Digestivesystem jaita
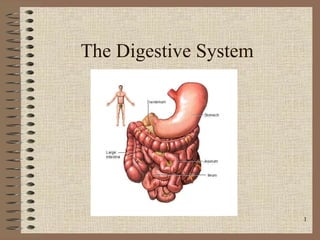
- 1. The Digestive System 1
- 2. Objective • At the end of the class students will be able to: - explain about the structure of alimentary tract & it’s accessory organs of digestion - explain about various alteration in diseases - apply & implicate the knowledge in day to day practice
- 3. • Digestive system = alimentary canal + accessory organs + variety of digestive processes.
- 4. Alimentary canal or Gastrointestinal (GI) tract • Mouth • Pharynx • Oesophagus • Stomach • Small intestine • Large intestine • Rectum & Anal canal
- 5. The Components of the Digestive System
- 6. Accessory organs • Glands situated out side of the tract; secretions pass through ducts to enter the tract: - 3 pairs of salivary glands • Parotid in front of ear • Submandibular below lower jaw • Sublingual below tongue - The pancreas - The liver & biliary tract
- 7. The Major Salivary Glands 7
- 8. Duct System
- 9. Digestive processes • Ingestion: • Propulsion: • Digestion: • Absorption: • Elimination:
- 10. General structures/ Layers of Digestive System
- 11. • Modified in different levels according to process • Inner Epithelial layer/ Mucosa – Soft and pink in colour – 3 layers Mucous membrane (innermost; columnar epithelium with goblet cells; protection, secretion, absorption) Lamina propria (loose connective tissue; supports blood vessels & lymphoid tissue) Muscularis mucosa (thin outer layer; smooth muscle) – Secretion of enzyme and mucus
- 12. • Mucous membrane secrets digestive juices: saliva from the salivary glands Gastric juice from gastric glands Intestinal juice from intestinal glands Pancreatic juice from pancreas Bile from liver • Also secrets mucus from goblet cells. 12
- 13. • Sub- mucosa – Connective tissue (binds muscle layer to mucosa) • Muscular layer – Outer layer (Longitudinal muscles) – Inner layer (Circular muscle) Between these two layers: blood vessels, lymph vessels & a plexus (network) of sympathetic& parasympathetic nerves (myenteric plexus or Auerbach’s plexus) – Peristalsis (Segmental contraction) 13
- 14. • Outer Serous layer or Adventitia – Protective function – In abdomen organs are covered by a serous membrane (peritoneum) Parietal peritoneum: lines the abdominal wall Visceral peritoneum: covers the organs (viscera) within the abdominal & pelvic cavities. Home work: explain about peritoneum in detail. 14
- 15. Anatomy of the Mouth and Throat 15
- 16. Mouth or oral cavity • Is bounded by muscles & bones: Anteriorly: by the lips Posteriorly: continuous with oropharynx Laterally: by the muscles of the cheeks Superiorly: by bony hard palate & muscular soft palate Inferiorly: by the muscular tongue & soft tissues of the floor of the mouth 16
- 17. • Vestibule: part of mouth between gums & cheeks. • Remainder of the cavity: oral cavity • Palate: forms the roof of mouth; has 2 parts Anterior hard palate: formed by maxilla & palatine bone Posterior soft palate: muscular curves from back of hard palate & blends with the wall of pharynx at side. 17
- 18. • Uvula: curved fold of muscle covered with mucous membrane, hanging down from middle of free border of soft palate. • Palatine tonsil: collection of lymphoid tissue on each side between the arches. 18
- 19. Tongue 19
- 20. • Voluntary muscle structure • Attached to hyoid bone at base • Attached to floor of the mouth by a fold of its mucous membrane covering: frenulum • Superior surface: numerous papillae (small projections); many of these contain sensory receptors (test buds) 20
- 21. Blood supply: lingual branch of external carotid artery; venous drainage by lingual vein Nerve supply: hypoglossal nerves (12th cranial nerve)- supply voluntary muscles; lingual branch of mandibular nerves (arises from 5th cranial nerve)- pain, temperature & touch; facial & glossopharyngeal nerves (7th & 9th cranial nerves)- nerves of taste 21
