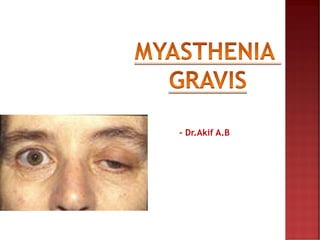
Myasthenia gravis
- 4. -100% specific -90% sensitivity in Generalised Myasthenia -50-70 % sensitivity in Ocular Myasthenia -False positives are very rare and may be seen in Lambert eoton syndrome, GVHD, Autoimmune liver disease, RA.
- 5. The anti–striated muscle (anti-SM) Ab refers to a class of antibodies against components of skeletal muscle including titin, the ryanodine receptor, myosin, and alpha-actin. Anti-SM Ab is present in about 70–80% of patients with thymoma and MG who are younger than 40 years 30% of adult patients with MG without thymoma 24% of patients with thymoma without MG. Thus, a positive test result should prompt a search for thymoma in patients younger than 40 years. In individuals older than 40 years, anti-SM Ab can be present without thymoma. anti–striated muscle ANTIBODY
- 6. About half of the patients with negative results for anti-AChR Ab (seronegative MG) may have positive test results for antibody to muscle-specific kinase (MuSK) -It is a Receptor tyrosine kinase that is essential for neuromuscular junction development. - Associated with more severe disease - Doesn’t responds to Acetylchoilnesterase Inhibitors Anti-lipoprotein-related protein 4 (LRP4) antibody Lipoprotein-related protein 4 is present on the postsynaptic membrane
- 7. Rheumatoid factor and antinuclear antibodies (ANAs) is indicated to rule out systemic lupus erythematosus (SLE) and rheumatoid arthritis (RA). Thyroid function tests are indicated to rule out associated Graves disease or hyperthyroidism. This is essential, especially in patients with ocular MG where the concomitant hyperthyroidism is most frequent. Other laboratory studies
- 8. On plain anteroposterior and lateral views, radiography may identify a thymoma as an anterior mediastinal mass. A negative chest radiograph does not rule out a smaller thymoma, in which case a chest computed tomography (CT) scan is required. Chest CT scan should be obtained to identify or rule out thymoma or thymic enlargement in all cases of MG, especially in elderly
- 9. It is essential to rule out mass lesions compressing the cranial nerves in strictly ocular MG. CT or preferably magnetic resonance imaging (MRI) of the brain and orbit is indicated.
- 10. 1) Repetitive stimulation of a muscle at 2-3 Hz, also known as repetitive nerve stimulation (RNS) 2) Single-fiber electromyography
- 11. Butterfly needle is placed in an accessible vein. A 2 mg test dose is administered initially If no response and no untoward effects are noted after 30 seconds 8 mg (0.8 mL) is injected in 2 mg increments every 10-15 seconds If the patient has objective improvement (improvement in ptosis or ophthalmoparesis) or a severe side effect, the test is aborted. Sinus bradycardia due to excessive cholinergic stimulation of the heart is a serious complication; consequently, an ampule of atropine(0.6mg) should be available at the bedside or in the clinic room while the test is performed. False positive : amyotrophic lateral sclerosis, LEMS, botulism, congenital myasthenic syndromes, and GBS
- 12. by cooling the tissues, and more specifically the skeletal muscle fibres, the activity of the acetylcholinesterases are inhibited
- 13. Drugs for symptomatic therapy Immunosuppressants and steroids
- 14. Drugs for symptomatic therapy - All subgroup responds to Acetyl cholinesterase inhibitors -Pyridostigmine is the Drug of choice -Neostigmine and Ambenonium chloride is also effective -Myasthenia gravis with MUSK+ responds least to symptomatic therapy. -Patients with mild diseases usually need no other therapy.
- 15. -Onset of action - 15-30min -Duration of action = 3-4hrs -Treatment generally begins with 30-60mg 3-4 times a day -Maximum dose = 120mg , 3-4 times a day -Overdose with anti cholinergics may cause increased weakness and SLUDGE.
