upper GIT symptoms and role of endoscopy.pptx
•Transferir como PPTX, PDF•
0 gostou•73 visualizações
An Overview for beginners. Giving easy to learn general information about upper git endoscopy
Denunciar
Compartilhar
Denunciar
Compartilhar
Recomendados
Mais conteúdo relacionado
Semelhante a upper GIT symptoms and role of endoscopy.pptx
Semelhante a upper GIT symptoms and role of endoscopy.pptx (20)
Endoscopic Techniques & Imaging Technologies in Surgical Diseases-Basic Princ...

Endoscopic Techniques & Imaging Technologies in Surgical Diseases-Basic Princ...
Part IV Gasitrointesitinal disorders pharmacotherapy.pptx

Part IV Gasitrointesitinal disorders pharmacotherapy.pptx
Último
PEMESANAN OBAT ASLI : +6287776558899
Cara Menggugurkan Kandungan usia 1 , 2 , bulan - obat penggugur janin - cara aborsi kandungan - obat penggugur kandungan 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 bulan - bagaimana cara menggugurkan kandungan - tips Cara aborsi kandungan - trik Cara menggugurkan janin - Cara aman bagi ibu menyusui menggugurkan kandungan - klinik apotek jual obat penggugur kandungan - jamu PENGGUGUR KANDUNGAN - WAJIB TAU CARA ABORSI JANIN - GUGURKAN KANDUNGAN AMAN TANPA KURET - CARA Menggugurkan Kandungan tanpa efek samping - rekomendasi dokter obat herbal penggugur kandungan - ABORSI JANIN - aborsi kandungan - jamu herbal Penggugur kandungan - cara Menggugurkan Kandungan yang cacat - tata cara Menggugurkan Kandungan - obat penggugur kandungan di apotik kimia Farma - obat telat datang bulan - obat penggugur kandungan tuntas - obat penggugur kandungan alami - klinik aborsi janin gugurkan kandungan - ©Cytotec ™misoprostol BPOM - OBAT PENGGUGUR KANDUNGAN ®CYTOTEC - aborsi janin dengan pil ©Cytotec - ®Cytotec misoprostol® BPOM 100% - penjual obat penggugur kandungan asli - klinik jual obat aborsi janin - obat penggugur kandungan di klinik k-24 || obat penggugur ™Cytotec di apotek umum || ®CYTOTEC ASLI || obat ©Cytotec yang asli 200mcg || obat penggugur ASLI || pil Cytotec© tablet || cara gugurin kandungan || jual ®Cytotec 200mcg || dokter gugurkan kandungan || cara menggugurkan kandungan dengan cepat selesai dalam 24 jam secara alami buah buahan || usia kandungan 1_2 3_4 5_6 7_8 bulan masih bisa di gugurkan || obat penggugur kandungan ®cytotec dan gastrul || cara gugurkan pembuahan janin secara alami dan cepat || gugurkan kandungan || gugurin janin || cara Menggugurkan janin di luar nikah || contoh aborsi janin yang benar || contoh obat penggugur kandungan asli || contoh cara Menggugurkan Kandungan yang benar || telat haid || obat telat haid || Cara Alami gugurkan kehamilan || obat telat menstruasi || cara Menggugurkan janin anak haram || cara aborsi menggugurkan janin yang tidak berkembang || gugurkan kandungan dengan obat ©Cytotec || obat penggugur kandungan ™Cytotec 100% original || HARGA obat penggugur kandungan || obat telat haid 1 bulan || obat telat menstruasi 1-2 3-4 5-6 7-8 BULAN || obat telat datang bulan || cara Menggugurkan janin 1 bulan || cara Menggugurkan Kandungan yang masih 2 bulan || cara Menggugurkan Kandungan yang masih hitungan Minggu || cara Menggugurkan Kandungan yang masih usia 3 bulan || cara Menggugurkan usia kandungan 4 bulan || cara Menggugurkan janin usia 5 bulan || cara Menggugurkan kehamilan 6 Bulan
________&&&_________&&&_____________&&&_________&&&&____________
Cara Menggugurkan Kandungan Usia Janin 1 | 7 | 8 Bulan Dengan Cepat Dalam Hitungan Jam Secara Alami, Kami Siap Meneriman Pesanan Ke Seluruh Indonesia, Melputi: Ambon, Banda Aceh, Bandung, Banjarbaru, Batam, Bau-Bau, Bengkulu, Binjai, Blitar, Bontang, Cilegon, Cirebon, Depok, Gorontalo, Jakarta, Jayapura, Kendari, Kota Mobagu, Kupang, LhokseumaweCara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...Cara Menggugurkan Kandungan 087776558899
Último (20)
❤️Amritsar Escorts Service☎️9815674956☎️ Call Girl service in Amritsar☎️ Amri...

