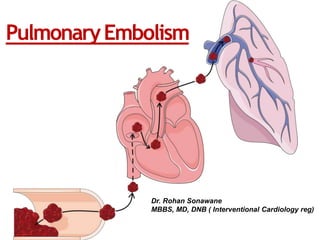
Pulmonary embolism
- 1. PulmonaryEmbolism Dr. Rohan Sonawane MBBS, MD, DNB ( Interventional Cardiology reg)
- 2. • Introduction • Definition & Sources • Riskfactors & aetiology • Pathogenesis • Clinical presentation • Differential Diagnosis • Investigations • Management • Complications • Prevention
- 3. • It is the third most common cardiovascular disease after MI and stroke. • Annual incidence of 100-200 per 1 lac population. • It is the only preventable lethal disease.
- 4. Pulmonary Embolism • Thrombus dislodges (DVT) and travels to pulmonary arteries causing occlusion of apulmonary artery(ies). • Provoked PE: PE in patients with recent occurrence of major clinical risk factor for VTE. Like recent Sx, trauma, OCP. • Proximal DVT: DVT in popliteal vein or above (40%) • Unprovoked PE: PE in patients with no recently occurring major clinical risk factors for VTE or patients with active cancer, thrombophilia or family history of DVT (these are risks, but they are constant)
- 5. Source • DVT • Intracardiac Clot • Air embolism • Fat embolism • Amniotic fluid embolism • Septic embolism • Tumor embolism
- 6. Risk Factors • Virchow’s Triad
- 7. Risk Factors • Prior DVTorPE • CongestiveHeart Failure • Malignancy • Obesity • smoking • Estrogen, OCP ,HRT • Pregnancy • Lower limbs injury • Orthopedic Surgery • Prolonged immobilization, travel • Surgery requiring >30 minutes general anesthesia
- 8. Risk Factors • Age> 40 • VenousStasis • Factor VLeiden mutation • Protein Cdeficiency • Protein Sdeficiency • Antithrombin deficiency • Anticardiolipin antibodies • SLE,APS • Hyperhomocystinemia
- 9. Risk Factors ICU-related factors: • Immobility • Neuromuscular paralysis (drug-induced) • Central venous catheters • Severesepsis
- 10. Pathogenesis
- 12. Clinical Presentation • Small PE:Asymptomatic, SOB,chestdiscomfort. • Medium PE: SOB,Haemoptysis, Pleuritic chest pain, Tachycardia,Tachypnea, Pleural rub. • Massive PE: Death, Shock,Severecentral chest pain, Syncope, Pallor, Sweating, Central cyanosis, Elevated JVP ,Loud P2,S2split, galloprhythm. 1
- 14. Clinical Prediction Score Clinical decision points Wells rule Original version1 Simplified version2 Previous PE or DVT 1.5 1 Heart Rate ≥ 100 bpm 1.5 1 Sx or immobilisation within past 4 weeks 1.5 1 Hemoptysis 1 1 Active Cancer 1 1 Clinical Sign of DVT 3 1 Alternative Δ less likely 3 1 Clinical probability PE unlikely 0-4 0-1 PE likely > 5 ≥2 1. Wells PS et al. Thromb Haemost 2000;83(3):416–420. 2. Gibson NS, Wells PS et al. Thromb Haemost 2008;99(1):229–234.
- 15. Clinical Prediction Score Clinical decision points Revised Geneva Score Original version1 Simplified version2 Previous PE or DVT 3 1 Heart rate 75-94 bpm ≥95 bpm 3 5 1 2 Surgery or Fracture within past month 2 1 Hemoptysis 2 1 Active Cancer 2 1 Unilateral lower limb pain 3 1 Pain on deep veinous palpation/ unilateral edema 4 1 Age ≥ 65 years 1 1 Clinical probability PE unlikely 0-5 0-2 PE likely ≥6 ≥3 1. Le Gal G et al. Ann Intern Med 2006;144(3):165–171. 2. Klok FA et al. Arch Intern Med 2008;168(19):2131–2136.