- 22. Functions of tongue • Chewing (mastication) • Swallowing (deglutition) • Speech • Taste 22
- 23. Teeth 23
- 24. • Embedded in the alveoli or sockets of the alveolar ridges of the mandible & the maxilla. • Temporary or deciduous teeth: babies born with two sets (dentitions) • 20 temporary teeth (10 in each jaw); erupt at about 6 months; should be present by 24 months • Permanent teeth begin to replace deciduous teeth in 6th year; 32 teeth; usually complete by 21st year 24
- 25. Functions of the teeth • Incisors & canine teeth: cutting teeth; used for biting pieces of food • Premolar & molar teeth: broad, flat surface; used for grinding or chewing food 25
- 26. Structure of tooth • Crown: part that protrudes from gum • Root: part embedded in bone • Neck: narrowed region between crown & root. • Blood supply: maxillary artery; jugular veins • Nerve supply: upper teeth maxillary nerves; lower teeth mandibular nerves. Both are branches of trigeminal nerves (5th cranial nerve) 26
- 27. Salivary glands 27
- 28. Parotid glands • Each side of the face just below the external acoustic meatus. • Each gland has a parotid duct opening in mouth at the level of 2nd upper molar tooth. 28
- 29. Sub- mandibular glands • One on each side of face under angle of jaw. • 2 submandibular ducts open on the floor of the mouth (each side of the frenulum of tongue) 29
- 30. Sublingual glands • Lie under the mucus membrane of the floor of mouth in front of submandibular glands • Have numerous small ducts that open into the floor of mouth 30
- 31. Salivary Glands • Produce and secrete saliva that: – Cleanses the mouth – Moistens and dissolves food chemicals – Aids in bolus formation – Chemical digestion of Food
- 32. Saliva • 1-1.5 litre/day; pH slightly acidic (6.8) Composition • Mostly water 97 to 99.5% • Mucus • Mineral salts • A digestive enzyme: salivary amylase • Lysozyme • Immunoglobulin • Blood clotting factors
- 33. Secretion of saliva • Secretion is under autonomic nervous system • Parasympathetic stimulation causes: profuse secretion of watery saliva with a relatively low content of enzymes & other organic substances • Sympathetic stimulation causes: secretion in small amount of saliva rich in organic materials specially from sub mandibular glands 33
- 34. Functions of saliva • Chemical digestion of polysaccharides Saliva contains enzyme amylase: break down of complex sugars (starch to disaccharide maltose) • Lubrication of food made a bolus ready for swallowing • Cleaning & lubricating the mouth prevents damage to mucous membrane by rough & abrasive food 34
- 35. • Non- specific defence lysozyme, immunoglobulin & clotting factors combat invading microbes • Taste test buds are stimulated only by chemical substances; thus dry foods only stimulate the sense of taste after thorough mixing with saliva 35
- 36. Pharynx • Connects nasal and oral cavities with larynx & oesophagus • force food down during swallowing • Divisions Nasopharynx (important in respiration) Oropharynx & Laryngopharynx (both are common passage to both respiratory & digestive system)
- 37. 37
- 38. • Blood supply: several branches of facial arteries; venous drainage: into facial veins & internal jugular veins • Nerve supply: sympathetic from cervical ganglia; parasympathetic by glossopharyngeal & vagus nerves 38
- 39. Oesophagus
- 40. Esophagus – 25cm long muscular tube; 2cm diameter – From pharynx to stomach – Behind trachea and in front of vertebral column – Food passes to stomach by active muscular action – As it passed through diaphragm it curves upward: prevents regurgitation (backflow) of gastric content 40
- 41. Oesophagus contd. – Closed with two sphincters (upper: cricopharyngeal or upper oesophageal sphincter; lower: cardiac or lower oesophageal sphincter) – Solid food reaches stomach in 7 to 8 seconds – Liquids reaches stomach in 2 to 3 seconds • Functions – Secrete mucous – Transport food 41
