Ngai Language Barrier in Disaster Planning
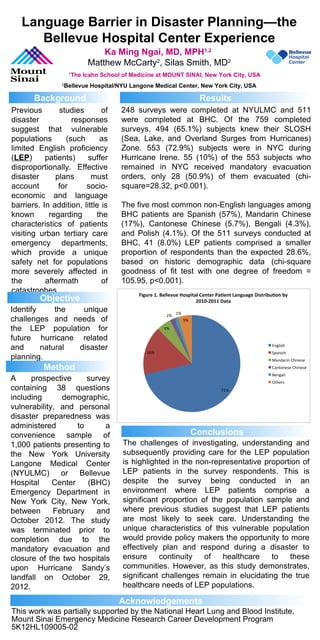
- 1. Language Barrier in Disaster Planning—the Bellevue Hospital Center Experience Ka Ming Ngai, MD, MPH1,2 Matthew McCarty2 , Silas Smith, MD2 Sch1 The Icahn School of Medicine at MOUNT SINAI, New York City, USA 2 Bellevue Hospital/NYU Langone Medical Center, New York City, USA This work was partially supported by the National Heart Lung and Blood Institute, Mount Sinai Emergency Medicine Research Career Development Program 5K12HL109005-02 Previous studies of disaster responses suggest that vulnerable populations (such as limited English proficiency (LEP) patients) suffer disproportionally. Effective disaster plans must account for socio- economic and language barriers. In addition, little is known regarding the characteristics of patients visiting urban tertiary care emergency departments, which provide a unique safety net for populations more severely affected in the aftermath of catastrophes. Identify the unique challenges and needs of the LEP population for future hurricane related and natural disaster planning. A prospective survey containing 38 questions including demographic, vulnerability, and personal disaster preparedness was administered to a convenience sample of 1,000 patients presenting to the New York University Langone Medical Center (NYULMC) or Bellevue Hospital Center (BHC) Emergency Department in New York City, New York, between February and October 2012. The study was terminated prior to completion due to the mandatory evacuation and closure of the two hospitals upon Hurricane Sandy’s landfall on October 29, 2012. 248 surveys were completed at NYULMC and 511 were completed at BHC. Of the 759 completed surveys, 494 (65.1%) subjects knew their SLOSH (Sea, Lake, and Overland Surges from Hurricanes) Zone. 553 (72.9%) subjects were in NYC during Hurricane Irene. 55 (10%) of the 553 subjects who remained in NYC received mandatory evacuation orders, only 28 (50.9%) of them evacuated (chi- square=28.32, p<0.001). The five most common non-English languages among BHC patients are Spanish (57%), Mandarin Chinese (17%), Cantonese Chinese (5.7%), Bengali (4.3%), and Polish (4.1%). Of the 511 surveys conducted at BHC, 41 (8.0%) LEP patients comprised a smaller proportion of respondents than the expected 28.6%, based on historic demographic data (chi-square goodness of fit test with one degree of freedom = 105.95, p<0.001). The challenges of investigating, understanding and subsequently providing care for the LEP population is highlighted in the non-representative proportion of LEP patients in the survey respondents. This is despite the survey being conducted in an environment where LEP patients comprise a significant proportion of the population sample and where previous studies suggest that LEP patients are most likely to seek care. Understanding the unique characteristics of this vulnerable population would provide policy makers the opportunity to more effectively plan and respond during a disaster to ensure continuity of healthcare to these communities. However, as this study demonstrates, significant challenges remain in elucidating the true healthcare needs of LEP populations. Background Objective Method Results Acknowledgements Conclusions