- 16. Differential Diagnosis • Myocardial Infraction • Pleurisy • Pneumonia • Bronchitis • Pneumothorax • Costochondritis • Rib #
- 17. Investigations • D-dimer • ECG • Chest X-ray • Echocardiography • Ventillation Perfusion Scan • CT Pulmonary Angiography • Invasive Pulmonary Angiography
- 18. D-dimer • Levels elevate in acute thrombosis • High negative predictive value and low positive predictive value • False positive in many conditions like in cancer & pregnancy • Specificity decreases with age (almost 10% in patients > 80years) • Age adjusted cut offs used after 50 years i.e. (age x 10 ug/L) • For < 50 years, cut off is 500 ug/L
- 19. ECG In severe cases 1) RV strain, like inversion of T waves in leads V1–V4, a QR pattern in V1 2) S1Q3T3 pattern 2) Incomplete or complete RBBB In milder cases Only anomaly may be sinus tachycardia - 40% Atrial arrhythmias, most frequently atrial fibrillation may be seen
- 20. ECG
- 24. 2D Echo • Echo doesnot provide conclusive evidence of PE. • Sensitivity is only 65% • But is available bedside and cheap. • Rules out other causes like MI, Tamponade
- 28. IVC is dilated without any inspiratory collapse
- 29. Ventilation/PerfusionRatio • Increases specificity • In acute PE, ventilation is expected to be normal in hypoperfused segments • Radiation exposure lower than CT angiography • Radiation and contrast medium-sparing procedure • So can be done in : Outpatients with low clinical probability In young (particularly female) patients, In pregnancy History of contrast medium-induced anaphylaxis In severe renal failure • Results are interpreted as low, intermediate or high probability of PE
- 31. CT Pulmonary Angiography • Method of choice for imaging patients with suspected PE • Highly sensitive and specific • Cannot interpret subsegmental thrombus • Radiation and Iodine contrast are major drawbacks • Can’t be used in renal failure patients.
- 33. The PIOPED II trial observed a sensitivity of 83% and a specificity of 96% for MDCT Negative Predictive Value low clinical probability of PE - 96% intermediate clinical probability - 89% high pre-test probability - 60% Positive Predictive Value Low clinical probability of PE – 58% Intermediate clinical probability – 92% High clinical probability- 96% PIOPED ll trail (Prospective Investigation on Pulmonary Embolism Diagnosis)
- 34. PulmonaryAngiography • Was Gold Standard for decades • Replaced now by CT pulmonary angiography • Often used to guide percutaneous catheter- directed treatment of acute PE • Procedure-related mortality 0.5%, major non-fatal complications 1%
- 36. Management of PE
- 38. Diagnostic algorithm for Non high-risk PE [2014 ESC Guidelines. European Heart Journal (2014) 35, 3033–3080 ]
- 39. Diagnostic algorithm for High-risk PE [2014 ESC Guidelines. European Heart Journal (2014) 35, 3033–3080 ]
- 40. Pulmonary Embolism Severity Index
- 41. Original PESI Simplified PESI
- 42. Intermediate risk PE • Hemodynamically stable with evidence of myocardial injury and RV dysfunction with high PESI • They have high 30 day mortality • Early reperfusion is required in them
- 44. Thrombolytic Therapy • Primary reperfusion • PE with hemodynamic instability • use in stable pt is contaversial . • Initiated within 48 hrs of symptoms can be extend upto 6-14 days of symptoms. • Aim to: Relievepulmonary vasculature obstruction, Improve right ventricular efficacy, Correct the hemodynamic instability. • Risk: Bleeding
- 46. Anticoagulation Therapy • Pt with PE should receive at least 3 months of Anticoagulation treatment. • Pt with cancer are candidate for indefinite treatment due to high recurrence rate (20% after 12 months of index event) • Parentral anticoagulation should be started immediately with thrombolysis in high/ intermediate high risk pt. • In Low risk/ intermediate low risk PE pt oral anti- coagulation (VKA/NOAC) to be started immediately • VKA should be started under cover of UFH/LMWH till INR 2-3 for two consecutive day. • Maintain INR 2-3 • Risk of bleeding: old age, GI bleed, Renal and hepatic disease etc.
