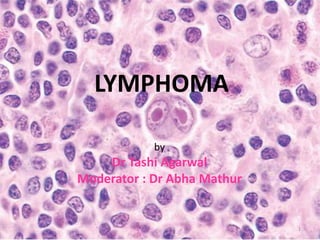
Hodgkin lymphoma
- 1. LYMPHOMA by Dr Tashi Agarwal Moderator : Dr Abha Mathur 1
- 2. Hematopoietic Malignancies Lymphoma is a general term used for proliferations that arise as discrete tissue masses. Leukemia is used for neoplasms that present with widespread involvement of the bone marrow and the peripheral blood(usually). 2
- 3. What is Lymphoma Malignant lymphoma is a term given to tumors of the lymphoid system and specifically of lymphocytes and their precursor cells i.e. Cancer of the lymphatic system. • Many lymphomas are known to be due to specific genetic mutations. 3
- 4. Malignant lymphoma Hodgkin lymphoma Non Hodgkin lymphoma 4
- 5. Hodgkin disease Hodgkin lymphoma Type of malignant lymphoma in which Reed-Sternberg cells are present in a characterstic background of reactive inflammatory cells of various types, accompanied by fibrosis of variable degree. ( except NLPHL) 5
- 7. Introduction • Are group of cancers which originate from lymphatic systems. • It was named after Thomas Hodgkin who first described it in 1832. • Dorothy Reed and Carl Sternberg first described the malignant cells of Hodgkin lymphoma call Reed Sternberg cells. • Hodgkin lymphoma was the first cancer which could be successfully treated by radiation therapy and also by combination chemotherapy. 7
- 9. Risk Factors • No clear risk factors, several implicated • EBV (pathogen or passenger) • HIV • woodworking, farming • rare familial aggregations • First degree relatives have five fold increase in risk for Hodgkin lymphoma. • Associated with EBV infection mainly with mixed cellularity type. • High socio economic status. • Prolonged use of of human growth hormone. • men > women • whites > blacks > Asians 9
- 10. Natural history • Hodgkin lymphoma arises in a single node or chain of nodes and spreads first to anatomically contiguous lymphoid tissue. • Visceral involvement by hodgkin lymphoma may be secondary to extension from adjacent lymph nodes. • Hematogenous spread occurs to liver or multiple bony sites. • Mechanism of spleen involvement is unclear but all patients with hepatic and bone involvement are associated with splenic involvement. 10
- 11. Clinical features • Most common presentation is asymptomatic lymphnode enlargement, typically in the neck. • Cervical lymphnodes are involved in 80% cases. • Mediastinal involvement is seen in about 50% cases. They produce symptoms like chest pain, cough and dyspnoea. • Infradiaphrgamatic involvement is seen in 5% cases and usually seen with older patients. • Other less common symptoms are : Pruritis, alcohol induced pain over involved lymphnodes, nephrotic syndrome, erythema nodosum, cerebellar degeneration, immune hemolytic anaemia, thrombocytopenia, hypercalcemia. 11
- 12. B symptoms • About 33 % present with B symptoms overall • Only 15-20% of stage I-III have B symptoms like 1. Fever(>38^C) • May first present as fever of unknown origin • Fever persists for days to weeks followed by afebrile intervals and then recurrence. • This pattern is called Pel Ebstein fever. 2. Drenching night sweats 3. Weight loss (>10% in 6 months) 12
- 13. 13
- 15. 15
- 17. PET SCAN 17
- 18. Relative frequencies of different lymphomas Hodgkin lymphoma NHL Diffuse large B-cell Follicular Other NHL Non-Hodgkin Lymphomas ~85% of NHL are B-lineage 18
- 19. Hodgkin lymphoma • Cell of origin: Germinal centre B-cell • Reed-Sternberg cells (or RS variants) in the affected tissues. • Most cells in affected lymph node are polyclonal reactive lymphoid cells, not neoplastic cells. 19
- 20. JACKSON AND PARKER (1947) SMETANA AND COHEN’S ADDITION (1956) LUKES (1963) PARAGRANULOMA PARAGRANULOMA LYMPHOCYTIC AND HISTIOCYTIC, NODULAR LYMPHOCYTIC AND HISTIOCYTIC, DIFFUSE GRANULOMA GRANULOMA NODULAR SCLEROSIS MIXED CELLULARITY NODULAR SCLEROSIS SARCOMA SARCOMA DIFFUSE FIBROSIS RETICULAR Early Classifications 20
