Endocarditis
•Download as PPTX, PDF•
0 likes•371 views
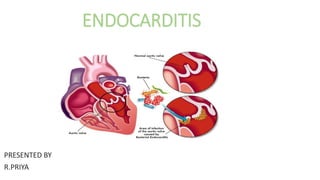
ENDOCARDITIS is the internal inflammation of the endocardium. and some value or has affected causes of this infection and noninfective endocarditis, management of the valve replacement medical management is antibiotic.
Report
Share
Report
Share
Recommended
Recommended
More Related Content
What's hot
What's hot (20)
Similar to Endocarditis
Similar to Endocarditis (20)
More from Priya
More from Priya (20)
Recently uploaded
PEMESANAN OBAT ASLI : +6287776558899
Cara Menggugurkan Kandungan usia 1 , 2 , bulan - obat penggugur janin - cara aborsi kandungan - obat penggugur kandungan 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 bulan - bagaimana cara menggugurkan kandungan - tips Cara aborsi kandungan - trik Cara menggugurkan janin - Cara aman bagi ibu menyusui menggugurkan kandungan - klinik apotek jual obat penggugur kandungan - jamu PENGGUGUR KANDUNGAN - WAJIB TAU CARA ABORSI JANIN - GUGURKAN KANDUNGAN AMAN TANPA KURET - CARA Menggugurkan Kandungan tanpa efek samping - rekomendasi dokter obat herbal penggugur kandungan - ABORSI JANIN - aborsi kandungan - jamu herbal Penggugur kandungan - cara Menggugurkan Kandungan yang cacat - tata cara Menggugurkan Kandungan - obat penggugur kandungan di apotik kimia Farma - obat telat datang bulan - obat penggugur kandungan tuntas - obat penggugur kandungan alami - klinik aborsi janin gugurkan kandungan - ©Cytotec ™misoprostol BPOM - OBAT PENGGUGUR KANDUNGAN ®CYTOTEC - aborsi janin dengan pil ©Cytotec - ®Cytotec misoprostol® BPOM 100% - penjual obat penggugur kandungan asli - klinik jual obat aborsi janin - obat penggugur kandungan di klinik k-24 || obat penggugur ™Cytotec di apotek umum || ®CYTOTEC ASLI || obat ©Cytotec yang asli 200mcg || obat penggugur ASLI || pil Cytotec© tablet || cara gugurin kandungan || jual ®Cytotec 200mcg || dokter gugurkan kandungan || cara menggugurkan kandungan dengan cepat selesai dalam 24 jam secara alami buah buahan || usia kandungan 1_2 3_4 5_6 7_8 bulan masih bisa di gugurkan || obat penggugur kandungan ®cytotec dan gastrul || cara gugurkan pembuahan janin secara alami dan cepat || gugurkan kandungan || gugurin janin || cara Menggugurkan janin di luar nikah || contoh aborsi janin yang benar || contoh obat penggugur kandungan asli || contoh cara Menggugurkan Kandungan yang benar || telat haid || obat telat haid || Cara Alami gugurkan kehamilan || obat telat menstruasi || cara Menggugurkan janin anak haram || cara aborsi menggugurkan janin yang tidak berkembang || gugurkan kandungan dengan obat ©Cytotec || obat penggugur kandungan ™Cytotec 100% original || HARGA obat penggugur kandungan || obat telat haid 1 bulan || obat telat menstruasi 1-2 3-4 5-6 7-8 BULAN || obat telat datang bulan || cara Menggugurkan janin 1 bulan || cara Menggugurkan Kandungan yang masih 2 bulan || cara Menggugurkan Kandungan yang masih hitungan Minggu || cara Menggugurkan Kandungan yang masih usia 3 bulan || cara Menggugurkan usia kandungan 4 bulan || cara Menggugurkan janin usia 5 bulan || cara Menggugurkan kehamilan 6 Bulan
________&&&_________&&&_____________&&&_________&&&&____________
Cara Menggugurkan Kandungan Usia Janin 1 | 7 | 8 Bulan Dengan Cepat Dalam Hitungan Jam Secara Alami, Kami Siap Meneriman Pesanan Ke Seluruh Indonesia, Melputi: Ambon, Banda Aceh, Bandung, Banjarbaru, Batam, Bau-Bau, Bengkulu, Binjai, Blitar, Bontang, Cilegon, Cirebon, Depok, Gorontalo, Jakarta, Jayapura, Kendari, Kota Mobagu, Kupang, LhokseumaweCara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...Cara Menggugurkan Kandungan 087776558899
Ahmedabad Call Girls Book Now 9630942363 Top Class Ahmedabad Escort Service Available
9630942363 Ahmedabad Escort Service Ahmedabad Call Girls Ahmedabad Escorts Service Ahmedabad Call Girl Russian 9630942363 Russian Ahmedabad Escort Service Vip Ahmedabad Escort Service Ahmedabad Call Girls Housewife Model College Girls Aunty Bhabhi Ahmedabad 9630942363 Genuine Ahmedabad Call Girl Escort ServiceAhmedabad Call Girls Book Now 9630942363 Top Class Ahmedabad Escort Service A...