❤️Amritsar Escorts Service☎️9815674956☎️ Call Girl service in Amritsar☎️ Amri...
Call Girls in Lucknow Just Call 👉👉 8875999948 Top Class Call Girl Service Ava...

Call Girls in Lucknow Just Call 👉👉 8875999948 Top Class Call Girl Service Ava...
💰Call Girl In Bangalore☎️7304373326💰 Call Girl service in Bangalore☎️Bangalor...

💰Call Girl In Bangalore☎️7304373326💰 Call Girl service in Bangalore☎️Bangalor...
Call Girls Kathua Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Kathua Just Call 8250077686 Top Class Call Girl Service Available
Low Cost Call Girls Bangalore {9179660964} ❤️VVIP NISHA Call Girls in Bangalo...

Low Cost Call Girls Bangalore {9179660964} ❤️VVIP NISHA Call Girls in Bangalo...
Independent Bangalore Call Girls (Adult Only) 💯Call Us 🔝 7304373326 🔝 💃 Escor...

Independent Bangalore Call Girls (Adult Only) 💯Call Us 🔝 7304373326 🔝 💃 Escor...
Pune Call Girl Service 📞9xx000xx09📞Just Call Divya📲 Call Girl In Pune No💰Adva...

Pune Call Girl Service 📞9xx000xx09📞Just Call Divya📲 Call Girl In Pune No💰Adva...
Gastric Cancer: Сlinical Implementation of Artificial Intelligence, Synergeti...

Gastric Cancer: Сlinical Implementation of Artificial Intelligence, Synergeti...
Call Girls in Lucknow Just Call 👉👉8630512678 Top Class Call Girl Service Avai...

Call Girls in Lucknow Just Call 👉👉8630512678 Top Class Call Girl Service Avai...
Premium Call Girls Dehradun {8854095900} ❤️VVIP ANJU Call Girls in Dehradun U...

Premium Call Girls Dehradun {8854095900} ❤️VVIP ANJU Call Girls in Dehradun U...
Gorgeous Call Girls Dehradun {8854095900} ❤️VVIP ROCKY Call Girls in Dehradun...

Gorgeous Call Girls Dehradun {8854095900} ❤️VVIP ROCKY Call Girls in Dehradun...
Premium Call Girls Nagpur {9xx000xx09} ❤️VVIP POOJA Call Girls in Nagpur Maha...

Premium Call Girls Nagpur {9xx000xx09} ❤️VVIP POOJA Call Girls in Nagpur Maha...
Call Girls Shahdol Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Shahdol Just Call 8250077686 Top Class Call Girl Service Available
❤️Chandigarh Escorts Service☎️9814379184☎️ Call Girl service in Chandigarh☎️ ...

❤️Chandigarh Escorts Service☎️9814379184☎️ Call Girl service in Chandigarh☎️ ...
Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...
💰Call Girl In Bangalore☎️63788-78445💰 Call Girl service in Bangalore☎️Bangalo...

💰Call Girl In Bangalore☎️63788-78445💰 Call Girl service in Bangalore☎️Bangalo...
Kolkata Call Girls Shobhabazar 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Gir...

Kolkata Call Girls Shobhabazar 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Gir...
7 steps How to prevent Thalassemia : Dr Sharda Jain & Vandana Gupta

7 steps How to prevent Thalassemia : Dr Sharda Jain & Vandana Gupta
Circulatory Shock, types and stages, compensatory mechanisms

Circulatory Shock, types and stages, compensatory mechanisms
Call Girl In Indore 📞9235973566📞 Just📲 Call Inaaya Indore Call Girls Service ...