- 16. Side effects of Cholinesterase Inhibitors -Increased salivation -Lacrimation -Urination -Diarrhea -Abdominal cramps(GIT) -Emesis
- 17. -Prednisone or prednisolone -Start at 15-20mg/day -Slowly increase by 5mg every 2-3days -Upto maximum of 60mg/day -Continue for 3 months -Put on alternate day therapy for 1-3months -Slowly taper
- 18. -Aim : to prevent generalisation of Disease -Low dose steroid is usually recommended for patients who have persistent symptoms and have other factors involved like positive antibodies or an enlarged Thymus.
- 19. -One of the most commonly used drug nowadays because of its efficiency and fewer side effects -Dose = 1-1.5g bd -M.O.A = Inhibition of Purine synthesis by denovo pathway -Lymphocytes have only denovo pathway, thus prevents proliferation whereas other cells have salvage pathway as well and hence are not affected. -It doesn’t kill preexisting Lymphocytes and thus its action takes months to act. Life span of lymphocyte : few weeks to few months. Side effects : GI symptoms and rarely leucopenia
- 20. INDICATIONS Patients not responding to steroids Patients not willing for steroids Combination therapy is better and avoids side effects - Dose is 2-3mg/kg
- 21. -Inhibits purine synthesis and thus cell proliferation -Active metabolite : 6-mercaptopurine -Strong effect on T and B cells -Thiopurine methyltransferase activity (metabolises azathioprine) should be checked because its absence may increase toxicity of Azathioprine - 0.3% of people doesn’t have these enzyme -Effect of Azathioprine takes months to appear, so till that time alternate medicine should be used
- 22. -Most common - Nausea and vomitings -Bone marrow suppression -So counts should be monitored during therapy -Very rarely Pancreatitis
- 23. -Methotrexate -Tacrolimus -Cyclosprine -Rituximab : 375mg/m2 i.v in 4 weekly infusions or 1gm i.v 2 doses, 2 weeks apart -Most guidelines recommend Mycophenolate mofetil for mild to moderate Myasthenia Gravis
- 25. -Myasthenia Gravis patients with Thymoma benefit with Thymectomy. -All Studies have shown that Thymectomy has a beneficial role in patients with Myasthenia whether or not they have Thymoma - It may lead to drug free remission as well Not recommended Patients with only ocular Myasthenia With MUSK+ or LRP4 antibodies All antibodies are negative -There is less evidence that Thymectomy prevents Generalisation of Disease -Thymectomy must be considered in patient with ocular Myasthenia only if symptomatic therapy has failed or they are positive for Acetyl Choline receptors and neurophysiological tests show possibility for Generalisation. Thymectomy should be considered in negative antibodies patient if drug therapy fails
- 27. Myasthenic crisis is a life-threatening condition which is defined as weakness from acquired myasthenia gravis that is severe enough to necessitate intubation or to delay extubation following surgery. The respiratory failure is due to weakness of respiratory muscles. Severe bulbar (oropharyngeal) muscle weakness When this results in upper airway obstruction or severe dysphagia with aspiration, intubation and mechanical ventilation are necessary. D/D : Cholinergic Crisis Treatment : Immunoglobulins or Plasmapheresis
- 28. -Muscles stop responding to the high quantity of Ach due to blockage of receptors, leading to flaccid paralysis, respiratory failure and SLUDGE - can be distinguished by Edrophonium test - Treatment : Atropine + other supportive measures
- 32. -Plasma which contains the pathological antibodies are mechanically separated from cells. -A course of 5 cycles (3-4l/cycle) over period of 10-14 days -Leads to significant improvement in symptoms Indications Myasthenia Crisis To improve patients condition prior to surgery (Thymectomy)
- 33. Indications Myasthenia Crisis To improve patients condition prior to surgery (Thymectomy) - 2gm/kg over 5 days i.e 400mg/kg/day
- 35. -Oral Prednisone or Pyridostigmine is safe during Pregnancy -Azathioprine and cyclosporine is safe as well -Methotrexate and Mycophenolate are contraindicated as they are teratogenic -Womens are advised to avoid pregnancy for upto 1 year after Rituximab therapy -Immunoglobulins and Plasmapheresis can be used in worsening Myasthenia -Lactation should be continued -Transient Myasthenia is seen in 15% of neonates due to transfer of IgG from mother