- 21. Later Classifications • The Lukes-Butler classification of HL, modified at the Rye Conference in 1966, described the criteria for the four familiar subtypes of HL: lymphocyte-predominant, nodular sclerosing, mixed cellularity, and lymphocyte-depleted. • The REAL classification separated the nodular lymphocyte-predominant (NLP) subtype from so-called classic HL based on the immunophenotypic and genotypic differences • The REAL classification of HL was carried forward to the 2001 WHO classification of HL and the 2008 WHO classification. 21
- 22. 2008 WHO Classification of Hodgkin Lymphoma 22
- 23. Reed Sternberg cell Common feature of ALL Hodgkin Lymphomas. • Large cells ( >45um in diameter) with classically binucleate or bilobed central nucleus each with a large acidophilic central nucleoli surrounded by a clear halo. “owl’s eye appearance” • Variants: mononuclear (Hodgkin’s cell), mummified cell, lacunar cell, L/H cell. • Requirement of Reed-Sternberg cell for initial diagnosis is “absolute”(less strict for LPHL or recurrent disease) • Classic Reed-Sternberg cell: + CD15, CD30, CD25 – CD45, pan-B, S-100, keratin, EMA • Most current studies indicate the RS cells of HL are lymphocytic in nature and, in the great majority of cases, are of B-cell origin. 23
- 25. lacunar cell (mixed cellularity) (nodular sclerosis) (lymphocyte predominance) RS Cell variants 25
- 26. Lymph node, nodular-sclerosing Hodgkin lymphoma. (A) Clusters of Reed-Sternberg cells and variants react with anti-CD15. (B) Reed-Sternberg cells in the same case show negative results for CD45 (leukocyte common antigen), in contrast to positive surrounding small lymphocytes. A B 26
- 27. A possible model of pathogenesis germinal centre B cell transforming event(s) loss of apoptosis RS cell inflammatory response EBV? cytokines 27
- 28. Cytokines (such as IL-5, IL-10, IL-13, and TGF-β) and chemokines (such as TARC, MDC, IP-10, and CCL28) are secreted by Reed- Sternberg cells. They lead to florid accumulation of reactive cells in tissues involved by classical HL. These reactive cells produce factors that support the growth and survival of the tumor cells and further modify the reactive cell response. 28
- 30. Lymphocyte predominant Hodgkin lymphoma • <5% of Hodgkin lymphoma • Mainly involves cervical, axillary or mediastinal • L&H cells or Popcorn cells are seen • Positive for CD20, 45, CD79a, Bcl-6, J-chain, and PAX-5. EMA positive in 50% cases. • Negative for CD15, 30. • Differential Diagnosis: Well differentiated lymphocytic lymphoma, mononucleosis, malignant melanoma,, progressive transformation of germinal centers 30
- 31. • LPHL is divided into two histopathologic subtypes: 1. Lymphocytic and histiocytic (L&H) nodular 2. L&H diffuse • Currently the WHO classification recognizes only the nodular type and requires at least a partially nodular growth pattern for diagnosis . Whether the diffuse type is a distinct entity is controversial. • Small lymphocytes predominate in the reactive component in both types and are intermixed with varying numbers of histiocytes. Eosinophils, neutrophils, and “diagnostic” or “classic” RS cells are rare. In fact, the diagnosis of LPHL is doubtful if diagnostic RS cells are found easily; the number of such cells should be fewer than one per histologic section. 31
- 32. • In LPHL, L&H variants of RS cells are conspicuous with folded, multilobed nucleus and smaller nucleoli(“popcorn nuclei”). • In the nodular subtype of LPHL, there is almost total obliteration of the nodal architecture by a vaguely nodular process. LPHL nodules are composed of small, round lymphocytes with varying numbers of epithelioid histiocytes which gives them a mottled appearance. L&H variants of RS cells may be numerous and are principally seen in the nodules. • “Diagnostic” or “classic” RS cells are rare or nonexistent and are not required for the diagnosis of NLPHL. 32
