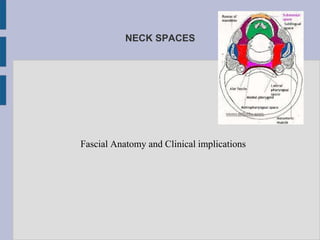
Deep Neck Spaces
- 1. NECK SPACES Fascial Anatomy and Clinical implications
- 2. contents ●Introduction ●Definition ●Classification ●Description of Fascia ●Spaces ●Pathways of spread ●Pathological organisms ●Management principles ●Conclusion
- 3. Introduction ●The infection in orofacial region does not spread haphazardly through the loose connective tissue, but tends to accumulate in the potential spaces around the head and neck ●Many of these spaces communicate with each other ●Knowledge of the spaces and potential area of communication assist with not only the management but also assist us with potential spread points
- 4. DEFINITATIONS: ●FASCIA: defined as a broad sheet of dense connective tissue, whose function is to separate structure that must pass over each other during movement such as muscles and glands and also serve as pathway for course of vascular and neural structures ●Shapiro defined facial spaces as “potential spaces between the layers of fascia” ●These areas are normally filled with loose connective tissue which readily breaks down when invaded by infection
- 5. Classifications: ● Grodinsky and Holyoke in 1938 ● Space 1 – the potential space superficial and deep to platysma muscle ● Space 2. - the space behind the anterior laryer of deep cervical fascia ● Space 3 – pretracheal space lies anterior to trachea ● Space 3a – lincoln”s highway ● Space 4 – danger space, potential space between the alar and prevertebral fascia
- 6. Based on Clinical significance ● Face: - buccal, canine, masticatory and parotid ● Suprahyoid: - sublingual, submandicular, lateral pharyngeal and peritonsillar ● Infrahyoid: - pretracheal ● Spaces of total neck :- retropharyngeal, parapharyngeal and space of carotid sheath
- 7. Based on mode of involvement ● Direct involvement Primary spaces : maxillary space Mandibular spaces ● Indirect imvolvement: secondary spaces
- 8. FASCIA DESCRIBED UNDER: ●SUPERFICIAL CERVICAL FASCIA Thin layer of connective tissue that lies between dermis of the skin and investing layer of deep cervical fascia Contains cutaneous nerves, blood and lymphatic vessels, superficial lymph nodes and variable amount of fat Anteriolaterally it contains the platysma
- 9. VISCERAL LAYER ● Middle layer Muscular division – surrounds the infrahyoid strap muscles Visceral division envelops the pharynx, larynx, oesophagus, trachea and the thyroid gland Passes inferiorly into the upper mediastinum where it is continious with the fibrous pericardium and covers the trachea and oesophagus Above hyoid this layer continues on the posterior pharyngeal wall as the buccopharyngeal fascia Primary surgical significance of this layer is it must be divided in midline in a surgical approach to trachea or thyroid gland
- 10. DEEP LAYER ● Originates from the spinous processes of the cervical vertebra and ligamentum nuchae ● At the transverse process of the cervical vertebra, it divides into an anterior alar layer and posterior prevertebral layer ● Alar fascia extends from base of skull to the second thoracic vertebra ● Prevertebral fascia lies just anterior to the vertebral bodies and extends the entire length of vertebral column
- 11. FASCIA ●Deep cervical fascia consists of FOUR fascial layers ●Investing or superficial or anterior layer ●Pretracheal or middle layer ●Prevertebral or posterior layer ●Carotid sheath ●These layers support the viscera, muscles, vessels and deep lymph nodes ●Provide the slipperiness that allows the structures in the neck to move and pass over one another without difficulty (e.g. when turning the head and swallowing) ●Layers form natural cleavage planes, allowing seperation of tissues during surgery
- 12. Investing layer Superficial layer of deep cervical layer ●Follows the “rule of Twos” Envelops two muscles, two glands and forms two spaces Originates from the spinous porcess of the vertebral column and spreads circumferentially around the neck Covers the sternocleidomastoid and trapezius muscles Encloses submandibular and parotid glands Covers anterior bellies of the digastric and the mylohyoid – forms floor of submandibular space
- 13. Investing layer ● Forms the space of the posterior triangle ● and the suprasternal space of burns in the midline
