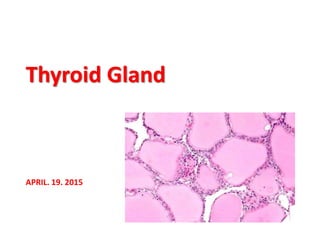
Thyroid gland dr faeza
- 1. APRIL. 19. 2015 Thyroid Gland
- 2. Thyroid gland • Anatomy • Histology • Physiology • Pathology • Hyperthyroidism • Hypothyroidism • Tumors April . 12. 2015
- 3. 15-25 grams
- 4. Earliest endocrine organs to differentiate • Thyroid; 1st ph. Pouch • Thymus & Inf. Para. G; 3rd ph. Pouch • Sup. Para. G; 4th ph.pouch • Remnants; • Arrested descent • Thyroglossal duct – cyst • Inferior part – pyramidal lobe Foramen Caecum Lingual thyroid Tongue Thyroglossal duct Hyoid boneThyrohoid membrane Thyroid cartilage Cricoid cartilage ? Thyroid gland
- 7. Arteries; Superior and inferior thyroid arteries Veins; Superior, middle, and inferior thyroid veins Lymphatics; Periglandular, prelaryngeal, pretracheal, paratracheal lymph nodes (level VI) Nerves; Sympathetic: Superior, middle sympathetic ganglia Parasympathetic: Vagus nerves Recurrent laryngeal nerve. External laryngeal nerve Thyroid gland
- 9. High mag of thyroid follicles – note Parafollicular or C-Cells (arrows)
- 10. Examples of results of thyroid function tests Free T3Free T4TSHThyroid functional state Euthyroid Thyrotoxicosis Myxoedema Suppressive T4 therapy T3 toxicity
- 11. Developmental Abnormalities Lingual Thyroid; Midline mass at the base of tongue THYROGLOSSAL DUCT CYST
- 12. Many vegetables are goiterogens, fruits are NOT Goitrogens; chemical agents inhibit function of the thyroid gland. Suppress T3 and T4 synthesis, so the level of TSH increases, &t hyperplastic enlargement of the gland (goiter) follows.
- 13. Anti-thyroid autoantibodies Anti-thyroid peroxidase Abs; Hashimoto`s thyroiditis & Grave’s disease. TSH receptor Abs; (two forms) • 1. An activating Abs “TSI” (associated with hyperthyroidism); TSH receptor activating Abs are characteristic of Graves Disease (in 90% of patients). • 2. A blocking antibody (associated with thyroiditis); These competitively inhibit the binding of TSH to its receptor. Anti-Thyroglobulin Abs; found in most people with Grave’s disease and nearly all with Hashimoto’s thyroiditis). • They are commonly used to monitoring thyroid cancer following thyroidectomy.
- 14. Tests of Thyroid Function 1. Serum Thyroid-Stimulating Hormone (TSH) (Normal 0.5–5 U/mL) 2. Total T4 (55–150 nmol/L) & T3 (1.5–3.5 nmol/L) 3. Free T4 (12–28 pmol/L) & Free T3 (3–9 pmol/L) 4. Thyroid Antibodies: 5. Thyroid antibodies include: antibodies against thyroid peroxidase (TPO), anti-thyroglobulin antibodies & TSH receptor antibodies 6. Serum Thyroglobulin: The most important use is in monitoring patients with differentiated thyroid cancer for recurrence, particularly after total thyroidectomy & RAI ablation. 7. Serum Calcitonin (0–4 pg/mL Basal): It is also a sensitive marker of Medullary Thyroid Carcinoma.
- 15. Tests of Thyroid Function • Images techniques: X – Ray U/S CT Scan MRI PET RAI uptake (Scan), (I-123) or technetium (99mTc) • FNA • Biopsy
- 16. • The thyroid scan is used to determine the size, shape & position of the thyroid gland • A whole-body thyroid scan is typically performed on people who have had thyroid Ca. It detects the recurrence & spread of thyroid Ca.