Ahmedabad Call Girls Book Now 9630942363 Top Class Ahmedabad Escort Service A...GENUINE ESCORT AGENCY
Genuine Call Girls Hyderabad 9630942363 Book High Profile Call Girl in Hyderabad Genuine Escort ServiceGenuine Call Girls Hyderabad 9630942363 Book High Profile Call Girl in Hydera...

Genuine Call Girls Hyderabad 9630942363 Book High Profile Call Girl in Hydera...GENUINE ESCORT AGENCY
Recently uploaded (20)
Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...
Dehradun Call Girl Service ❤️🍑 8854095900 👄🫦Independent Escort Service Dehradun

Dehradun Call Girl Service ❤️🍑 8854095900 👄🫦Independent Escort Service Dehradun
Premium Call Girls Nagpur {9xx000xx09} ❤️VVIP POOJA Call Girls in Nagpur Maha...

Premium Call Girls Nagpur {9xx000xx09} ❤️VVIP POOJA Call Girls in Nagpur Maha...
ANATOMY AND PHYSIOLOGY OF REPRODUCTIVE SYSTEM.pptx

ANATOMY AND PHYSIOLOGY OF REPRODUCTIVE SYSTEM.pptx
Call Girls Bangalore - 450+ Call Girl Cash Payment 💯Call Us 🔝 6378878445 🔝 💃 ...

Call Girls Bangalore - 450+ Call Girl Cash Payment 💯Call Us 🔝 6378878445 🔝 💃 ...
💚Chandigarh Call Girls 💯Riya 📲🔝8868886958🔝Call Girls In Chandigarh No💰Advance...

💚Chandigarh Call Girls 💯Riya 📲🔝8868886958🔝Call Girls In Chandigarh No💰Advance...
Chandigarh Call Girls Service ❤️🍑 9809698092 👄🫦Independent Escort Service Cha...

Chandigarh Call Girls Service ❤️🍑 9809698092 👄🫦Independent Escort Service Cha...
Kolkata Call Girls Naktala 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Girl Se...

Kolkata Call Girls Naktala 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Girl Se...
❤️Chandigarh Escorts Service☎️9814379184☎️ Call Girl service in Chandigarh☎️ ...

❤️Chandigarh Escorts Service☎️9814379184☎️ Call Girl service in Chandigarh☎️ ...
🚺LEELA JOSHI WhatsApp Number +91-9930245274 ✔ Unsatisfied Bhabhi Call Girls T...

🚺LEELA JOSHI WhatsApp Number +91-9930245274 ✔ Unsatisfied Bhabhi Call Girls T...
💚Chandigarh Call Girls Service 💯Piya 📲🔝8868886958🔝Call Girls In Chandigarh No...

💚Chandigarh Call Girls Service 💯Piya 📲🔝8868886958🔝Call Girls In Chandigarh No...
Call Girl In Indore 📞9235973566📞 Just📲 Call Inaaya Indore Call Girls Service ...

Call Girl In Indore 📞9235973566📞 Just📲 Call Inaaya Indore Call Girls Service ...
Ahmedabad Call Girls Book Now 9630942363 Top Class Ahmedabad Escort Service A...

