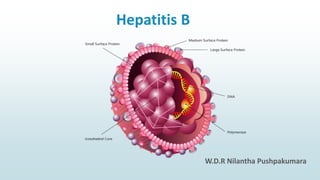
Hepatitis b virus
- 1. Hepatitis B W.D.R Nilantha Pushpakumara
- 2. Objectives • To determine what is hepatitis B ? • Transmission of hepatitis B virus • To determine symptoms after infection of hepatitis B • Preventive measures that can be taken to avoid transmission
- 3. Content ➢ What is hepatitis B ➢ Epidemiology of hepatitis B ➢ Causes for hepatitis B ➢ Transmission of hepatitis B virus ➢ Common ways of hepatitis B transmission ➢ Symptoms ➢ Diagnosis ➢ Treatment ➢ Prevention
- 4. What is Hepatitis B • Hepatitis B is a viral infection • that attack liver and can cause both acute and chronic diseases • It is the most serious type of viral hepatitis • Majority of patients with chronic HBV (CHB) infection will have chronic liver disease • Some with CHB infection develop a primary liver cancer, hepatocellular carcinoma (HCC) later in life
- 5. Hepatitis B in the World • Hepatitis B virus (HBV) infection is a global public health problem • 2 billion people have been infected • It is estimated that there are 248 million HBV carriers in the world (positive for hepatitis B surface antigen [HBsAg]) • 1 million people die each year from hepatitis B and its complications • Approximately 2 people die each minute from hepatitis B
- 6. In Sri Lanka • prevalence of HBV infection in Sri Lanka is estimated to be less than 2%
- 7. What causes hepatitis B ? • It is caused by hepatitis B Virus • It is a DNA virus
- 8. Transmission of hepatitis B (HBV) • The virus is highly contagious • Transmitted through contact with the blood or other body fluids of an infected person • Hepatitis B virus can survive outside of the body for at least 7 days • It is an important occupational hazard for health care workers
- 9. Concentration of Hepatitis B Virus in Various Body Fluids High Moderate Low/Not detectable Blood Semen Urine Serum Vaginal fluid Faeces Wound exudate Saliva Sweat Tears Breastmilk
- 10. Most common ways of hepatitis B transmission include : • Sexual contact • Sharing of injecting equipment (used for injecting drugs) • Needlestick injuries in a health care setting • Reuse of unsterilized or inadequately sterilized needles • Sharing personal items such as razors, toothbrushes, or hair and nail clippers • Perinatal Transmission Congenital or Vertical transmission is quite common from carrier mothers The risk to babies is high if the mother is HBeAg positive (60- 90%) and low if Negative (5-15%)
- 11. Needle stick injury sharing injecting drugs
- 12. unsterilized tattooing equipment contamination vaccine equipment unsterilized body piercing equipment
- 13. • Hepatitis B does NOT spread by contaminated food or water, and cannot spread through casual or social contact such as kissing, sneezing or coughing, hugging, or eating food prepared by a person with hepatitis B High Risk Groups • Injecting drug users • Sex workers • Men who have sex with men • Medical and paramedical personnel • People from endemic regions • Hemophiliacs and other patients requiring blood and blood product treatment
- 14. What are the symptoms • Feeling very tired • Mild fever • Headache • Loss of appetite • Nausea • Abdominal pain • Tan-colored bowel movements (stools) • Dark urine • Yellowish eyes and skin (jaundice). Jaundice usually appears only after other symptoms have started to go away
- 15. • Hepatitis B can also cause a chronic infection • This can later develop to cirrhosis or hepatocellular carcinoma
- 16. Diagnosis • Laboratory confirmation is essential • Number of blood tests are available to diagnose and monitor infected people • These tests can distinguish between chronic and acute infection • Laboratory detection mainly focuses on detection of Hepatitis B surface antigen • All donated blood is screened for Hepatitis B
- 17. Treatment • No specific treatment for acute Hepatitis B • Maintaining comfort and adequate nutrition balance is essential • Chronic infection is treated with oral antiviral agents • These medicines can slow the progression of cirrhosis, reduce liver cancers and improve the life span
- 18. Prevention To avoid transmission of hepatitis B: • consider being vaccinated • practice safer sex (use a condom) • wash hands after touching blood or body fluids • wear disposable gloves if giving someone first aid, or cleaning up blood or body fluids • avoid sharing toothbrushes, razors, needles, syringes, personal hygiene items and grooming aids or any object that may come into contact with blood or body fluids
- 19. • Use new and sterile injecting equipment for each injection • Cover all cuts and open sores with a band aid or bandage • Wipe up any blood spills and then clean the area with household bleach • Throw away personal items such as tissues, menstrual pads, tampons and bandages in a sealed plastic bag.
