Abdominal wall defects
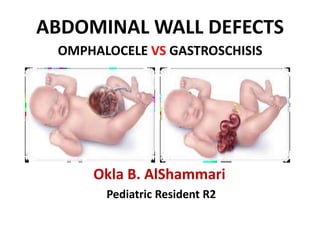
- 1. ABDOMINAL WALL DEFECTS OMPHALOCELE VS GASTROSCHISIS Okla B. AlShammari Pediatric Resident R2
- 2. OBJECTIVES • Epidemiology • Etiology • Pathophysiology • Clinical Features • Diagnosis • Management • Prognosis , long term outcomes.
- 3. Epidemiology Omphalocele * Incidence - 3 per 5,000 *M:F is 1.5:1 * >70% association with congenital anomalies such Bowel atresia, Imperforated anus, Trisomies 13, 18, 21, Beckwith-Wiedemann Syndrome Gastroschisis *Incidence - 4 per 10,000 *M:F is 1:1 • 10-15% association with congenital anomalies such as CHD(VSD), cleft palate and intestinal atresia • 40% are premature/SGA
- 4. Etiology Omphalocele *Congenital abdominal wall defect with protrusion of abdominal viscera contained within a parietal peritoneum and amniotic membranous sac with Wharton’s jelly. *Due to failure of the midgut to return to abdomen by the 10th week of gestation during midgut rotation. Gastroschisis *Congenital abdominal wall defect towards the right side of the umbilicus and protruded bowel is not covered by a membrane. * Failure of migration and fusion of the lateral folds of the embryonic disc on the 3rd-4th week of gestation. * Disruption of the right omphalomesenteric artery as midgut returns to abdomen by the 10th week of gestation causing ischemia of the abdominal wall and weakness then herniation. * Rupture of omphalocele
- 5. Risk Factors Omphalocele • Increased maternal age More than 40 yr • Twins • High gravida • Consecutive births Gastroschisis • Young maternal age • Low gravida • Prematurity • Low birth-weight secondary to IUGR
- 7. GASTROSCHISIS *Abnormal involution of right umbilical vein * Rupture of a small omphalocoele *Failure of migration and fusion of the lateral folds of the embryonic disc on the 3rd- 4th week of gestation
- 8. OMPHALOCELE Failure of the midgut to return to abdomen by the 10th week of gestation
- 9. Clinical Features GASTROSCHISIS Defect to the right of an intact umbilical cord allowing extrusion of abdominal content Umbilical cord arises from normal place in abdominal wall Opening <=5 cm No covering sac (never has a sac ) Evisceration usually only contains intestinal loops Bowels often thickened, matted and edematous 10-15% have associated anomalies 40% are premature/SGA OMPHALOCELE central defect of the abdominal wall beneath the umbilical ring. Defect may be 2-12 cm (Small- <5cm)(Large>8cm) Always covered by sac Sac is made of amnion, Wharton’s jelly and peritoneum The umbilical cord inserts directly into the sac in an apical or lateral position. Small one contains intestinal loops only. Large one may involve liver, spleen and bladder, testes/ovary >50% have associated anomalies
- 10. Diagnosis About 90% of GASTROSCHISIS and Omphalocele diagnosed prenatally. Maternal AFP usually elevated with fetal gastroschisis Alpha-feto-protein-synthesized in fetal liver and excreted by fetal kidneys and crosses placenta by 12weeks. Prenatal ultrasound after 14 weeks gestation is the confirmatory test.
- 11. Prenatal Ultrasound The diagnostic prenatal ultrasound findings of Gastroschisis are extraabdominal loops of bowel without covering sac
- 12. Prenatal Ultrasound The prenatal ultrasound findings of Omphalocele are abdominal organs herniated outside the abdominal cavity with an abnormal insertion of Umbilical cord into the membrane rather than into abdominal wall at midline on the mass Contents are intestinal loops and maybe liver, spleen and gonads.
- 13. Management Gastroschisis After delivery :- The perfusion of the herniated contents should be carefully evaluated . If bowel ischemia or infarction suspected > immediate surgical consultation is indicated. If the viscera are well perfused , it is important to next place a clear plastic bag over the exposed bowel as a temporary covering to minimize evaporative heat and fluid loss
- 14. Pre-operative Management • ABC • Heat Management – Sterile wrap or sterile bowel bag – Radiant warmer • Fluid Management – IV bolus 20 ml/kg LR/NS – D10¼NS 2-3 maintenance rate • Nutrition – TPN (central venous line ) • Abdominal Distention – OG/NG tube – urinary catheter • Infection Control Broad-spectrum antibiotics • Closure of the Defect
- 15. Surgical Management Gastroschisis The goal of surgical repair is safe the reduction of the eviscerated contents and eventual closure of the abdominal wall. – Primary Closure Use of own baby umbilical stump as biological dressing to seal gastroschisis defect without attempting a primary fascial closure – Staged Closure • Staged repair using silo pouch
- 16. Management Omphalocele:- Including the evaluation for associated anomalies and monitoring of fetal growth. Echocardiography : high risk for CHD Prenatal monitoring of fetal growth : high risk of IUGR . Other specific evaluation for associated pulmonary hypoplasia ( giant omphalocele ) Prenatal counseling about the expected hospital course and the long term prognosis
- 17. Cont management Omphalocele: After delivery :- The initial evaluation and resuscitation to a babies with an Omphalocele follow same protocol and sequences of all newborns. Should be handled carefully to prevent the omphalocele membrane from tearing. After initial stabilization for the newborn with omphalocele should be inspected to confirm that it is intact and then covered with a nonadherent dressing to protect the sac.
- 18. Cont management Omphalocele: Primary Closure Small defects (<4cm) excision of the sac and closure of the fascia and skin over the abdominal contents Mesh patch Medium defects (6-8cm) Conservative Large defect (10-12cm) apply topical application - Betadine ointment or silver sulfadiazine to make intact sac. till the baby is bigger and more able to tolerate major operation
- 19. Long term outcomes Gastroschisis : -Almost always with intestinal malrotation - Hernias at the site of repair. - Intestinal atresia. - Short bowel syndrome. Omphalocele: Small will recovery well The outcomes determine by the severity of associated anomalies , so babies with giant omphalocele have increased mortality and morbidity because of the large abdominal wall defect and associated pulmonary hypoplasia and pulmonary hypertension - GERD - Hernias - Respiratory infection - Failure to thrive
- 20. Thank you
