WOUNDS.pptx
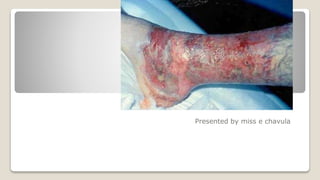
- 1. WOUND Presented by miss e chavula
- 2. GENERAL OBJECTIVES At the end of the lesson, students should gain knowledge on the management of patients with wounds.
- 3. SPECIFIC OBJECTIVES At the end of the lesson students should be able to; 1. define the term wound 2. state the classification of wounds 3. state the types of wounds 4. outline the process of wound healing 5. outline the classification of wound healing and factors affecting it 6. state wound management and complications of wound healing
- 4. INTRODUCTION A wound is a loss of continuity of the skin or mucous membrane which may involve soft tissues, muscles, bone and other anatomical structure. Any disruption to layers of the skin and underlying tissues due to multiple causes including trauma, surgery, or a specific disease state (Manley, Bellman, 2000).
- 5. TYPES OF WOUNDS Incisions or incised wounds, caused by a clean, sharp-edged object such as a knife, a razor or a glass splinter. Lacerations, Tissues torn apart, usually caused by irregular objects from accidents (e.g, machinery), results in swelling Contusion Blow from a blunt instrument Abrasions , superficial wounds in which the top most layer of the skin (the epidermis) is scraped off Punctured wounds, results in small opening in the skin, caused by an object puncturing the skin, such as a nail or needle or bullet
- 6. VARIOUS CLASSIFICATION OF WOUNDS Acute or chronic Open or closed Classified based on clinical appearance Penetrating or non-penetrating Based on contamination: Clean or contaminated
- 7. Classification by wound contamination Clean wounds: This category includes non- traumatic, uninfected wounds where no inflammation is encountered and no break in technique has occurred. Clean-contaminated: This category included non- traumatic wounds where a minor break in technique has occurred. No evidence of infection. Contaminated: Gross spillage has occurred or a fresh traumatic wound from a relatively clean source. Acute non-purulent inflammation may be evident. Dirty or infected : Old traumatic wounds from a dirty
- 8. Classification of wounds by depth Partial-thickness: Confined to the skin, the dermis and epidermis. Full-thickness : Involve the dermis, epidermis, subcutaneous tissue, and possibly muscle and bone
- 9. THE NORMAL PROCESS OF WOUND HEALING The inflammatory phase The regenerative (Proliferative) phase The Maturative (Remodeling) phase
- 10. THE INFLAMMATORY PHASE Initiated immediately after injury and lasts 3 to 4 days Two major processes:- - Homeostasis - Phagocytosis
- 11. THE INFLAMMATORY PHASE Hoemestasis is characterized by: Vasoconstriction of blood vessels in the affected area Deposistion of fibrin (connective tissue) Formation of blood clots. Increased blood supply to the area. Area appears reddened and oedematous
- 12. THE INFLAMMATORY PHASE Phagocytosis Macrophages( neutrophil) engulf micro Organisms and secrete angiogenesis factor which stimulate formation of new blood vessels.
- 13. THE REGENERATIVE PHASE Begins on the 2nd day of inflammation and last up to 24 days Signs of inflammation often reduces although the wound will often remain red in color. Here, the wound is usually covered by the skin cells( epithelial) cells.
- 14. THE MATURATIVE PHASE Begins about day 28 and can extend up to 6 months up to one or two years after the injury. Fibroblasts( a cell from which connective tissue form) continue to synthesize collagen( structural protein found in skin that is responsible for skin strength). In about the 3rd week, fibroblasts start to leave the wound, this reduces the scar but increases its strength. The scar become a thin and less elastic.
- 15. CLASSIFICATION OF WOUND HEALING (According to the amount of tissue loss) Primary intention healing Secondary intention healing Tertiary intention healing
- 16. CLASSIFICATION OF WOUND HEALING CONT.. PRIMARY INTENTION HEALING Occurs where the tissue surfaces have been closed and there is minimal or no tissue loss Characterized by the formation of minimal granulation tissue and scarring Example of such wound is a surgical incision SECONDARY INTETION HEALING Wound is extensive and involves considerable tissue loss Edges can not be approximated (closed). Here, the wound
- 17. CLASSIFICATION OF WOUND HEALING CONT.. TERTIARY INTENTIONAL HEALING Require more connective tissue. Occurs if a deep wound is not sutured early allowing more micro organisms to penetrate the wound. This leaves a deeper and wider scar. Example is an abdominal wound that is left open for drainage
- 18. FACTORS AFFECTING WOUND HEALING Age Wound healing tends to be faster in young people as compared to old people due to increased metabolism and circulation. Diabetes mellitus Provides good media for growth of bacteria thus delays wound healing Immune status Poor immune status of an individual can lead to poor wound healing Nutritional status Proteins and vitamin c are important nutrients needed for wound healing
- 19. FACTORS AFFECTING WOUND HEALING CONT.. Presence of infection Local infection delays wound healing. It increases the local tissue injury because infected wound will not heal until the infection is removed. Reduced blood supply to the wound Resting of the affected part Over activity of the affected part delays wound healing as this can disrupt wound closure Size of wounds
- 20. WOUND MANAGEMENT Surgical management of a wound whether elective or post- traumatic requires strict adherence to certain basic precepts if a successful outcome is to be expected, these include: History taking When-time What-circumstance Which-type of object causing injury Other associated factors
- 21. Physical Examination General condition: vitals Full physical examination recommended quick head to toe assessment is helpful local examination of site of wound Resuscitation very important- ABC, you can suture a wound but yet loose a patient Position, Suction, O2, IV fluids,
- 22. The patient must be stabilized Blood supply to the tissue must be adequate in order for the wound to heal. Analgesics to reduce pain Debridement: all necrotic tissue must be debrided as it provides an excellent medium for bacterial growth. (This is applicable to infected wounds). Wound irrigation with normal saline is necessary to remove foreign matter ,hematoma and decrease
- 23. Give tetanus prophylaxis Suturing: deep structures maybe repaired as appropriate to help restore function Time factor important: avoid suturing a wound which has occurred 6 hrs before presentation
- 24. Carry out aseptic wound dressing Antibiotics to kill bacteria Resting of the affected part so as to avoid disruption of wound healing Provide well balanced diet rich in proteins and vitamin c to promote wound healing
- 25. COMPLICATIONS OF WOUND HEALING Haemorrhage. May be due to dislodged clot or slipped ligature Hematoma- collection of blood under neath the skin Infection Dehiscence- partial or total rupturing of wound Evisceration – protrusion of internal viscera through an incision
- 26. REFERENCES 1. Black J and Hankinson J (2009) Medical Surgical Nursing, 8TH edition ,Mosby Elsevier 2. Lewis (2007) Medical Surgical Nursing, Assessment and Management of problems, 7TH edition ,Mosby Elsevier USA 3. Monahan et al (2007) Phipps Medical Surgical Nursing, 8TH edition Mosby Elsevier
- 27. THE END ZIKOMO