- 14. Middle layer ● Surrounds the infrahyoid strap muscles, thyroid, larynx, trachea and oesophagus ● Below hyoid this layer continues inferiorly to fuse with pericardium ● Above hyoid this layer continues on the posterior pharyngeal wall as the buccopharyngeal fascia
- 15. Deep (Prevertebral Fascia) ● Surrounds the prevertebral muscle ● Anteriorly it divides to form a thin alar layer and a thicker prevertebral layer ● Between these two layer is the “danger space” extending from skull base to the diaphragm
- 16. Carotid sheath ● Carotid sheath is a fascial layer that is associated with but is anatomically separate from cervical fascial layers ● It receives contributions from all three layers of deep cervical fascia ● Contains carotid artery, internal jugular vein, vagus nerve and deep lymphatic chains ● It continues from the skull base through the neck along the anterior surface of the prevertebral fascia and enters the chest behind the clavicle
- 17. VISCERAL VASCULAR SPACE ● Potential space within the carotid sheath ● Contain little areolar tissue and is resistant to sperad of infections ● Aka “lincoln's Highway” ● Extends from base of skull into the mediastimum ● Receives contributions from all three layes of deep fascia ● Can become secondarily involved by infection in any other deep neck space by direct spread
- 18. SPACES SPANNING THE ENTIRE LENGTH OF NECK ● The superficial space is located between the superficial fascia and the superficial layer of deep fascia. ● This potential space lies superficial and deep to the platysma and contains loose areolar tissue, lymph nodes, nerves and vessels – most significant of which is the external jugular vein ● This space is most commonly involved with superficial cellulitis of the neck, but if abscess formation does occur, it will present with obvious fluctuance and typical signs of infections
- 19. DEEP NECK SPACES ● Retropharyngeal space ● Danger space ● Prevertebral space ● Visceral Vascular space
- 20. RETROPHARYNGEAL SPACE ● LARGEST and most clinically interfascial space in the neck because it is major pathway for spread of infection. ● Potential space consists of loose connective tissue between visceral part of prevertebral layer of deep cervical fascia and the buccopharyngeal fascia ● Occupies space posterior to the pharynx and oesophagus ● Anterior wall- buccopharyngeal fascia superiorly and the visceral division of the middle fascial inferiorly ● Posterior wall is the alar layer of the deep fascia ● Lateral boundry is the carotid sheath ● Space extends from the base of skull to T1 T2 vetebra
- 21. DANGER SPACE ● Posterior to the retropharyngeal space ● Space between the alar layer and prevertebral layer of deep fascia ● So named because it contains loose areolar tissue and ● offers little resistance to spread of infection ● Runs from the skull base to diaphragm
- 22. SUPRA HYOID SPACES ● Submandibular space ● Parapharyngeal space ● Peritonisllar space ● Masticator space ● Partoid space
- 23. SUBMANDIBULAR SPACE ● Bounded by the mandible anteriorly and laterally ● Lingual mucosa superiorly ● Hyoid postero- inferiorly ● Superficial layer of deep cervical fascia inferiorly
- 24. ● Mylohyoid muscle divides space into a superior sublingual space and submylohyoid space ● Sublingual space contains loose areolar tissue, the hypoglossa and lingual nerves, the sublingual gland and wharton's duct ● Submylohyoid space contains the anterior bellies of the digastric and submandibular glands ● These two subdivisions freely communicate around the posterior border of the mylyhyoid
- 25. PARAPHARYNGEAL SPACE ● Skull base superiorly ● Pterygo mandibular raphe anteriorly ● Hyoid bone inferiorly ● Bucopharyngeal fascia medially
- 26. PERITONSILLAR SPACE ● Medial – capsule of palatine tonsil ● Lateral – superior pharyngeal cronstrictor ● Superior – anterior tonsillar pillar ● Inferior – posterior tonsillar pillar ● Contains loose areolar tissue adjacent to soft palate
- 27. Masticator space ● Collective name for submasseteric, pterygomandibular, superficial and deep temporal spaces ● Muscles of mastication are enclosed by investing layer of fascia ● Contains mandibular division of trigeminal and internal maxillary artery
