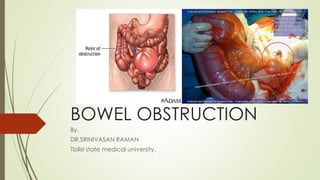
Bowel obstruction
- 1. BOWEL OBSTRUCTION By, DR.SRINIVASAN RAMAN Tbilisi state medical university.
- 2. BOWEL OBSTRUCTION OVERVIEW CLASSIFICATION COMMON CAUSES OF OBSTRUCTION CLINICAL FEATURES INVESTIGATION TREATMENT
- 3. INTRODUCTION Accounts for 5% of all acute surgical admissions Patients are often extremely ill requiring prompt assessment, resuscitation and intensive monitoring Types: Obstruction: A mechanical blockage arising from a structural abnormality that presents a physical barrier to the progression of gut contents. Ileus: is a paralytic or functional variety of obstruction Obstruction is: Partial or complete Simple or strangulated
- 4. CLASSIFICATION Result from atony of the intestine with loss of normal peristalsis, in the absence of a mechanical cause. or it may be present in a non-propulsive form (e.g. mesenteric vascular occlusion or pseudo-obstruction) ADYNAMIC (FUNCTIONAL) Result from atony of the intestine with loss of normal peristalsis, in the absence of a mechanical cause. or it may be present in a non-propulsive form (e.g. mesenteric vascular occlusion or pseudo-obstruction) ADYNAMIC (FUNCTIONAL)
- 5. TYPES OF BOWEL OBSTRUCTION
- 6. TYPES AND CAUSES OF DYNAMIC OBSTRUCTION Intraluminal •Impaction •Foreign bodies •Bezoars •Gallstone Intramural •Congenital atresia •Stricture •Malignancy(15%) Extramural •Bands/ adhesion(40%) •Hernia (12%) •Volvulus •Intussusception •Tumor- benign/malignant
- 8. Peritoneal irritation local fibrin production produces adhesions between apposed surfaces As early as 4 weeks post laparotomy. The majority of patients present between 1-5 years Colorectal Surgery 25% Gynaecological 20% Appendectomy 14% Prevention: good surgical technique, washing of the peritoneal cavity with saline to remove clots, etc, minimizing contact w/ gauze, covering anastomosis & raw peritoneal surfaces
- 9. TREATMENT OF ADHESIVE OBSTRUCTION Initially treat conservatively provided there is no signs of strangulation; should rarely continue conservative treatment for longer than 72 hours At operation, divide only the causative adhesion and limit dissection Laparoscopic adhesiolysis in cases of chronic subacute obstruction
- 10. Hernia Accounts for 20% of SBO Commonest 1. Femoral hernia 2. ID inguinal 3. Umbilical 4. Others: incisional The site of obstruction is the neck of hernia The compromised viscus is with in the sac. Ischaemia occurs initially by venous occlusion, followed by oedema and arterial compromise. Attempt to distinguish the difference between: Incarceration Sliding Obstruction Strangulation is noted by: Persistent pain Discolouration Tenderness Constitutional symptoms
- 11. Volvulus A twisting or axial rotation of a portion of bowel about its mesentery. When complete it forms a closed loop obstruction ischemia Commonest spontaneous type in adult is sigmoid, can be relieved by decompression per anum Surgery is required to prevent or relieve ischaemia Features: palpable tympanic lump (sausage shape) in the midline or left side of abdomen. Constipation, abdominal distension (early & progressive)
- 13. ACUTE INTUSSUSEPTION Occurs when one portion of the gut becomes invaginated within an immediately adjacent segment. Common in 1st year of life Common after viral illness enlargement of Peyer’s patches Ileocolic is the commonest variety in child. Colocolic intussusception commonest in adult An intussusception is composed of three parts : the entering or inner tube; the returning or middle tube; the sheath or outer tube (intussuscipiens).
- 14. Classically, a previously healthy infant presents with colicky pain and vomiting (milk then bile). Between episodes the child initially appears well. Later, they may pass a ‘redcurrant jelly’ stool.
- 16. LARGE BOWEL OBSTRUCTION Distinguishing ileus from mechanical obstruction is challenging Caecum is at the greatest risk of perforation Perforation results in the release of formed feaces with heavy bacterial contamination Aetiology: 1. Carcinoma: The commonest cause, 18% of colonic ca. present with obstruction 2. Benign stricture: Due to Diverticular disease, Ischemia, Inflammatory bowel disease. 3. Volvulus: -Sigmoid Volvulus/ Caecal Volvulus 4. Hernia. 5. Congenital : HirschPrung, anal stenosis and agenesis
- 17. CLINICAL FEATURES Large bowel obstruction distension is early and pronounced. Pain is mild and vomiting and dehydration are late. The proximal colon and caecum are distended on abdominal radiography CARDINAL FEATURES: Colicky pain Vomiting Abd distention Constipation OTHER FEATURES: Dehydration Hypokalaemia Pyrexia Abd tenderness
- 18. PHYSICAL EXAMINATION INSPECTION Abdominal distention, scars, visible peristalsis. PALPATION Mass, tenderness, guarding PERCUSSION Tymphanic, dullness AUSCULTATION Bowel sound are high pitch and increase in frequency
- 19. INVESTIGATIONS: Lab: FBC (leukocytosis, anaemia, hematocrit, platelets) Clotting profile Arterial blood gasses U& Crt, Na, K, Amylase, LFT and glucose, LDH Group and save (x-match if needed) Optional (ESR, CRP, Hepatitis profile) RadiOlogical: Plain ABDOMINAL xrays USS ( free fluid, masses, mucosal folds, pattern of paristalsis, Doppler of mesenteric vasulature, solid organs) Other advanced studies (CT, MRI, Contrast studieS)
- 20. Fluid levels with gas above; ‘stepladder pattern’. Ileal obstruction by adhesions; patient erect. Supine radiograph from a patient with complete small bowel obstruction shows distended small bowel loops in the central abdomen with prominent valvulae conniventes (small white arrow) Figure 3. Lateral decubitus view of the abdomen, showing air-fluid levels consistent with intestinal obstruction (arrows).