- 42. • Blood supply: - Thoracic region- paired oesophageal arteries; venous drainage: azygous & hemizygous veins - Abdominal region- branches from inferior phrenic arteries & left gastric branch of coeliac artery; Venous drainage in left gastric vein 42
- 43. Anatomy of the Stomach 43
- 44. Stomach • Usually “J” shaped; 1.5lt or more in adult • 2 sphincters: cardiac & pyloric 44
- 45. Organs associated with stomach • Anteriorly: left lobe of liver & abdominal wall • Posteriorly: abdominal aorta, pancreas, spleen, left kidney & adrenal gland • Superiorly: diaphragm, oesophagus & left lobe of liver • Inferiorly: transverse colon & small intestine • To the left: diaphragm & spleen • To the right: liver & duodenum 45
- 46. Walls of stomach • Consists of 3 layers instead of 2. Outer: longitudinal fibres Middle: circular fibres Inner: oblique fibres • This arrangement allows churning motion as well as peristaltic movement. • Circular muscle is strongest in the pylorus & pyloric sphincter 46
- 47. • Mucosa of stomach: When empty: thrown into longitudinal folds or rugae When full: rugae are ironed out & surface has a smooth, velvety appearance. Numerous gastric glands situated below mucous membrane & open on to it: secrets gastric juice 47
- 48. • Mucous membrane – G cells – secret gastrin – Goblet cells – secret mucous – Gastric pit has Oxyntic gland – Parietal cells – secret HCl – Chief cells or Zymogenic cells • Pepsin • Gastric lipase 48
- 50. • Blood supply: Arterial supply: left gastric artery, a branch of coeliac artery, right gastric artery & gastroepiploic arteries. Venous drainage: through veins of corresponding names into the portal vein 50
- 51. Gastric juice • About 2 lt of gastric juice/ day • Consist of: Water (by gastric glands) Mineral salts (by gastric glands) Mucus (mucous cells) HCL (parietal cells) Intrinsic factor (parietal cells) Inactive enzyme precursors: pepsinogen by chief cells 51
- 52. Functions of gastric juice • Water further liquefies the food swallowed • HCL: Acidifies the food & stops action of salivary amylase Kills ingested microbes Provides acid environment needed for effective digestion by pepsins 52
- 53. • Pepsinogens: are activated to pepsins by HCL acid & pepsins already present in the stomach These enzymes begin the digestion of proteins. Pepsins are more effective at a very low pH (1.5-3.5) 53
- 54. • Intrinsic factor (a protein): needed for absorption of vit B12 from ileum • Mucus: prevents mechanical injury to the stomach wall by lubricating the contents Prevents chemical injury by acting as a barrier between stomach wall & corrosive gastric juice 54
- 55. Secretion of gastric juice • Always a small quantity of gastric juice present in the stomach (even if no food) = “fasting juice” • Max. level: about 1 hr after a meal • Declines to fasting level after about 4 hrs. • 3 phases of secretion of gastric juice Cephalic phase Gastric phase Intestinal phase 55
- 56. Cephalic Phase
- 57. Cephalic phase • This flow of juice occurs before food reaches the stomach • Due to reflex stimulation of vagus (parasympathetic) nerves initiated by the sight, smell or test of food. 57
- 58. Gastric phase stimulated by the presence of food the in the pyloric antrum duodenum secret gastrin (circulating in blood) blood which supplies the stomach stimulates the gastric glands to produce more gastric juice Gastric phase secretion is suppressed when the pH in the pyloric antrum falls to about 1.5 58
- 59. Gastric Phase
- 60. Gastric Phase • Distention of the stomach activates a parasympathetic reflex. Action potentials are carried by the vagus nerves to the medulla oblongata. • Medulla oblongata stimulates further secretions of the stomach. • Distention also stimulates local reflexes that amplify stomach secretions.