- 28. Parotid space ● Formed by superficial layer of deep fascia and dense septa from capsule into gland ● Contents: parotid lymph nodes, facial nerve and posterior facial vein ● Fascial envelope is deficient on the supero- medial surface of the gland thus direct communication btwn this space and PPS
- 29. Direction of spread ● Tonsillitis – peritonsillar abscess ● Spread to lateral pharyngeal space ● To posterior pharyngeal and prevertebral spaces and chest ● Mediastinitis and empyema PPSParotid space Masticator space Submandibular space Retropharyngeal space
- 30. Retropharyngeal abscess in children ● Most common deep neck abscess ● Retropharyngeal lymph nodes tend to involute with age ● Source of infections suppurative process in the nose, nasopharynx, sinus and adenoids ● 96% of abscesses occur prior to 6 years of age
- 31. Common symptoms ● Fever ● Irritability ● Torticollis ● Trismus ● Cervical lymphadenopathy ● Posterior pharyngeal bulge ● Children often have poor oral intake due to sore throat initially ● Followed by dysphagia and drooling ● Finally if not treated may get laryngeal oedema and respiratory distress
- 32. RA IN ADULTS ● Typically caused by: Penetrating or blunt trauma Instrumentation such as endoscopy Intubation or NG placement Extension of infection from an adjoining deep neck space Historically, the most common cause of prevertebral abscess was the extension of a tuberculous infection of a vertebral body (pott's absces)
- 33. PARAPHARYNGEAL SPACE ABSCESS ● Infection in the pharynx, tonsils, adenoids, teeth, parotid or lymph node chains ● Middle ear infections or mastoiditis ● Extension of infection from the nearby: Peritonsillar space submandibular space retropharyngeal space Masticator space
- 34. Signs and symptoms ● Differ depending on whether the prestyloid or poststyloid compartment is involved ● In addition to fever, chills and malaise, anterior infection often causes pain, dysphagia and significant trismus due to medial pterygoid irritation ● Oedema in this area will cause medial bulging of the lateral pharyngeal wall and the tonsils and there will be swelling at the angle of mandible
- 35. ● Posterior compartment infection may have no localizing signs on examination ● Despite this patients do appear toxic “PUO” ● Involvement of neurovascular structures in this area may lead to neuropathies, horner's syndrome, septic internal jugular thrombosis or carotid artery rupture
- 36. ● In recent years, submandibular space abscess has become the most common deep neck space infection ● Seventy to 85% of these cases are odontogenic in origin, the rest are caused by sialadenitis, lymphadenitis, flor of mouth lacerations and infections and or mandibular fractures ● Ludwig's angina is the prototypical submandibular space infection
- 37. Ludwig's angina ● Cellulitic process of the submandibular space, not an abscess ● Involvement of only the submandiblar space ● Gangrene with foul serosangious fluid on incision, no pus ● Involvement of the fascia, muscles and connective tissue ● There is direct spread of infection rather than spread by lymphatics
- 38. Microbiology of deep neck infections: ● Mixed aerobic and anareobic organisms, often with predominance of oral flora ● Gram positive cocci: Group A beta haemolytic sterptococci species is most common ● A hemolytic streptococcal species (strept viridans, strept pneumonae) ● Staph Aureus ● Fusobacterium nucleatum, bactreoids, spirtochaeta, ● Klebsiella and Neisseria species found together ● Ocassionaly H influenza and E coli also isolated ● Poly microbial culture in 90% of patients ● Aerobes in 100% ● Anaerobes in more than 50%
- 39. Management PRINCIPLES ●Airway protection ●Appropriate antimicrobial therapy ●Surgical drainage
- 40. CONCLUSION Early recognition of orofacial infection and prompt appropriate therapy is essential A sound knowledge of anatomy of face and neck is necessary to predict pathways of spread of infection and drain the spaces adequately
- 41. THANK YOU......
Notas do Editor
- A temporalis muscle B masseter muscle C lateral pterygoid D medial pterygoid E superficial temporal space f deep temporal space G submasseteric space, H pterygomandibular space I infratemporal space
- Lateral pharyngeal space to the contents of carotid sheath, int jug vein thrombosis, subacute bacterial endocarditis, pulm emboli, carotid artery thrombosis, CVA, horner syndrome etc