- 21. In small bowel Central 3cm thick diameter Vulvulae coniventae Ileum may occur tubeless In large bowel Peripheral diameter 6cm Presence of haustration
- 22. ROLE OF CT Used with iv contrast, oral and rectal contrast (triple contrast). Able to demonstrate abnormality in the bowel wall, mesentery, mesenteric vessels and peritoneum. It can define: the level of obstruction The degree of obstruction The cause: volvulus, hernia, luminal and mural causes The degree of ischaemia Free fluid and gas Ensure: patient vitally stable with no renal failure and no previous alergy to iodine • FIGURE: AXIAL COMPUTED TOMOGRAPHY SCAN SHOWING DILATED, CONTRAST-FILLED LOOPS OF BOWEL ON THE PATIENT’S LEFT (YELLOW ARROWS), WITH DECOMPRESSED DISTAL SMALL BOWEL ON THE PATIENT’S RIGHT (RED ARROWS). THE CAUSE OF OBSTRUCTION, AN INCARCERATED UMBILICAL HERNIA, CAN ALSO BE SEEN (GREEN ARROW), WITH PROXIMALLY DILATED BOWEL ENTERING THE HERNIA AND DECOMPRESSED BOWEL EXITING THE HERNIA.
- 23. CONTRAST STUDIES Barium should not be used in a patient with peritonitis As: follow through, enema Limited use in the acute setting Gastrografin is used in acute abdomen but is diluted Useful in recurrent and chronic obstruction May able to define the level and mural causes. Can be used to distinguish adynamic and mechanical obstruction
- 26. TREATMENT OF INTESTINAL OBSTRUCTION Supportive 1. Resuscitation 2. Ryle tube free flow with 4 hourly aspiration -Decompression of proximal to the obstruction, reduce subsequent aspiration during induction of anesthesia and post extubation. 3. IV drip normal saline / Hartmann (Sodium & water loss during IO) 4. Broad spectrum antibiotic (not mandatory but need in all patient undergoing surgery.
- 27. MANAGEMENT FOR LARGE BOWEL OBSTRUCTION All patients require •Adequate resuscitation •Prophylactic antibiotics •Consenting and marking for potential stoma formation •At operation •Full laparotomy should be performed •Liver should be palpated for metastases •Colon should be inspected for synchronous tumours •Appropriate operations include: •Right sided lesions – right hemicolectomy •Transverse colonic lesion – extended right hemicolectomy •Left sided lesions – various options
- 28. INDICATIONS FOR SURGERY Generalised peritonitis Localised peritonitis Visceral perforation Irreducible hernia Palpable mass lesion Failure to improve Advanced malignancy Incomplete obstruction Advanced malignancy
- 29. SURGERY Three-staged procedure Defunctioning colostomy Resection and anastomosis Closure of colostomy Two-staged procedure Hartmann’s procedure: the surgical resection of the rectosigmoid colon with closure of the rectal stump and formation of an end colostomy. It was used to treat colon cancer or diverticulitis Closure of colostomy
- 31. Complications associated with intestinal obstruction repair include excessive bleeding infection formation of abscesses (pockets of pus) leakage of stool from an anastomosis adhesion formation paralytic ileus (temporary paralysis of the intestines) reoccurrence of the obstruction.
- 32. PARALYTIC ILEUS A state in which there is a failure of transmission of peristaltic waves 2° to neuromuscular failure ( in Auerbach’s and Meissner’s plexuses) Stasis leads to accumulation of fluid and gas within bowel a/w distension, vomiting, absence of bowel sound and absolute constipation Varieties factors: postoperative, infection, reflex ileus and metabolic Radiological: gas filled loops of intestines with multiple fluid levels
- 33. Management: Essence of treatment prevention with use of nasogastric suction and restriction of oral intake until bowel sound and passage of flatus return Maintain electrolyte balance Specific treatment: Removed primary cause Decompressed GI distension If prolong paralytic ileus , consider laparotomy exclude hidden cause and facilitate bowel decompression
- 34. REFERENCE http://emedicine.medscape.com/article/930576-overview#aw2aab6b2b4 http://www.patient.co.uk/doctor/intestinal-obstruction-and-ileus https://www.youtube.com https://en.wikipedia.org/wiki/Bowel_obstruction http://www.webmd.com/digestive-disorders/tc/bowel-obstruction-topic- overview http://www.mayoclinic.org/diseases-conditions/intestinal- obstruction/basics/symptoms/con-20027567