- 17. Normal Thyroid Scan Cold nodule in left lobe
- 19. PET/CT scan of the neck. Axial images through the thyroid gland on A) A CT-scan B) A 18F-FDG PET scan & C) A fused 18F-FDG PET & CT scan. A heterogeneous thyroid (arrows) is located in a CT scan in panel. A. Diffuse accumulation of 18F- FDG (arrows) is seen throughout the thyroid in panel. B. Fusion of the CT scan & 18F-FDG PET scan confirms that the entire thyroid is hypermetabolic.
- 20. Disorders Associated with Thyrotoxicosis Associated with Hyperthyroidism Primary • Diffuse hyperplasia (Graves disease) • Hyperfunctioning (“toxic”) multinodular goiter • Hyperfunctioning (“toxic”) adenoma • Iodine-induced hyperthyroidism • Neonatal thyrotoxicosis associated with maternal Graves disease Secondary TSH-secreting pituitary adenoma (rare) Not Associated with Hyperthyroidism Granulomatous (de Quervain) thyroiditis (painful) Subacute lymphocytic thyroiditis (painless) Struma ovarii (ovarian teratoma with ectopic thyroid) Factitious thyrotoxicosis (exogenous thyroxine intake)
- 21. Hyperthyroidism Clinical Course. Hypermetabolic state. Overactivity of the SNS (increase in the β-adrenergic “tone”).
- 22. Hyperthyroidism Increase BMR • The skin • Sweating • Weight loss despite increased appetite.
- 23. Hyperthyroidism • Cardiac manifestations • Elevated cardiac contractility and cardiac output, in response to increased peripheral O2 requirements. • Tachycardia, palpitations. • Arrhythmias, particularly Atrial fibrillation. • Congestive HF. • Cardiomegaly
- 24. Hyperthyroidism Over activity of Sympathetic Nervous System; • Tremor, hyperactivity, emotional labile, anxiety, inability to concentrate, insomnia. • Thyroid myopathy; Muscle weakness and decreased muscle mass. • GIT, hypermotility, diarrhea, & malabsorption
- 25. Hyperthyroidism • Ocular changes; • Staring gaze • lid lag • Proptosis (only in Graves Dis)
- 26. Hyperthyroidism • The skeletal system. • Increased bone resorption & risk of Osteoporosis & fractures • Atrophy of skeletal M. • Minimal liver enlargement due to fatty changes in the hepatocytes; • generalized lymphoid hyperplasia & lymphadenopathy in Graves disease. Thyroid storm Apathetic hyperthyroidism
- 27. Diagnosis of hyperthyroidism • Both Clinical and laboratory findings. • A low TSH value • High free T4. • RAI uptake by the thyroid gland.
- 28. Graves disease • The most common cause of endogenous hyperthyroidism. • Characterized by a triad of clinical findings: • • Hyperthyroidism associated with diffuse enlargement of the gland • • Infiltrative ophthalmopathy with resultant exophthalmos • • Localized, infiltrative dermopathy, (pretibial myxedema, which is present in a minority of patients
- 29. Pathogenesis of Graves disease • Autoantibodies against multiple thyroid proteins, most importantly the TSH receptor. • Thyroid stimulating immunoglobulin (TSI) Abs, in 90% of patients.
- 30. Graves ophthalmopathy • Exopthalmos, protrusion of the eyeball is associated with; increased Vo. Of retroorbital CT & extraocular M., for several reasons; • (1) infiltration of retroorbital space by mononuclear cells; • (2) inflammation, edema and swelling of extraocular M; • (3) accumulation of ECM, glycosaminoglycans such as hyaluronic acid and chondroitin sulfate; • (4) increased numbers of adipocytes (fatty infiltration). • These changes displace the eyeball forward and can interfere with the function of the extraocular muscles.