- 47. Parenteral AnticoagulantTherapy UnfractionatedHeparin • Usedforprimaryreperfusion • Bolusdoseabout100U / kg body weight • MaintenanceDose 12U/kgivinfusion • Follow up byaPTT (1.5-2.0) • Preferredincreatinineclearance <30ml/kg/min 20/01/2016
- 48. LMWH • Preferred over UFH • Low risk of bleeding • No need for monitoring
- 49. LMWH
- 50. OralAnticoagulantTherapy • Warfarin • 3-5 mg/day orally with LMWH (5 daysto start acting) • Duration: 3-6 months • Monitor INR(2-3)
- 51. New Oral Anticoagulants Drug Dose Rivaroxaban (EINSTEIN-DVT2010/PE2012) 15mg BD x 3weeks then 20mg OD Dabigatran (RE-COVER2009/ RE- COVER ll 2014) 150mg twice a day (110 bd for elderly) Apixaban (AMPLIFY2013) 10mg BD x 7 days then 5mg BD
- 53. • IVC filter use is restricted to 1. Contraindication to anti-coagulation 2. Recurrent PE despite adequate anticoagulation • Retrievable IVC filters should be implanted and removed within 3 months if possible. • Routinely placing filters maybe harmful
- 54. Embolectomy • Surgical Embolectomy • Catheter Embolectomy • Massive life-threatening PE
- 55. Prevention • Prophylaxis is the single mostimportant measure for ensuring patient safety in hospitalizedpatients
- 56. RISK FACTOR SCORING Cancer 3 Previous VTE 3 Immobility 3 Thrombophilia 3 Trauma/surgery 2 Age ≥ 70 years 1 Heart/respiratory failure 1 Acute MI or stroke 1 Infection/rheumatologic disorder 1 Obesity 1 Hormonal treatment 1 Padua Prediction Score for Identification of Hospitalized Patients at Risk for Venous Thromboembolism High risk for developing PE is defined as 4 score points or greater.
- 57. Condition Prophylaxis Hospitalization with medical illness -Unfractionated heparin 5000 units SC bid or tid or - -Enoxaparin 40 mg SC qd or -Dalteparin 2500 units or 5000 units SC qd or -Fondaparinux 2.5 mg SC qd with normal renal function (in patients with a heparin allergy such as heparin-induced thrombocytopenia) or -Graduated compression stockings or intermittent pneumatic compression for patients with contraindications to anticoagulation -Consider combination pharmacologic and mechanical prophylaxis for high-risk patients General surgery -Unfractionated heparin 5000 units SC bid or tid or -Enoxaparin 40 mg SC qd or -Dalteparin 2500 or 5000 units SC qd Major orthopedic surgery -Warfarin (target INR 2 to 3) or Enoxaparin 30 mg SC bid or -Enoxaparin 40 mg SC qd or -Dalteparin 2500 or 5000 units SC qd or -Fondaparinux 2.5 mg SC qd or Rivaroxaban 10 mg qd or -Aspirin 81 mg qd or -Dabigatran 220 mg qd (not in the U.S.) or -Apixaban 2.5 mg twice daily (not in the U.S.) or -intermittent pneumatic compression (with or without pharmacologic prophylaxis)
- 58. Take home message • PE is common but overlooked • High suspicion to make diagnosis • D- dimer, Echo, CTPA diagnostic tools • Immediate reperfusion for high risk cases • Give anticoagulants to all for 6 months • Prophylaxis is important for hospitalized patients.
Notas do Editor
- Proposed diagnostic algorithm for patients with suspected not high-risk pulmonary embolism
