyrinthine subtemporal transapical approach.
- 147. The middle fossa dura has been cut. The oculomotor nerve (III) is clearly seen. With more retraction of the temporal lobe and the tentorium (*), the optic nerve (II) is seen.
- 148. Retrolabyrinthine Subtemporal Transapical (Transpetrous Apex) Approach Schematic drawing showing the incision to be performed. A retrolabyrinthine approach is performed.
- 149. The dura of the middle fossa is detached from the superior surface of the temporal bone from posterior to anterior. With further detachment of the dura, the middle meningeal (MMA) artery is clearly identified.
- 150. The middle meningeal artery (MMA) and the three branches (V1, V2, V3) of the trigeminal nerve are identified. View after cutting the middle meningeal artery (MMA) and the mandibular branch of the trigeminal nerve (V).
- 151. The internal auditory canal (IAC) is identified. A large diamond burr is used to drill the petrous apex.
- 152. The petrous apex has been drilled. The internal carotid artery (ICA) is identified. At higher magnification, the abducent nerve (VI) is identified at the level of the tip of the petrous apex (PA).
- 153. Panoramic view showing the structures after opening of the posterior fossa dura. At higher magnification, the anterior inferior cerebellar artery (AICA)is seen stemming from the basilar artery (BA) at the prepontine cistern. The artery is crossed by the abducent nerve (VI). Note the good control of the prepontine cistern through this approach.
- 154. Tilting the microscope downward, the lower cranial nerves are well seen.
- 155. Retrolabyrinthine Subtemporal Transtentorial Approach The retrolabyrinthine craniotomy has been performed. The petrous apex has been partially drilled. The middle fossa dura (*) is incised.
- 156. The tentorium (*) is cut, taking care not to injure the trochlear nerve. The tentorium is further cut until the tentorial notch is reached. With retraction of the temporal lobe the optic (II), oculomotor (III) and contralateral oculomotor (IIIc) nerves are seen.
- 157. Branches of the trigeminal nerve (V1, V2, V3) at the level of the lateral wall of the cavernous sinus.
- 158. intra operative photograph through operating microscope during removal of posterior fossa arachnoid cyst -showing medulla oblnagata-cervical spinal cord -cerebellar tonsils-vertebral artery-hypoglossal nerve -accessory nerve -1st cervical nerve root - PICA loope,after removal of cyst wall
- 159. AICA
- 160. Posterior view of the left CPA with a 30° angled endoscope gives a view of CPA contents and permitsobservation of the blind spots by “looking around the corner.” V indicates trigeminal nerve; VI, abducens nerve; IV, trochlear nerve; VII, facial nerve anteriorly hidden by VIII; VIII, vestibulocochlear nerve; IX, glossopharyngeal nerve; X, vagusnerve; XI, spinal accessory nerve; XII, hypoglossal nerve; aica, anterior-inferior cerebellar artery; DV, Dandy’s vein or superior petrosal vein; SPS, superior petrosal sinus; Tent, tentorium.
- 161. 6th nerve origin is above or below AICA or has two rootlets of origin
- 162. Right sided anterior petrosectomy on a cadaver dissection: intradural exposure and operative field. PCA Petrous carotid artery; DPA drilled petrous apex; IPS inferior petrosal sinus; BA basilar artery; VI 6th cranial nerve; AICA anterior inferior cerebellar artery; P pons; V 5th cranial nerve
- 163. Cadaveric dissection image taken with a 70-degree endoscope. The right internal auditory canal (IAC) can be clearly visualized with the meatal segment of the anterior inferior cerebellar artery (AICA) entering the meatus. This vessel then loops between the facial (CN VII) and vestibulocochlear nerves. CN, cochlear nerve; CN V, trigeminal nerve.
- 164. The anterior inferior cerebellar artery, lying between the auditory and facial nerves, is found in 38% of cases. 5 Trigeminal nerve 7 Facial nerve 8 Vestibulocochlear nerve
- 166. Artist’s renderings showing posterior view of the left IAM. ( a ) Subarcuate artery penetrates the dura of the subarcuate fossa near the IAM. The labyrinthine artery enters the meatus with the vestibulocochlear and the facial nerves. ( b ) Laterally convex loop of the AICA is embedded in the dura covering the subarcuate fossa, where it gives off the subarcuate artery. ( c ) AICA loop is embedded in the dura and bone ( arrow ) surrounding the subarcuate
- 167. fossa. ( d ) Dura over the subarcuate fossa has been incised, and the dura with the adherent loop is dissected free from the subarcuate fossa in preparation for opening the IAM. ( e ) Dura over the subarcuate fossa has been incised and remains attached to the artery. The bone surrounding the embedded AICA loop is removed with a 2-mm diamond drill to displace the artery medially for exposure of the IAM (From Tanriover and Rhoton [ 50 ] )
- 169. The LA usually originates from the AICA, rarely directly from the BA.
- 171. https://www.facebook.com/entdissect ionpg/posts/852889001461081 • The subarcuate artery arises from the anterior inferior cerebellar artery(AICA-from the Basilar Artery) and does not supply the labyrinth. It is located between the anterior and posterior crura of the superior semicircular canal passing through the petro mastoid canal. This endoscopic view shows the posterior relationship to the AFB(acousticofacial bundle). • On CT it can be easily be mistaken for a fracture line. Radiologic classification (Migirov et al 2007): type I - invisible type II - less than 0.5 mm width type III - 0.5-1 mm width type IV - greater than 1 mm width • This artery is commonly encountered during labyrinthectomy.