- 33. • Hodgkin lymphoma, lymphocyte predominance type. Numerous mature- looking lymphocytes surround scattered, large, pale-staining lymphohistiocytic variants (“popcorn” cells). 33
- 34. • An attenuated rim of residual normal node (top) is often present in nodular NLPHL. The vaguely nodular growth pattern and compressed adjacent normal node seen at low magnification are features highly suggestive of Nodular NLPHL. 34
- 36. 1. Nodular Sclerosis • Most common type diagnosed • About 70% • Lacunar cells seen • CD15, 30 positive • EBV negative • Only subtype without a male predominance • Seen in younger patients with stage I-II disease. • Differential diagnosis: Large cell Non Hodgkin lymphoma, carcinoma, germ cell tumour and thymoma. 36
- 37. The classic histopathologic criteria for NSHL are (a) prominent nodularity (b) presence of lacunar RS cell variants, and (c) birefringent broad collagen bands • Nodal architecture is obliterated by relatively large nodules of tumor partly or totally encircled by dense connective tissue bands that are birefringent when viewed under polarized light. 37
- 38. LACUNAR VARIANT RS CELL : These variants possess large, multilobated, or irregular nuclei with finely dispersed chromatin; nucleoli are usually small. The cytoplasm of lacunar cells retracts when fixed in formalin, so the nuclei gives the appearance of cells that lie with empty spaces between them. (lacunae) This retraction in absent in tissues fixed in Zenker and B5. 38
- 39. • Hodgkin lymphoma, nodular sclerosis type. A low-power view shows well- defined bands of pink, acellular collagen that subdivide the tumor into nodules 39
- 40. 2. Mixed Cellularity • Constitutes about 20% • More than 50% present as stage III or IV disease • Biphasic incidence, peaking in young adults and again in adults older than 55 • CD15, 30, EBV positive • Presents in advanced stages • Tendency to involve spleen, bone marrow. • Differential diagnosis: Some cases of MCHL display an interfollicular growth pattern. Such cases may be difficult to distinguish from peripheral T-cell lymphomas. Lennert’s lymphoma (diffuse mixed T-cell ML with excessive histiocytes). Diffuse follicular lymphoma. 40
- 41. Lymph node, mixed-cellularity Hodgkin lymphoma disease. Diagnostic Reed- Sternberg cells are usually found without difficulty in mixed-cellularity Hodgkin lymphoma. The reactive component consists of small, round lymphocytes, histiocytes, plasma cells, and eosinophils, 41
- 42. 3. Lymphocyte Depleted • Constitutes <5% • Worst prognosis of all subtypes • Older males, rare in children • Present as febrile illness with pancytopenia, hepatomegaly, and no peripheral lymphadenopathy • Advanced stage, Stage IV • The biologic hallmark of LDHL is a collapse of cell-mediated immunity, HIV infection • RS cells CD15+, CD30+; most EBV+ • Differential Diagnosis: Large cell Non- Hodgkin’s lymphoma. Nodular sclerosis HL 42
- 43. • Two subtypes of LDHL—diffuse fibrosis and reticular. The WHO classification does not subdivide the LDHL. Although the morphologic appearance of LDHL is varied, a unifying feature is the relative predominance of RS cells compared with the depletion of background lymphocytes. • In some cases there is a diffuse fibrosis background. Sections show a hypocellular background and abundant disorderly connective tissue admixed with a PAS-positive fibrinoid material that is not birefringent. Nodal architecture is completely obliterated. RS cells may be rare and difficult to identify. multiple sections may be required to find RS cells. • Other cases of LDHL have little in the way of a reactive component but are distinguished by the presence of numerous large RS cells with bizarre cytologic features. The sheetlike growth of bizarre RS cells is responsible for the older term Hodgkin sarcoma. 43