- 61. Intestinal Phase • Chyme in the duodenum with a pH less than 2 or containing lipids inhibits gastric secretions by 3 mechanisms • Sensory input to the medulla from the duodenum inhibits the motor input from the medulla to the stomach. Stops secretion of pepsin and HCl. • Local reflexes inhibit gastric secretion • Secretin, gastric inhibitory polypeptide, and cholecystokinin produced by the duodenum inhibit gastric secretions in the stomach. (Enterogastrone)
- 62. Intestinal Phase
- 63. Intestinal phase • When the partially digested contents of the stomach reach the small intestine, a hormone complex enterogastrone is produced which slows down the secretion of gastric juice & reduces gastric motility. • Two hormones forming this complex are secretin & cholecystokinin (CCK) • Enterogastrone (any hormone or combination of hormones released by the intestine that inhibits gastric secretion.) 63
- 64. • By slowing the emptying rate of the stomach, the contents of the duodenum become more thoroughly mixed with bile & pancreatic juice. • This phase of gastric secretion is most marked when the meal has had a high fat content 64
- 65. 65
- 66. Functions of Stomach – Mix food – Limited absortion of – Reservoir • Alcohol – Mechanical digestion • Water – Chemical digestion of • B 12 • Protein – Storage of food for 3 • Nucleic acids hours • Fats – Partial digestion of – Activates some enzymes proteins and fats – Destroy some bacteria – Outward movement of – Dissolving out iron from content of pyloric end food of the stomach 66
- 67. Small Intestine • Extends from pyloric sphincter ileocecal valve – 6 to 7 meter long, 2.5cm diameter – Lies in center of abdomen – Divided into 3 parts • First part – Duodenum • Second part – Jejunum • Third part – ileum 67
- 68. Small Intestine • Alkaline Secretions – Protects from acid contents of stomach • Small intestine – Mucosa • Deeply folded to increase the surface area (villi) • Helps in absorption of food. • Movements – Segmentation – Peristalsis 68
- 69. Segmentation & Peristalsis • Peristalsis: is a radially symmetrical contraction and relaxation of muscles which propagates in a wave down the muscular tube, in an anterograde fashion. In humans, peristalsis is found in the contraction of smooth muscles to propel contents through the digestive tract. • Segmentation: Most areas of the small intestine and some portions of the large intestine undergo cycles of contraction that churn and fragment the bolus, mixing the contents with intestinal secretions
- 70. Peristalsis and Segmentation 70
- 71. 71
- 72. Small Intestine cont. • Structural modifications of the small intestine wall increase surface area – Plicae circulares: deep circular folds of the mucosa and submucosa – Villi – fingerlike extensions of the mucosa – Microvilli – tiny projections of absorptive mucosal cells’ plasma membranes
- 73. Small Intestine
- 74. Structure of the Villi in the Small Intestine 74
- 75. Small Intestine • Requires pancreatic enzymes & bile to complete digestion • Blood supply: Superior mesenteric artery; superior mesenteric vein 75
- 76. Large Intestine • Extends from ileocecal valve to anus – 1.5meter long, 5 to 6cm diameter • Regions – Cecum – Colon: Divided into 3 parts • Right ascending colon • Transverse colon • Left descending colon – Appendix (Epiploic appendages) – Rectum – Anal canal 76
- 77. Large Intestine • Cecum – 1st part of large intestine, Blind sac, appendix attached • Colon – Ascending, transverse, descending, sigmoid • Rectum – Straight muscular tube, 13cm long, between sigmoid colon & anal canal • Anal canal: 3.8cm long – Internal anal sphincter (smooth muscle) – External anal sphincter (skeletal muscle)