Ahmedabad Call Girls Book Now 9630942363 Top Class Ahmedabad Escort Service A...
Call Girls Mussoorie Just Call 8854095900 Top Class Call Girl Service Available

Call Girls Mussoorie Just Call 8854095900 Top Class Call Girl Service Available
💚Call Girls In Amritsar 💯Anvi 📲🔝8725944379🔝Amritsar Call Girl No💰Advance Cash...

💚Call Girls In Amritsar 💯Anvi 📲🔝8725944379🔝Amritsar Call Girl No💰Advance Cash...
Call 8250092165 Patna Call Girls ₹4.5k Cash Payment With Room Delivery

Call 8250092165 Patna Call Girls ₹4.5k Cash Payment With Room Delivery
Circulatory Shock, types and stages, compensatory mechanisms

Circulatory Shock, types and stages, compensatory mechanisms
❤️Amritsar Escorts Service☎️9815674956☎️ Call Girl service in Amritsar☎️ Amri...

❤️Amritsar Escorts Service☎️9815674956☎️ Call Girl service in Amritsar☎️ Amri...
Jaipur Call Girl Service 📞9xx000xx09📞Just Call Divya📲 Call Girl In Jaipur No💰...

Jaipur Call Girl Service 📞9xx000xx09📞Just Call Divya📲 Call Girl In Jaipur No💰...
Genuine Call Girls Hyderabad 9630942363 Book High Profile Call Girl in Hydera...

