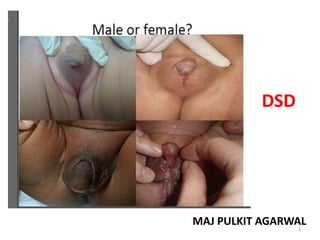
Approach to DSD (Ambiguous genitalia)
- 2. NORMAL SEXUAL DIFFERENTIATION Three steps- 1. Establishment of chromosomal sex at fertilization(46,XX or 46,XY) 2. Development of undifferentiated gonads into testes or ovaries 3. Subsequent differentiation of internal ducts & external genitalia as a result of endocrine functions associated with the gonad present 2
- 3. HOW TO ASSIGN GENDER • Genetic Sex (Karyotype) • External Genitalia • Gonads/reproductive organs • Psychosocial 3
- 4. 4
- 5. 5
- 6. 7
- 7. DISORDERS OF SEXUAL DIFFERENTIATION • When the external genitalia do not have the typical anatomic appearance of normal male or female genitalia. • Infants with ambiguous genitalia have genes of either a male or female, but with some additional characteristics of opposite sex. 8
- 8. 9
- 9. CAUSES OF DSD • 46XX DSD • 46XY DSD • Disorders of Gonadal Differentiation 10
- 10. 46,XX DSD • Previously known as female- pseudohermaphrodites • Normal ovaries • Internal female organs are present • Variable degrees of virilisation of the external genitalia • Causes – CAH – Placental Aromatase Deficiency • Both mother and infant are virilised – Maternal Androgen excess • Maternal CAH, Virilizing tumors, drugs 11
- 11. CAH • 21 Hydroxylase deficiency in >90% (mutation in CYP21A2) • 11 β Hydroxylase or 3 β Hydroxysteroid dehydrogenase deficiency is rare • Easily detected in females • Males: hyperpigmentation of scrotum • Salt wasting: simple virilizing = 3:1 (d/f by PRA and Aldosterone level) 12
- 12. 13
- 13. 46 XY DSD • Incomplete masculinization in a male • Causes – Testicular unresponsiveness to hCG & LH – Disorders of testosterone synthesis • 17 α hydroxylase deficiency, 17-20 lyase deficiency etc – Disorders of testosterone metabolism • 5 α reductase deficiency – End organ resistance • PAIS, CAIS – Vanishing testes syndrome – Lack of AMH receptor ( Persistent Mullerian Duct Syndrome) 14
- 14. GONADAL DIFFERENTIATION DISORDERS • Ovotesticular DSD (True hermaphroditism) – 46XX (70%), 46 XY (10%), mosaics – Internal structures may be mullerian or wolffian depending upon local presence of testosterone/AMH – Histology of gonads is diagnostic: should contain both testicular and follicle containing ovarian tissue • Mixed Gonadal Dysgenesis (MGD) – 45X/46 XY – Testes on one side, streak gonad/dysgenetic testes on other side – Asymmetric external genitalia + single palpable testis, but can vary widely 15
- 15. • 46XY Complete Gonadal Dysgenesis (CGD) – Swyer Syndrome – Complete sex reversal – Abnormal functioning of SRY leads to incomplete testicular differentiation – B/l streak gonads, internal structures are female – Raised as females, usually diagnosed at puberty • 46XX Testicular DSD – Phenotypically male, fail to attain puberty due to inadequate testosterone secretion – Translocation of SRY to X chromosome 16
- 16. 17
- 17. Gonadal and chromosomal characteristics of DSD 18
- 18. EVALUATION 19
- 19. HISTORY Family history • CAH:Neonatal death (male baby with vomiting/dehydration) • Hypospadias/ cryptorchidism • Infertility/Pubertal delay • Consanguinity Pregnancy history -Placental aromatase deficiency allows fetal adrenal androgens to virilize both mother & fetus -Androgen secreting tumors – Medication: Androgens, antiandrogens (finesteride, spironolactone), estrogens 20
- 20. PHYSICAL EXAMINATION General Examination – Dysmorphic features – Evidence of salt wasting skin turgor, poor tone, dehydration, low BP, vomiting, poor feeding – Hyper pigmentation – In adolescent evidence of hirsutism/ virilization Tanner staging 21
- 21. External Genitalia • Phallus – Stretched length (>2.5 cm in male term infant/ < 1cm clitoris in female term infant) – Chordee – Position of orifice • Labioscrotal folds – Separated or fused fusion is an androgen effect – Skin texture rugosity suggests exposure to androgens – Color of the skin ↑↑ pigmentation may be evidence for CAH – Vaginal opening 22
- 22. Gonadal Examination • Palpate labioscrotal tissue & inguinal canal for presence of gonads • Note No. of gonads, size, symmetry, position. • Palpable gonads below the inguinal canal are almost always testicles • Ovotestis may be present as inguinal hernia Rectal exam • To palpate for presence or absence of the uterus 23
- 23. - Complete masculinisation - Normal looking hyperpigmented male genitalia (but no palpable testes) A 46,XX patient known to have congenital adrenal hyperplasia due to 21 α-hydroxylase deficiency 24
- 24. 5α-Reductase deficiency Boys with a small phallus Bifid scrotum Urogenital sinus with perineal hypospadias, and a blind vaginal pouch 25
- 25. Pigmented, short, curved phallus, central urogenital slit, and separated labioscrotal testis A 46,XY patient known to have congenital adrenal hyperplasia due to 3β-hydroxy dehydrogenase deficiency 26
- 26. Androgen Insensitivity Syndromes Partial androgen insensitivity with descended testes in bifid labioscrotal folds Less severe partial androgen insensitivity with severe hypospadias and maldescent of testes 27
- 27. INVESTIGATIONS First Line • Karyotype • Electrolytes • RFT • 17 OHP & Testosterone Chromosome analysis • FISH (SRY) USG pelvis, KUB MRI Genitogram/ cystoscopy Rarely laporoscopy & gonadal biopsy 28
- 28. • Hormonal assays 17 OHP • Done after 48-72 hrs of life (normally elevated in the 1st 2 days of life) • False positive: prematurity, LBW, acute illness • Normal =82-400 ng/dl • >400 CAH • 200-300 ACTH stimulation test 29
- 29. 17OHP Normal/ slight increase Elevated 17OHP Increased CAH rare forms Normal CAH 21 OH Normal 17OHP Gonadal Dysgenesis/ Ovotesticular DSD/ Non CAH DSD Elevated CAH 21 OH ACTH Intermediates 30
- 30. • 21-hydroxylase def: ↑↑ 17-OHP • Normal 17-OHP + 46XX ACTH stim test check (11-deoxycorticosterone, 11- deoxycortisol, 17-hydroxypregnenolone ) to detect other adrenal enzymatic defects • 11OH: 11 deoxycortisol, 11 deoxycorticosterone ↑ • 3β HSD: 17OHP ↑, 17 OH Pregnenolone ↑↑ 31
- 31. Testosterone Normal/ Slight Increase No increase, normal T:DHT ?PAIS Phallus increase <2+/- 0.6 Very high CAIS Low No change Gonadal dysgenesis/LH receptor mutation/ Gest loss of testes/defect of Testosterone synth T:DHT >20:1 5 α reductase def T:DHT<0.8:1 17 β HSD deficiency HCG stimulation HCG stimulation Monthly testosterone x 3 months 32
- 32. 33
- 33. 34
- 34. THANKS 35