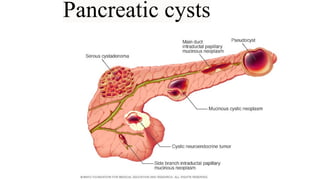
Pancreatic cyst and tumour
- 2. • Pancreatic cysts are saclike pockets of fluid on or in pancreas. • Pancreatic cysts are typically found during imaging testing for another problem. • The main categories of pancreatic cysts can be divided into two groups, non-neoplastic or neoplastic cysts.
- 3. Causes • The cause of most pancreatic cysts is unknown. Some cysts are associated with rare illnesses, including polycystic kidney disease or von Hippel-Lindau disease, a genetic disorder that can affect the pancreas and other organs. • Pseudocysts often follow a bout of a painful condition in which digestive enzymes become prematurely active and irritate the pancreas (pancreatitis). • Pseudocysts can also result from injury to the abdomen, such as from a car accident.
- 4. Risk factors • Heavy alcohol use and gallstones are risk factors for pancreatitis, and pancreatitis is a risk factor for pseudocysts. • Abdominal injury is also a risk factor for pseudocysts.
- 5. Types The characteristics and location of the pancreatic cyst, along with your age and sex, can sometimes help doctors determine the type of cyst you have: •Pseudocysts are not cancerous (benign) and are usually caused by pancreatitis. Pancreatic pseudocysts can also be caused by trauma. •Serous cyst adenomas can become large enough to displace nearby organs, causing abdominal pain and a feeling of fullness. •Mucinous cystic neoplasms are usually situated in the body or tail of the pancreas and nearly always occurs in women, most often in middle-aged women. Mucinous cyst adenoma is precancerous, which means it might become cancer if left untreated. Larger cysts might already be cancerous when found.
- 6. •An intraductal papillary mucinous neoplasm (IPMN) is a growth in the main pancreatic duct or one of its side branches. IPMN may be precancerous or cancerous. It can occur in both men and women older than 50. Depending on its location and other factors, IPMN may require surgical removal. •Solid pseudo-papillary neoplasms are usually situated in the body or tail of the pancreas and occur most often in women younger than 35. They are rare and sometimes cancerous. •A cystic neuroendocrine tumour is mostly solid but can have cyst like components. They can be confused with other pancreatic cysts and may be precancerous or cancerous.
- 7. Symptoms When signs or symptoms of pancreatic cysts do occur, they typically include: •Persistent abdominal pain, which may radiate to back •Nausea and vomiting •Weight loss
- 8. Diagnosis After taking a medical history and performing a physical exam, your doctor may recommend imaging tests to help with diagnosis and treatment planning. Tests include: •Computerized tomography (CT) scan. This imaging test can provide detailed information about the size and structure of a pancreatic cyst. •MRI scan. This imaging test can highlight subtle details of a pancreatic cyst, including whether it has any components that suggest a higher risk of cancer. •Endoscopic ultrasound. This test, like an MRI, can provide a detailed image of the cyst. Also, fluid can be collected from the cyst for analysis in a laboratory for possible signs of cancer. •Magnetic resonance cholangiopancreatography (MRCP). MRCP is considered the imaging test of choice for monitoring a pancreatic cyst. This type of imaging is especially helpful for evaluating cysts in the pancreatic duct.
- 9. Treatment Watchful waiting or treatment depends on the type of cyst , its size, its characteristics and whether it's causing symptoms. Watchful waiting A benign pseudocyst, even a large one, can be left alone as long as it isn't bothering. Serous cyst adenoma rarely becomes cancerous, so it also can be left alone unless it causes symptoms or grows. Some pancreatic cysts should be monitored. Drainage A pseudocyst that is causing bothersome symptoms or growing larger can be drained. A small flexible tube (endoscope) is passed through mouth to stomach and small intestine. The endoscope is equipped with an ultrasound probe (endoscopic ultrasound) and a needle to drain the cyst. Sometimes drainage through the skin is necessary. Surgery Some types of pancreatic cysts require surgical removal because of the risk of cancer. Surgery might be needed to remove an enlarged pseudocyst or a serous cyst adenoma that's causing pain or other symptoms.