- 31. The thyroid gland is symmetrically enlarged due to diffuse hypertrophy and hyperplasia of thyroid follicular epithelial cells Graves disease
- 34. Graves disease
- 35. Graves Disease • SUMMARY: ■ Graves disease, the most common cause of endogenous hyperthyroidism, • characterized by the triad of thyrotoxicosis, ophthalmopathy, and dermopathy. • ■ It is an autoimmune disorder caused by activation of thyroid epithelial cells by autoantibodies to the TSH receptor that mimic TSH action (thyroid-stimulating immunoglobulins). • ■ The thyroid in Graves disease is characterized by diffuse hypertrophy and hyperplasia of follicles and lymphoid infiltrates; • glycosaminoglycan deposition and lymphoid infiltrates are responsible for the ophthalmopathy and dermopathy. • ■ Laboratory features include elevations in serum free T3 and T4 and decreased serum TSH.
- 36. G O I T E R
- 37. Causes of Hypothyroidism Primary Iodine deficiency* Autoimmune hypothyroidism Hashimoto thyroiditis* Postablative Surgery, radioiodine therapy, or external irradiation Genetic defects in thyroid development (PAX8, FOXE1, TSH receptor mutations) (rare) Thyroid hormone resistance syndrome (THRB mutations) (rare) Drugs (lithium, iodides, p-aminosalicylic acid)* Congenital biosynthetic defect (dyshormonogenetic goiter) (rare) * Secondary (Central) Pituitary failure (rare) Hypothalamic failure (rare)
- 38. Autoimmune hypothyroidism • The most common cause of hypothyroidism in iodine-sufficient areas of the world. • The majority are due to Hashimoto thyroiditis. • antimicrosomal, antithyroid peroxidase, and antithyroglobulin antibodies, • goitrous • can occur in isolation or in conjunction with autoimmune polyendocrine syndrome.
- 39. • Myxedema is applied to hypothyroidism developing in the older child or adult. • Early symptoms; Dry skin, brittle hair, depression, wt. gain, constipation, increased sensitivity to cold , weakness, Heavy menstruation, joint & M. pain. • Late symptoms;, Puffy face, hands & feet, Slow speech, Thickening of the skin. • Myxedema coma; medical emergency, thyroid hormones becomes very low. Hypothyroidism
- 40. Cretinism
- 43. THYROIDITIS • Hashimoto (Auto-Immune) (Lymphoid follicles with germinal centers), MOST COMMON cause of acquired hypothyroidism in USA • Subacute Granulomatous (DeQuervain) • Subacute Lymphocytic (just like Hashimoto’s but NO fibrosis and no germinal centers), often post-partum
- 44. Hashimoto thyroiditis. The thyroid parenchyma contains a dense lymphocytic infiltrate with germinal centers. Residual thyroid follicles lined by deeply eosinophilic Hürthle cells are also seen.
- 48. G O I T E R
- 49. GOITERS (diffuse or nodular) • IODINE deficiency** • Associated with HYPO thyroidism** eventually, NOT hyperthyroidism • Increased TSH • Goitrogens vegetables.
