Inflammation spring 2013 narrated(1)
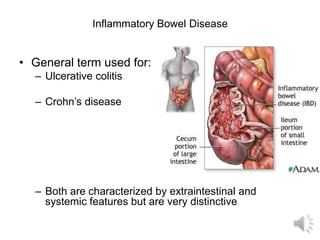
- 1. Inflammatory Bowel Disease • General term used for: – Ulcerative colitis – Crohn’s disease – Both are characterized by extraintestinal and systemic features but are very distinctive
- 2. Famous People with UC
- 3. Ulcerative Colitis • Area of chronic inflammation of mucosa and • submucosa in the rectum and spread to the • cecum that results in poor absorption of nutrients • Periods of exacerbations and remission • Can range in severity from mild to severe
- 8. Ulcerative Colitis • Manifestations – Colon becomes edematous and develops bleeding lesions & ulcers – Scar tissue develops and causes elasticity and loss of absorption • Diarrhea – Severe – Bloody • Vitamin K deficiency
- 9. • Weight loss • Anorexia • Malaise • Dehydration and electrolyte imbalances • Anemia • Abdominal tenderness and cramping
- 10. Mild Disease
- 11. Moderate
- 13. • May affect quality of life; patient may be fearful to leave house • Complications include: hemorrhage, abscess formation, malabsorption, bowel obstruction, bowel perforation, increased risk for colon cancer. • Diagnosed by colonoscopy; barium enema can show differences between UC and Crohn's
- 14. Ulcerative Colitis • Collaborative Management : – Medical management: • Rest is required to decrease intestinal activity • Diet therapy – Low-residue, high protein diet with vitamins and iron; in severe cases, nothing by mouth to rest the bowel; TPN will be ordered in severe cases – Avoid gas-forming foods, milk products, and foods with whole grains, nuts, alcohol, ETC
- 15. • Medications – • Aminosalicylates – deliver 5-ASA to the affected area– read these drugs! – Glucocorticoid – prednisone = given during an exacerbation to decrease the inflammation process of the bowel – – Immunomodulators – Antidiarrheals – Dangerous! Toxic Megacolon – New – Fecal bacterial transplantation therapy
- 17. Cont. Collaborative Care • Surgery – Total proctocoloctomy (removal of colon) with permanent ileostomy – is curative – Kock ileostomy – Ileoanal anastomosis with ileoanal resevoir – Review NUR 111 Elimination – for ostomy care! – Post op care • Encourage patient to talk about concerns related to disease process and its effect on lifestyle
- 19. Protocolectomy
- 20. Kock Surgery • Continent Ileostomy
- 21. Coping with flares • The above website will take you to a slide show on how to cope with UC flare ups.
- 22. Crohn’s disease • Chronic inflammation of GI mucosa occurring anywhere from mouth to anus but most common in terminal ileum • Characterized by exacerbations and remissions • Leads to thickening and scarring, a narrowed lumen, malabsorption • Lesions extend to all thickness of bowel wall and are prone to fistulas, ulcerations and abscesses • Lesions have a “cobblestone appearance” with sections of normal mucosa between lesions called “skip” lesions.
- 25. • Evidence is mounting that Crohn's disease is not an autoimmune disease, but an immune response to a bacteria - most likely candidate being "mycobacterium avium paratuberculosis
- 26. Crohn’s disease • Manifestations: vary patient to patient – common: – Diarrhea(5 to 6 liquid to semi formed stools/day) is most common symptom(usually without blood); steatorrhea (fatty stool) may occur – Abdominal pain n RLQ and distention – Low-grade fever • Others: – Weight loss – Malnutrition More that with UC – Fatigue, malaise – Dehydration – Complications
- 28. Crohn’s disease • Collaborative Management: – Diagnostic – see Ulcerative Colitis (UC) – Medical management: similar to UC • Diet: – Provide prescribed diet: usually high calorie, high protein; – Encourage intake of prescribed nutritional supplements – Daily weight, maintain calorie count, and monitor I and O – During severe exacerbations: NPO and TPN • Medications: – Same as UC with the following: » Budesonide (Entocort EC); metronidazole (Flagyl)
- 29. Crohn's disease Ulcerative colitis Defecation Often porridge-like[3], sometimes steatorrhea Often mucus-like and with blood[3] Tenesmus Less common[3] More common[3] Fever Common[3] Indicates severe disease[3] Fistulae Common[4] Seldom Weight loss Often More seldom Symptoms in Crohn's disease vs. ulcerative colitis [ v · d · e ]
- 30. Crohn’s disease • Surgical: – Avoided if possible; not curative, mostly just used to treat complications – Performed if not improved medically – Allow patient to express fears and anxiety about course of illness and possibility of surgical intervention
- 31. Nursing Diagnoses • Diarrhea related to inflammation of the bowel mucosa • Acute pain • Knowledge deficit • Imbalanced nutrition: Less than body requirements • Impaired skin integrity • Risk for FVD • PC: anemia • Differential Features of UC and Crohn’s Disease
- 32. Website for children and teens