- 79. Large Intestine – No villi – No permanent circular folds – Longitudinal muscle is modified: collected into 3 bands • Taeniae coli (Haustra) – Otherwise like rest of Gl tract 79
- 80. Large intestine • Blood supply: - Inferior mesenteric artery, middle & inferior rectal arteries; - Superior & inferior mesenteric vein 80
- 81. Functions of Large Intestine • Absorption • Microbial activity (large no. of microbes synthesize vitamin K & folic acid):E. coli, Streptococcus faecalis etc. • Mass movement • Defecation 81
- 82. Feces Formation and Defecation • Sigmoid Colon & • Defecation – Peristalsis pushes feces Rectum into rectum – Temporary storage of – Rectal walls stretch faeces • Control • Chyme dehydrated to – Parasympathetic form feces • Feces composition – Voluntary – Water – Inorganic salts – Epithelial cells – Bacteria – Byproducts of digestion 82
- 83. The Liver • The largest gland in the body • Performs metabolic and hematological regulation and produces bile • Location – R. Hypochondrium – Epigastric region
- 84. Organs associated with liver • Superiorly & anteriorly: diaphragm & anterior abdominal wall • Inferiorly: stomach, bile ducts, duodenum, hepatic flexure of the colon, right kidney & adrenal gland • Posteriorly: oesophagus, inferior vena cava, aorta, gall bladder, vertebral column, diaphragm • Laterally: lower ribs & diaphragm 84
- 85. Liver • 4 Lobes – Left – Quadrate – Caudate – Right 85
- 86. The Liver
- 87. • Each lobe has lobules (tiny functional units) – hexagonal in shape; • Lobules contains hepatocytes: arranged in pairs of column • Between 2 pairs of column of cells are sinusoids (blood vessels with incomplete walls – Feed into central vein (mix blood from portal vein & hepatic artery) • Kupffer cells (Hepatic macrophages): within sinusoids; ingest & destroy worn out blood cells & any foreign particles present in blood 87
- 90. Liver • Dual blood supply – Hepatic portal vein – Hepatic artery/vein 90
- 91. Blood and Bile Flow
- 92. Liver Functions •Carbohydrate, fat, protein metabolism •Synthesis of bile •Formation of urea •Detoxification of drugs, alcohol •Destruction of RBC •Storage of excess glucose in form of glycogen •Storage of Vitamin A & D •Storage of Hemoglobin •Activates vitamin D •Fetal RBC production •Phagocytosis •Manufacturing of prothrombin & fibrinogen 92
- 93. The Pancreas • Pale gray gland; (Both exocrine & endocrine gland) • In epigastric & left hypochondriac regions; posterior to stomach • Weighing 60 gm; 12-15cm long • Parts of pancreas – Broad Head (lies in curve of duodenum) – Body (behind the stomach) – Narrow Tail (infront of left kidney just reaches the spleen) • Abdominal aorta & inferior vena cava lie behind
- 94. Tail Pancreas Body Head 94
- 95. The Pancreas • Endocrine functions – Groups of specialized cells (pancreatic islets of Langerhans): have no ducts; hormones diffuse directly into blood. – Secrets Insulin, Glucagon (controls blood glucose)
- 96. • Exocrine functions – Majority of pancreatic secretions – Consists of a large number of lobules made up of small alveoli (walls consists of secretory cells) – Each lobules is drained by tiny duct (unite to form pancreatic duct): joins with common bile duct (forms hepatopancreatic ampulla) & opens into duodenum – Duodenal opening of ampulla is controlled by hepatopancreatic sphincter (sphincter of Oddi) 96
- 97. The Pancreas – Produces pancreatic juice containing enzymes – Pancreatic juice digests • Carbohydrate • Proteins • Fats
- 99. Pancreas • Blood supply: Arterial supply: splenic & mesenteric arteries; Venous drainage: splenic & mesenteric veins joins to form portal vein 99
