CVS anti arrhythmic drugs
- 2. What is an Arrhythmia ? Irregular rhythm Abnormal Rate Conduction abnormality
- 3. What causes an arrhythmia? Changes in automaticity of the pacemaker Ectopic foci causing abnormal APs Reentry tachycardias Block of conduction pathways Abnormal conduction pathways (WPW) Electrolyte disturbances & Drugs Hypoxic/ Ischemic tissue can undergo spontaneous depolarization & become an ectopic pacemaker
- 4. Important cardiac arrhythmias Extra systoles PSVT Atrial flutter Atrial fibrillation Ventricular tachycardia Torsade's de pointes Ventricular fibrillation AV block
- 5. Normal Sinus Rhythm Heart rhythm is determined by SA node = Cardiac Pacemaker Called Sinus Rhythm Specialised pacemaker cells spontaneously generate APs APs spread through the conducting pathways Normal sinus rate 60-100 beats/min
- 6. Conducting System SAN AP triggers atrial depolarisation AVN Only pathway for AP to enter ventricles Conducts slowly: Complete atrial systole appear before ventricular systole Conducts rapidly through Bundles of His & Purkinje Ventricular depolarization & contraction
- 7. Conducting System Permits rapid organized depolarization of ventricular myocytes Necessary for the efficient generation of pressure during systole Atrial activation complete 0.09s after SAN firing Delay at AVN Septum activated 0.16s Whole ventricle activated by 0.23s
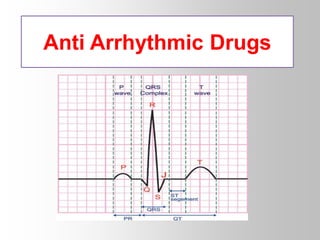
- 8. Cardiac Action Potential Phase 4: RMP AP depolarizes cells to threshold -70mV Phase 0: Rapid depolarization Caused by a transient opening of fast Na channels Increases inward directed depolarizing Na+ currents Generate "fast-response" APs
- 9. Cardiac Action Potential Phase 1: Initial repolarization Open K channel: transient outward hyperpolarizing K+ current Large increase in slow inward gCa++ occurs at the same time L-type CaCh open Repolarization delayed Phase 2: Plateau phase Plateau phase prolongs AP duration vs APs in nerves & skeletal muscle
- 10. Cardiac Action Potential Phase 3: Repolarization K channels open Inactivation of Ca++ channels Action potential in non- pacemaker cells is primarily determined by relative changes in fast Na+, slow Ca++ and K+ conductances and currents
- 11. Refractory Periods Once an AP is initiated, there is a period (phase 0,1,2, part 3) that a new AP cannot be initiated. Effective or Absolute refractory period (ERP or ARP) Stimulation of cell by adjacent cell depolarizing does not produce new propagated APs Prevents compounded APs from occurring & limits frequency of depolarization and HR
- 12. Regulation of Cardiac APs SNS - Increased with concurrent inhibition vagal tone: NA binds to B1 Rec Increases cAMP Increases Ca & Na in Decreases K out Increases slope phase 0 Non-Nodal tissue: More rapid depolarization More forceful contraction Pacemaker current enhanced Increase slope phase 4 Pacemaker potential more rapidly reaches threshold Rate increased
- 13. