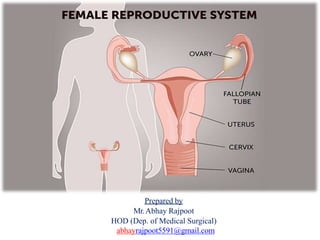
Female reproductive system
- 1. Prepared by Mr.Abhay Rajpoot HOD (Dep. of Medical Surgical) abhayrajpoot5591@gmail.com
- 4. The Female Reproductive System Functions Produces the female egg cells Transports the eggs to the site of fertilization The fertilization of an egg by a sperm, occurs in the fallopian tubes After fertilization, provides a place for a baby to develop If fertilization does not take place, the system is designed to menstruate Produces female sex hormones that maintain the reproductive cycle The female reproductive system consists of: A pair of ovaries along with A pair of oviducts, Uterus, Cervix, Vagina The external genitalia located in pelvic region.
- 5. The Female Reproductive System These parts of the system along with a pair of the mammary glands are integrated structurally and functionally to support the processes of ovulation, fertilization, pregnancy, birth and child care.
- 6. External Genitalia Collectively known as the vulva Labia majora Rounded folds of adipose tissue and skin Protect other external reproductive organs
- 7. Labia minora Fold of skin between labia majora Very vascular Merge to form hood over clitoris Vestibule – space enclosed by labia minora Bartholin’s glands secrete mucus during sexual arousal Clitoris Anterior to urethral meatus Contains female erectile tissue Rich in sensory nerves Perineum Between vagina and anus Area for episiotomy, if needed, during birth process
- 8. Hymen The hymen is a thin layer of mucus membrane that [partially blocks the opening of the vagina. Its normally incomplete to allow for passage of menstrual flow. Vestibule Gland It is the space between the labia minora. Its floor contain the greater vestibular gland or Bartholin glands one on each side of vaginal opening. During sexual excitement vestibular gland secreta alkaline mucus that provides some lubrication and also reduce some of the natural acidity of vagina.
- 10. Vagina Canal that joins the cervix (the lower part of uterus) to the outside of the body Also is known as the birth canal Passageway for sperm and menstrual flow Capable of considerable distention (stretching) Contains large stores of glycogen which decomposes to organic acids – lower pH = less susceptible to infection & less hospitable to sperm.
- 11. The Uterus An organ about the size and shape of an inverted pear. Its weight is from 30 to 40 grams Functions in menstruation, implantation of zygote, development of the fetus, and labor. Also part of the pathway for sperm to reach ovum. Uterus can be divided into: Fundus – domed upper portion Body – main portion Cervix – narrow, lower section extending into vagina (cervical orifice)
- 13. The Uterus Layers of uterus: Perimetrium a part of visceral peritoneum Myometrium Bulk of uterus Three layers of muscle that contract under influence of oxytocin during labor. Endometrium – Highly vascular mucosa Stratum functionalis – Shed during menstruation Stratum basalis – Deeper, permanent layer, gives rise to new stratum functionalis after each cycle.
- 14. Uterine (Fallopian) Tubes Narrow tubes that are attached to the upper part of the uterus and serve as tunnels for the egg cell to travel from the ovaries to the uterus. Fertilization of an egg by a sperm, normally occurs in the fallopian tubes. The fertilized egg then moves to the uterus, where it implants into the lining of the uterine wall . Fertilization can occur up to about 24 hours after ovulation. If oocyte is fertilized, it will reach the uterus in about 7 days. Uterine Tube & Ciliated cells
- 15. Ovaries Ovaries are the primary female sex organs that produce the female gamete (ovum) and several steroid hormones (ovarian hormones). Oval-shaped glands that are located on either side of the uterus. The ovaries are located one on each side of the lower abdomen. Each ovary is about 2 to 4 cm in length and is connected to the pelvic wall and uterus by ligaments. Location of Ovaries
- 16. Each ovary has a hilus – blood vessels and nerves enter Several layers: Germinal epithelium – simple squalors cells Tunica albuginea- white capsule of C. T. Stroma – connective tissue, can be divided into: Medulla – loose connective tissue, blood vessels, nerves Cortex - contains ovarian follicles – consist of oocytes at various stages of development Single layer – follicular cells Several layers – granulosa cells Mature or Graafian follicle is a large, fluid-filled follicle that will rupture and release a secondary oocyte in process called ovulation. Corpus luteum is the remnant of a ruptured follicle – produces estrogen, progesterone and relaxin until degenerates into the corpus albicans.