- 100. Biliary tract • Consists of bile duct & gall bladder 100
- 101. Bile ducts • Right & Left Hepatic ducts merge Common hepatic duct (7.5 cm long, 6mm diameter) • Common hepatic duct joins Cystic duct from gallbladder Common Bile duct • Bile duct joins Pancreatic duct at Hepatopancreatic ampulla and enters duodenum • Hepatopancreatic sphincter regulates passage of bile and pancreatic juices into duodenum
- 102. 102
- 103. The Gallbladder • Hollow, pear-shaped sac; attached to posterior surface of liver • Has a fundus (expanded end) & body (main part) & neck (continuous with cystic duct) • Stores, modifies and concentrates bile • Releases bile via the cystic duct, which flows into the bile duct • Blood supply: - Cystic artery (branch of hepatic artery) - Cystic vein (joins portal vein)
- 104. Functions of gall bladder • Reservoir for bile • Secretion of mucus into the bile • Absorption of water so that it is 10-15 times more concentrated than liver bile • Release of stored bile 104
- 105. Metabolism • Carbohydrate • Protein • Fat 105
- 106. Digestive processes • Ingestion: taking food in GI tract (eating, drinking) • Propulsion: mixes & moves the contents along GI tract.
- 107. Digestive processes cont. • Digestion: Mechanical breakdown of food (mastication) & chemical digestion (by enzymes of secretion produced by glands & accessory organs.
- 108. Digestive processes cont. • Absorption: digested food substances pass through the walls of some organs of GI tract into blood & lymph capillaries for circulation &use by body cell
- 109. Digestive processes cont. • Elimination: food substances which can not be digested & absorbed excreted as faeces by the process of defaecation.
- 110. oral cavity/teeth/salivary glands oropharynx/epiglottis oesophagus The path of food: stomach small intestine: duodenum small intestine: jejunum small intestine: ileum large intestine: ascending colon large intestine: transverse colon large intestine: descending colon sigmoid colon rectum anus
- 111. Diseases of mouth • Inflammation: thrush, angular cheilitis, gingivitis, stomatitis, • Viral infection • Tumors of mouth: squamous cell carcinoma • Developmental defects: cleft palate & cleft lip 111
- 112. Diseases of pharynx • Tonsillitis • Diphtheria 112
- 113. Diseases of salivary glands • Mumps • Calculus formation • tumors 113
- 114. Diseases of oesophagus • Esophageal varices • Inflammatory conditions • Spontaneous rupture of oesophagus • Tumors • Congenital malformation 114
- 115. Diseases of the stomach • Gastritis • Peptic ulceration • Tumors of stomach • Congenital pyloric stenosis 115
- 116. Diseases of the intestine • Appendicitis • Microbial disease: typhoid fever, paratyphoid fever, infection, food poisoning, cholera, dysentery • Inflammatory bowel disease: crohn’s disease, ulcerative colitis, tumors, hernias, intestinal obstruction etc 116
- 117. Diseases of pancreas • Acute pancreatitis • Chronic pancreatitis • Tumors 117
- 118. Disease of liver • Acute hepatitis • Chronic hepatitis • Non- viral inflammation of liver: liver abscess, cirrhosis of liver, liver faliure, hepatic encephalopathy, blood coagulation defect, ascites etc. • Tumors of the liver 118
- 119. Disease of gall bladder & bile duct • Gall stones (cholelithiasis) • Tumors • Jaundice • Cholecystitis 119
Notas do Editor
- Insert Process Fig. 24.13 A. Insert Animation: Three Phases of Gastric Secretion.exe
- Insert Process Fig. 24.13 B with verbiage. Insert Animation: Three Phases of Gastric Secretion.exe
- Insert Process Fig. 24.13 B with verbiage. Insert Animation: Three Phases of Gastric Secretion.exe