- 11. • Pancreatic cancer begins in the tissues of pancreas. • Several types of growths can occur in the pancreas, including cancerous and noncancerous tumors. The most common type of cancer that forms in the pancreas begins in the cells that line the ducts that carry digestive enzymes out of the pancreas (pancreatic ductal adenocarcinoma).
- 12. Causes • It's not clear what causes pancreatic cancer. • Doctors have identified some factors that may increase the risk of this type of cancer, including smoking and having certain inherited gene mutations.
- 13. Risk factors Factors that may increase risk of pancreatic cancer include: •Smoking •Diabetes •Chronic inflammation of the pancreas (pancreatitis) •Family history of genetic syndromes that can increase cancer risk. •Family history of pancreatic cancer •Obesity •Older age, as most people are diagnosed after age 65
- 14. Pathophysiology • Pancreatic cancer occurs when cells in pancreas develop changes (mutations) in their DNA. • A cell's DNA contains the instructions that tell a cell what to do. • These mutations tell the cells to grow uncontrollably and to continue living after normal cells would die. • These accumulating cells can form a tumour. • When left untreated, the pancreatic cancer cells can spread to nearby organs and blood vessels and to distant parts of the body.
- 15. Symptoms Signs and symptoms of pancreatic cancer often don't occur until the disease is advanced. They may include: •Abdominal pain that radiates to back •Loss of appetite or unintended weight loss •Yellowing of skin and the whites of eyes (jaundice) •Light-coloured stools •Dark-coloured urine •Itchy skin •New diagnosis of diabetes or existing diabetes that's becoming more difficult to control •Fatigue
- 16. Diagnosis •Imaging tests that create pictures of internal organs. These tests help doctors visualise internal organs, including the pancreas. Techniques used to diagnose pancreatic cancer include ultrasound, computerised tomography (CT) scans, magnetic resonance imaging (MRI) and, sometimes, positron emission tomography (PET) scans. •Using a scope to create ultrasound pictures of pancreas. An endoscopic ultrasound (EUS) uses an ultrasound device to make images of pancreas from inside abdomen. The device is passed through a thin, flexible tube (endoscope) down esophagus and into your stomach in order to obtain the images. •Removing a tissue sample for testing (biopsy). A biopsy is a procedure to remove a small sample of tissue for examination under a microscope. •Blood test. Doctor may test blood for specific proteins (tumour markers) shed by pancreatic cancer cells. One tumor marker test used in pancreatic cancer is called CA19-9.
- 18. Treatment • Treatment for pancreatic cancer depends on the stage and location of the cancer as well as on overall health and personal preferences. • For most people, the first goal of pancreatic cancer treatment is to eliminate the cancer, when possible. • When that isn't an option, the focus may be on improving quality of life and limiting the cancer from growing or causing more harm. • Treatment may include surgery, radiation, chemotherapy or a combination of these. • When pancreatic cancer is advanced and these treatments aren't likely to offer a benefit, doctor will focus on symptom relief (palliative care) to keep as comfortable as possible for as long as possible.
- 19. Surgery Operations used in people with pancreatic cancer include: •Surgery for tumors in the pancreatic head. If cancer is located in the head of the pancreas, may consider an operation called a Whipple procedure (pancreaticoduodenectomy). The Whipple procedure is a technically difficult operation to remove the head of the pancreas, the first part of the small intestine (duodenum), the gallbladder, part of the bile duct and nearby lymph nodes. In some situations, part of the stomach and colon may be removed as well. Surgeon reconnects the remaining parts of pancreas, stomach and intestines to allow to digest food.
- 21. •Surgery for tumors in the pancreatic body and tail. Surgery to remove the left side (body and tail) of the pancreas is called distal pancreatectomy. •Surgery to remove the entire pancreas. In some people, the entire pancreas may need to be removed. This is called total pancreatectomy. One can live relatively normally without a pancreas but do need lifelong insulin and enzyme replacement.