Call Girl In Indore 📞9235973566📞 Just📲 Call Inaaya Indore Call Girls Service ...
upper GIT symptoms and role of endoscopy.pptx
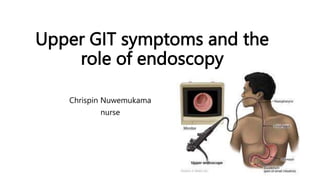
- 1. Upper GIT symptoms and the role of endoscopy Chrispin Nuwemukama nurse
- 2. Presentation outline • Learning objectives • The Upper GIT Anatomy • Examples of upper GIT diseases • Examples of UGIT symptoms • Risk Factors For upper GIT D’se • Definition of upper gi endoscopy • Uses • Indications • Patient preparation • Additional tests • complications
- 3. Learning objectives • To understand what the upper GIT is. • To identify upper GI symptoms and signs among patients. • To know when endoscopy should be done • To know the uses/roles of endoscopy in patient management • To learn how to prepare a patient for endoscopy
- 4. Reasons for discussing upper GIT/symptoms diseases • They are common, especially in outpatient departments. • And cause Significant morbidity among adults • To increase on the awareness among medical staff about the treatment options available especially the role of Endoscopy • As a reminder, trigger for everyone to actively participate in investigating upper GI symptoms
- 5. What’s the Upper GIT? -- Anatomy • For endoscopic purposes, upper GI includes the • esophagus, • stomach and • duodenum. • It ends at the duodenojejunal junction (ligament of trietz) • And lower GI includes the • anus, rectum, colon and cecum.
- 6. Examples of upper GIT diseases • Acute • Gastritis • Duodenitis • Esophagitis • PUD • GERD • Chronic • MALIGNANT/pre-malignant • Ca stomach • Ca esophagus • Burret esophagus • NON-malignant • Varices • Chronic gastroduodenitis • Strictures • Achalasia • Hernias • Polyps and other growths • Mallory-weis tear
- 7. Examples of UGIT symptoms • Epigastric pain, peri-umbilical pain • Heartburn • Sometimes chest pain • Vomiting, Nausea, Anorexia • Dyspepsia/indigestion • Dysphagia (difficulty in swallowing) • Regurgitation/Reflux/waterbrash sensation. • Retching • Gaseous abdomen/bloating • belching • Malaise • Weight loss • Anemia • Melena stools • hematemesis
- 8. Symptoms that signify chronic disease • Progressive vomiting • Progressive weight loss • Evening fevers, night sweats, (B-symptoms) • Unexplained anemia
- 9. Risk factors for upper git d’se • Age >40yrs, >60yrs • H. pylori infections • Longterm use of high dose NSAIDs • Highly spiced foods • Heavy alcohol consumption • Long spells of hunger, irregular meals • Physical inactivity • Physiological Stress • Family h/o malignancy e.g ca stomach • Genetic predisposition
- 10. UPPER GI ENDOSCOPY aka – Esophagogastroduodenoscpy (EGD) • DEFINITION. • Is a procedure used to examine the lining of the upper digestive tract, using an endoscope (a flexible tube with a camera & light at its end) • Is an intermediate surgical procedure, done under light
- 11. Endoscopy • It’s an outpatient procedure if the patient is stable (without compelling comorbidities) • Is used to investigate the cause of symptoms, treat symptoms, help in diagnosis
- 12. An endoscope
- 13. Indications of endoscopy of upper GI • Dysphagia • Odynophagia • Hematemesis or melena • Persistent heartburn/reflux • Dyspepsia unresponsive to treatment • Intractable vomiting • Foreign body ingestion
- 14. Uses of endoscopy 1. To investigate the cause of symptoms. 1. biopsy 2. To diagnose 3. To treat/intervene 1. FB removal 2. Stenting 3. Banding 4. Stricturotomy
- 15. Preparation for endoscopy I • In general, the patient should be stable, stabilize all unstable patients e.g. • Correct hypovolemia, electrolytes, anemia • Control bleeding in case there is • Stabilize vitals-BP, PR, RR, SPO2, RBS • Screen for communicable diseases-Hep B, Hep C, covid=? • Counsel the patient about the procedure, provide information, then • Consent • Inform theater • IV access • Prepare to monitor recovery
- 16. PREPARATION II • the patient to continue with normal diet till the day before the procedure. • If the procedure is scheduled in the morning (before 12pm), patient should stop eating/drinking at midnight. • If the procedure is in the afternoon (after 12pm, patient is allowed to eat solid foods till 8 hours before the procedure (5am). • Clear fluids are allowed up to 2 hours before the procedure. • Clear fluids include water, coffee, tea, soda. • The following are not clear fluids: alcohol, milk, juice with pulp, and liquid you cannot see through. • Patient should come with attendant/driver because the procedure involves sedation.
- 17. Additional tests done to add value to endoscopy • Depend on the findings during endoscopy and patient’s presentation. • Histology on biopsies taken • H.pylori Antigen test (on stool) • Urea breath test • Tumor markers
- 18. Complications/Risks of endoscopy • Can be minimized by properly preparing the patient and having the procedure done by skilled personnel • The risk of complication increases with any additional procedure/intervention done during endoscopy e.g. biopsy, stenting, releazing strictures, FB removal, etc, • Perforation. • Bleeding. • Infections (to and from the patient). • Cardiac arrest • Effects of drugs
- 19. Have learning objectives been achieved? • What are the structures in the upper GI? • Can you identify upper GI symptoms and signs among patients? • Some examples of chronic upper GI diseases • What are the uses/roles of endoscopy in patient management? • How do you prepare a patient for endoscopy? • Any complications? • Any additional tests you can do?
- 20. Video summary of endoscopy Upper Gastrointestinal Endoscopy Procedure - YouTube • Watch this YouTube video to give you a brief overview of endoscopy procedure • thanks
- 21. END
Notas do Editor
- Heavy consumption of carbonated drinks
- CA 72-4, CEA , CA19-9, AFP, Barium meal, barium swallow, barium follow through