- 172. Labyrinthine artery / subarcuate artery Labyrinthine artery Subarcuate artery
- 173. subarcuate artery
- 174. subarcuate artery
- 175. PICA
- 176. From vertebral artery book
- 177. PICA passes between two bundles of 12th nerve The endoscope is focusing on the hypoglossal nerve area. The posterior inferior cerebellar artery arises from the vertebral artery in the background, and runs between the two bundles of the hypoglossal nerve.
- 178. PICA can be seen running between the vagus (CN X)
- 179. PICA can be seen running between spinal and cranial portions of the accessory nerves (CN XI – S, CN XI – C). Endoscopic lateral skull base Endoscopic anterior skull base Lateral skull base – far lateral approach
- 180. PICA passes between two bundles of 12th nerve & between two roots of 11th nerve Cadaveric dissection image demonstrating the posterior inferior cerebellar artery (PICA) running between the vagus (CN X) and the cranial accessory nerve rootlets (CN XI-C) at the position where the nerves exit the brainstem. CN VII, facial nerve; CN VIII, vestibulocochlear nerve; NI, nervus intermedius; CN IX, glossopharyngeal nerve; CN XI-S, spinal accessory nerve The tip of the endoscope lies between the acousticofacial nerve bundle and the anterior inferior cerebellar artery. The posterior inferior cerebellar artery arises from the vertebral artery, runs between the root fibers of the hypoglossal nerve, and forms a loop below the roots of the lower cranial nerves, before coursing in a posterior direction.
- 181. Two cerebellar lobes and the medullary stem. The posterior inferior cerebellar artery encircles the medullary stem. The opposite vertebral artery exits from the dural porus and raises the hypoglossal nerve.
- 182. 11th nerve behind left vertebral artery at cervico-medullary junction – listen lecture at 23.25 min in this Prof. Amin Kassam video https://www.youtube.com/watch?v=QoMCqwJ6Ke0 Through anterior skull base approach Through endoscopic lateral skull base approach – The entrance of the vertebral artery is the boundary between the foramen magnum and the spinal part of the accessory nerve.
- 183. The accessory nerve (XI) is closely related to the vertebral artery (VA) at the point of dural entrance. Note the dura attached to the artery at this level. Endoscopic lateral skull base approach
- 184. The accessory nerve (XI) is closely related to the vertebral artery (VA) at the point of dural entrance. Note the dura attached to the artery at this level. In far lateral approach
- 185. C2 nerve root below the 11th nerve in posterior triangle clearance in SLD the C2 nerve root is seen crossing the vertebral artery (VA).
- 186. Superior Cerebellar Artery [ SCA ]
- 187. SCA in enlarged translabyrinthine approach
- 188. Endoscopic lateral skull base [ note 2 branches of SCA – may present from the origin itself ]
- 189. 3rd nerve is sandwiched between posterior cerebral artery & superior cerebellar artery [ note 2 branches of SCA – may present from the origin itself ] Through endoscopic lateral skull base Through endoscopic lateral skull base
- 190. 3rd nerve is sandwiched between posterior cerebral artery & superior cerebellar artery Through endoscopic lateral skull base Through endoscopic anterior skull base
- 191. 3rd nerve is sandwiched between posterior cerebral artery & superior cerebellar artery Through endoscopic lateral skull base Through endoscopic anterior skull base
- 192. See the basilar artery, PCA,SCA.....through endoscopic 3rd ventriculostomy
- 193. 0° endoscope. In the next pictures the retrosellar area is presented when an endoscope is inserted behind the pituitary stalk and orientated downwards (arrows). The dorsum sellae is outlined with a dotted line. - From Atlas of Endoscopic Anatomy for Endonasal lntracranial Surgery ; Paolo Cappabianca
- 194. 30° endoscope. After the introduction of a downward orientated endoscope behind the dorsum sellae the basilar tip is visualized. PCoA = posterior communicating artery, SCA = superior cerebellar artery, P1-P2 = posterior cerebral artery.
- 195. 30° endoscope. Right side. closer view. PCoA = posterior communicating artery. SCA = superior cerebellar artery. P1 = posterior cerebral artery.
- 196. 30° endoscope. Left side. closer view. SCA = superior cerebellar artery. P1-P2 = posterior cerebral artery. PCoA = posterior communicating artery.
- 197. Posterior cerebral artery [ P1 & P 2 ]
- 198. P1 in relation to 3rd nerve P2 in relation to 3rd nerve
- 199. 3rd nerve is sandwiched between posterior cerebral artery [ PCA ] & superior cerebellar artery [ SCA ]
- 200. Right supraorbital approach (0 optic). 1 Diaphragma sellae, 2 cn II, 3 optic tract, 4 ICA, 5 A1, 6 M1, 7 C. N.III, 8 anterior petroclinoid fold, 9 anterior clinoid process. A Optocarotid window, B window between ICA and cn III –I think B is nothing but posterior clinoid process C window lateral of cn III Right supraorbital approach (30 optic). Window between ICA and cn III : 1 tuber cinereum, 2 left P1, 3 left cn III, 4 BA, 5 right P1, 6 right SCA, 7 right cn III
- 201. For Other powerpoint presentatioins of “ Skull base 360° ” I will update continuosly with date tag at the end as I am getting more & more information click www.skullbase360.in - you have to login to slideshare.net with Facebook account for downloading.