- 44. 4. Lymphocyte-Rich • RS cells CD15+, CD30+; 40% EBV+ • Uncommon • M > F • Tends to be seen in older adults • This is an uncommon form of classical HL • Reactive lymphocytes make up the vast majority of the cellular infiltrate. In most cases, involved lymph nodes are diffusely effaced, but vague nodularity due to the presence of residual B-cell follicles is sometimes seen. • Differential Diagnosis: This entity is distinguished from the lymphocyte predominance type by the presence of frequent mononuclear variants and diagnostic Reed-Sternberg cells with a “classical” immunophenotypic profile. • Very good to excellent prognosis. 44
- 45. Frequent mononuclear and diagnostic RS cells; background infiltrate rich in lymphocytes. 45
- 46. 46
- 47. Spread • Generally a well behaved spread of disease through contiguous LN groups, (especially NS and LP); <5% show non-contiguous spread • May have direct extension into perinodal tissue. • 85% of Stage I/II disease are above diaphragm. • Spleen: if >400g, almost always positive. • Liver: if positive, spleen and retroperitoneal LN’s are also positive. 47
- 48. Ann Arbor Staging System • Stage I: Single lymph node region (I) or single extralymphatic organ or site (IE) • Stage II: > 2 lymph node regions on same side of diaphragm (II) or with limited, contiguous extra lymphatic tissue involvement (IIE) • Stage III: both sides of diaphragm involved, may include spleen (IIIS) or local tissue involvement (IIIE) • Stage IV: multiple/disseminated foci involved with > 1 extralymphatic organs (i.e. bone marrow) (A) or (B) designates absence/presence of “B” symptoms *(E) Localized, solitary involvement of extralymphatic tissue, excluding liver and bone marrow 48
- 49. 49
- 50. Stage I Stage II Stage III Stage IV Staging of lymphoma A: absence of B symptoms B: fever, night sweats, weight loss 50
- 51. PROGNOSIS • Clinical stage • Extranodal involvement bad (especially if distant rather than by direct spread) • Degree of splenic involvement: ≥5 nodules poor prognosis • Age: >50 yrs unfavorable • Sex and race: Black males worse than white females • Microscopic type: LP and NS best, MC intermediate, LD worst (less important with current treatment protocols) • Laboratory findings: decreased hematocrit, elevated LDH, raised ESR, elevated serum levels of CD30, soluble CD25 have negative prognosis. • CD15- lack of expression is a negative prognostic factor. 51
- 52. 52
- 53. Chemotherapy Regimen Medication Regimen Medication 1. ABVD (US) •ADRIAMYCIN •BLEOMYCIN •VINBLASTINE •DACARBAZINE 2. STANFORD V (NEW) •ADRIAMYCIN •BLEOMYCIN •VINBLASTINE •VINCRISTINE •PREDNISONE •MECHLORETHAMINE ETOPOSIDE 3. MOPP •Mechlorethamine • Vincristine •Procarbazine • Prednisone 4. BEACOPP (EUROPE) •BLEOMYCIN •ETOPOSIDE •ADRIAMYCIN •CYCLOPHOSPHAMIDE •ONCOVIN •PROCARBAZINE •PREDNISONE 53
- 54. Radiotherapy • Radiation therapy is the most effective single thrapeutic agent for treating Hodgkin lymphoma. • The main objective of radiation in Hodgkin lymphoma is to treat involved and contiguous field. • Radiotherapy can be given by 1. 2D planning 2. 3D planning 3. IFRT • Involved field radiotherapy is the most commonly used technique at present. It targets a smaller area rather than a classical extended field. 54
- 55. Complications • Autologous bone marrow transplantation can cure half of patients who fail effective chemotherapy regimens. • Because of the very high cure rate in patients with Hodgkin's disease, long-term complications have become a major focus for clinical research. The most serious late side effects include secondary malignancies, cardiac injury, infertility and Lhermitte's syndrome. 55
- 56. LYMPHOMA 56