- 50. Etiology of Nontoxic Goiter ClassificationSpecific etiology Iodine deficiency, dietary goitrogens (cassava, cabbage) Endemic Iodide, amiodarone, lithiumMedications Subacute, chronic (Hashimoto's)Thyroiditis Dyshormonogenesis - genetic defect. (Impaired hormone synthesis from enzyme defects) Familial Adenoma, carcinomaNeoplasm Goiter
- 51. Physiological goiter: Endemic goiter; The occurrence of a goiter in a significant proportion of individuals in a particular geographic regions due to dietary iodine deficiency. Goiter
- 52. Goiter Colloid goitre; A colloid goitre is a late stage of diffuse hyperplasia when TSH stimulation has fallen off & when the follicles are inactive & full of colloid
- 53. Multinodular goiter. A, Gross morphology nodular gland, containing areas of fibrosis and cystic change. B, Photomicrograph of a hyperplastic nodule, with compressed residual thyroid parenchyma on the periphery. Note absence of a prominent capsule, a distinguishing feature from follicular neoplasms
- 54. “NODULES” • Solitary vs. Multiple • Younger vs. Older • Male vs. Female • Hx. neck radiation vs. NO Rx. • “Cold” vs. HOT (really NOT-cold)
- 55. Thyroid Neoplasms • “Nodules” vs. true neoplasms • Adenomas vs. Carcinomas
- 56. NEOPLASMS • ADENOMAS – FOLLICULAR – HÜRTHLE (oxyphilic) • CARCINOMAS – FOLLICULAR – PAPILLARY – MEDULLARY (AMYLOID) – ANAPLASTIC (worst)
- 57. • Risk factors for malignancy; • Ionizing radiation. • Sex; women 3 times > than men. A discrete swelling in male is much more likely to be malignant than in a female. • Family history; Medullary (MEN2) syndromes) & Non-medullary thyroid cancer (familial cancer syndromes e.g. Cowden's syndrome; has high risk of breast, thyroid, endometrium, colorectal & skin tumors. • Investigations; TFTs, Autoantibody titers, Isotope scan, U/S & CT, MRI, FNA & Biopsy.
- 59. Follicular adenoma of thyroid. A, A solitary, well-circumscribed nodule. B, well-differentiated follicles resembling normal thyroid parenchyma
- 62. HÜRTHLE CELL ADENOMA, note “atypia”
- 63. CARCINOMAS • Papillary carcinoma (>85% of cases) • Follicular carcinoma (5% to 15% of cases) • Anaplastic (undifferentiated) carcinoma (<5% of cases) • Medullary carcinoma (5% of cases)
- 64. Follicular carcinoma. A, Cut surface of a follicular carcinoma with substantial replacement of the lobe of the thyroid. The tumor has a light tan appearance and contains small foci of hemorrhage. B, A few of the glandular lumens contain recognizable colloid.
- 65. Capsular integrity in follicular neoplasms. adenomas (A), follicular carcinomas demonstrate capsular invasion (B, arrows) that may be minimal, or wide The presence of vascular invasion is another feature of follicular carcinomas
- 66. Thyroid; Follicular ca. invasion or metastases is the only evidence of malignancy.
- 67. Papillary neoplasms do NOT usually look uniform on cut surface.
- 68. Papillary carcinoma of the thyroid
- 71. ORPHAN ANNIE CELLS in PAPILLARY CARCINOMA
- 72. Anaplastic carcinoma of the thyroid
- 73. MEDULLARY CARCINOMA of the thyroid with “HYALINIZATION”, i.e., AMYLOID!!!
- 74. HYALINIZATION showing APPLE GREEN birefringence in CONGO RED stain, i.e., AMYLOID
- 75. Fine Needle Aspiration Cytology •FNAC is a safe, sensitive & specific technique. •An excellent screening test for thyroid swellings •Diagnosis can be achieved in a majority of cases. •Thyroid papillary carcinoma ; •(a) FNAC smear showing intra- nuclear cytoplasmic inclusions (black arrow) & nuclear grooves (red arrow). •(b) Histopathology section showing intra-nuclear cytoplasmic inclusions (black arrow) and nuclear grooves (red arrow) •© ground glass nuc. (blue arrow).
- 76. • A discrete swelling in an otherwise impalpable gland is termed isolated or solitary. Conditions presenting as Solitary thyroid nodule are; 1. Dominant nodule of multinodular goiter 2. Thyroid adenoma (30-40%) 3. Thyroid cyst 4. Thyroid carcinoma (10 - 15%) 5. Localised form of thyroiditis 6. Colloid nodule • (Incidental nodules). Solitary thyroid nodule