- 17. Ovary
- 18. Oogenesis During fetal development, germ cells differentiate into oogonia millions of germ cells. Many degenerate, but a few develop into primary oocytes that enter Prophase I of meiosis before birth – stop there. At birth, about 1 million oogonia and primary oocytes in each ovary. About 400 mature over a woman’s lifetime. Primordial follicle – primary oocyte and single layer of follicular cells Layer of glycoprotein, the zona pellucida, separates oocyte from the granulosa cells. Ovarian cells outside follicle form two layers: Inner vascular layer (theca interna) that secretes hormones Outer fibrous layer (theca externa) – connective tissue. Granulosa cells begin to secrete fluid, forms a cavity called the antrum. After puberty, each month one secondary follicle resumes meiosis. Meiosis I results in two unequal cells – secondary oocyte and a polar body. Begins to divide again but stops at metaphase II.
- 19. Oogenesis z
- 20. Oogenesis At ovulation, secondary oocyte and polar body are released. If not fertilized, degenerates. If penetrated by sperm, meiosis resumes, forming ovum and another polar body. Nuclei of ovum and sperm unite to form a zygote. (2n or diploid). So, meiosis results in ONE OVUM and three polar bodies (which degenerate).
- 21. Reproductive Cycle Menstrual cycle Regular changes in uterine lining, resulting in monthly bleeding Menarche First menstrual period Menopause Termination of cycle due to normal aging of ovaries Phases of the Female Reproductive Cycle Type cycle runs 24 -35 days, 28 days ave. Three phases: Menstrual phase Preovulatory phase Postovulatory phase
- 22. Menstrual phase Days 1 – 5 FSH release stimulates the maturation of follicles. 20 or so follicles, some in each ovary begin to enlarge. In the uterus, the stratum functionalis is shed, discharging 50 -150 ml of blood, tissue fluid, mucus and epithelial cells. Declines of estrogen and progesterone cause the spiral arteries to constrict, cells become ischemic and die, and are sloughed off.
- 23. Preovulatory phase Most variable in length, us. Day 6 – 13 Follicles continue to grow, granulosa cells produce increasing amounts of estrogen and some progesterone. This causes LH to be secreted, but stored in the pituitary. Dominant follicle secretes inhibin, inhibiting growth of other follicles, and continues to develop into a mature follicle. Called follicular phase in ovary. In the uterus, the estrogens produced by the developing follicles cause the cells of the stratum basalis to produce a new stratum functionalis, and thickness of endometrial doubles. Proliferative phase in uterus.
- 24. Postovulatory phase Postovulatory phase most constant in duration at 14 days, days 15 – 28. In ovaries called the luteal phase. If fertilization does not occur, at end of two weeks the secretions of corpus luteum decline, and it degenerates into corpus albicans (white body) In the uterus, progesterone promotes : growth of endometrial glands which secrete glycogen Vacularization of stratum functionalis Increase in amount of tissue fluid These changes reach a peak about one week after ovulation, about the time the fertilized ovum would arrive. Called secretory phase in uterus
- 26. Breast The breast lies over the pectoral muscles. Estrogen and progesterone hormones released by ovaries, control the breast development, progesterone Stimulates the secretory cell and estrogen stimulates the growth of the ducts. Structure of the breast: Each breast consist of several lobules. In which secreting cell are present. Adipose tissue is deposited around the surface of the gland, just under the skin between the lobes. The lobules join to form ducts called lactiferous ducts. There are 15 to 20 Ducts
- 29. Mammary glands Accessory organs of the female reproductive system Modified sweat glands Function is to synthesize, secrete and eject milk (lactation) Lie over the pectoralis major muscles Are attached to fascia by the suspensory ligaments (of Cooper) Breast size is determined more by fat than by glandular tissue. Each breast has 15 – 20 lobes made up of several lobules. Lobules are made of milk-secreting cells arranged in alveoli. Alveoli are surrounded by myoepithelial cells which contract to move milk out of alveoli. Milk passes from alveoli to secondary tubules into mammary ducts.