Genuine Call Girls Hyderabad 9630942363 Book High Profile Call Girl in Hydera...
Endocarditis
- 2. INTRODUCTION Infective endocarditis is a rare disease, with an incidence of two to six episodes per 100,000 habitants/year. Incidence is higher in elderly people; besides, this group is often affected by many comorbidities.
- 3. DEFINITION Endocarditis is an inflammation of the inner layer of the heart , the endocardium. It usually involves the heart valves, Other structures that may be involved include the interventricular septum , the chordae tendineae, the mural endocardium, or the surfaces of intracardiac devices.
- 4. TYPES Infective endocarditis, also called bacterial endocarditis, is an infection caused by bacteria that enter the bloodstream and settle in the heart lining, a heart valve or a blood vessel. The cause is typically abacterial infection and less commonly a fungal infection Risk factors include valvular heart disease including rheumatic disease, rheumatic disease ,congenital heart disease ,artificial valves , hemodialysis , intravenous drug use, and electronic pacemakers. The bacterial most commonly involved are streptococci. Noninfective endocarditis refers to formation of sterile platelet and fibrin thrombi on cardiac valves and adjacent endocardium in response to trauma, circulating immune complexes, vasculitis, or a hypercoagulable state.
- 5. CAUSES Endocarditis can involve the heart muscle, heart valves, or lining of the heart. Some people who develop endocarditis have a: •Birth defect of the heart •Damaged or abnormal heart valve •History of endocarditis •New heart valve after surgery •Parenteral (intravenous) drug addiction •Long-term intravenous line in place Endocarditis begins when germs enter the bloodstream and then travel to the heart. •Bacterial infection is the most common cause of endocarditis. •Endocarditis can also be caused by fungi, such as Candida. •In some cases, no cause can be found. Germs are most likely to enter the bloodstream during: •Central venous access lines •Injection drug use, from the use of unclean (unsterile) needles •Recent dental surgery •Other surgeries or minor procedures to the breathing tract, urinary tract, infected skin, or bones and muscles
- 6. RISK FACTOR •Older age. Endocarditis occurs most often in older adults over age 60. •Artificial heart valves. Germs are more likely to attach to an artificial (prosthetic) heart valve than to a normal heart valve. •Damaged heart valves. Certain medical conditions, such as rheumatic fever or infection, can damage or scar one or more of your heart valves, increasing the risk of infection. •Congenital heart defects. If you were born with certain types of heart defects, such as an irregular heart or abnormal heart valves, your heart may be more susceptible to infection. •Implanted heart device. Bacteria can attach to an implanted device, such as a pacemaker, causing an infection of the heart's lining. •A history of endocarditis. Endocarditis can damage heart tissue and valves, increasing the risk of a future heart infection. •A history of illegal IV drug use. People who use illegal drugs by injecting them are at a greater risk of endocarditis. The needles used to inject drugs can be contaminated with the bacteria that can cause endocarditis. •Poor dental health. A healthy mouth and healthy gums are essential for good health. If you don't brush and floss regularly, bacteria can grow inside your mouth and may enter your bloodstream through a cut on your gums. •Long-term catheter use. Having a catheter in place for a long period of time (indwelling catheter) increases your risk of endocarditis.
- 8. SIGNS AND SYMPTOMS Common signs and symptoms of endocarditis include: •Aching joints and muscles •Chest pain when you breathe •Fatigue •Flu-like symptoms, such as fever and chills •Night sweats •Shortness of breath •Swelling in your feet, legs or abdomen •A new or changed heart murmur, which is the heart sound made by blood rushing through your heart Less common signs and symptoms of endocarditis can include: •Unexplained weight loss •Blood in your urine, which you might be able to see or that your doctor might see when he or she views your urine under a microscope •Tenderness in your spleen, which is an infection-fighting organ located just below your left rib cage •Red spots on the soles of your feet or the palms of your hands (Janeway lesions) •Red, tender spots under the skin of your fingers or toes (Osler's nodes) •Tiny purple or red spots, called petechiae (puh-TEE-kee-ee), on the skin, in the whites of your eyes or inside your mouth
- 9. DIAGNOSTIC EVALUATION •Blood culture test. A blood culture test is used to identify any germs in your bloodstream. Blood culture test results help your doctor choose the most appropriate antibiotic or combination of antibiotics. •Complete blood count. This blood test can tell your doctor if you have a lot of white blood cells, which can be a sign of infection. A complete blood count can also help diagnose low levels of healthy red blood cells (anemia), which can be a sign of endocarditis. Other blood tests also may be done to help your doctor determine the diagnosis. •Echocardiogram. An echocardiogram uses sound waves to produce images of your heart while it's beating. This test shows how your heart's chambers and valves are pumping blood through your heart. Your doctor may use two different types of echocardiograms to help diagnose endocarditis. In a transthoracic echocardiogram, sound waves directed at your heart from a wand like device (transducer) held on your chest produce video images of your heart in motion. This test lets your doctor see the heart's structure and check it for any signs of damage. A transesophageal echocardiogram gives your doctor a closer look at your heart valves. During this test, a small transducer attached to the end of a tube is inserted down the tube leading from your mouth to your stomach (esophagus). This test provides much more detailed pictures of your heart than is possible with a transthoracic echocardiogram. •Electrocardiogram (ECG or EKG). An ECG is used to measure the timing and duration of your heartbeats. It isn't specifically used to diagnose endocarditis, but it can show your doctor if something is affecting your heart's electrical activity. During an ECG, sensors that can detect your heart's electrical activity are attached to your chest, arms and legs. •Chest X-ray. A chest X-ray can show your doctor the condition of your lungs and heart. It can help determine if endocarditis has caused heart swelling or if any infection has spread to your lungs. •Computerized tomography (CT) scan or magnetic resonance imaging (MRI). You may need a CT scan or an MRI scan of your brain, chest or other parts of your body if your doctor thinks that infection has spread to these areas.
- 10. MANAGEMENT IV antibiotics for 6 weeks(PENNICILLIEN) SURGERY Heart valve surgery may be needed to treat persistent endocarditis infections or to replace a damaged valve. Surgery is also sometimes needed to treat endocarditis that's caused by a fungal infection. Depending on your condition, your doctor may recommend repairing your damaged valve or replacing it with an artificial valve made of cow, pig or human heart tissue (biological tissue valve) or man-made materials (prosthetic mechanical valve). PREVENTION •Tell your doctors and dentists you have heart disease that places you at greater risk of developing endocarditis. •Take antibiotics before the following procedures (as recommended by the American Heart Association): • All dental procedures that involve manipulation of gingival tissue or the periapical region of teeth, or perforation of the oral mucosa. • Procedures of the respiratory tract or infected skin, tissues just under the skin, or musculoskeletal tissue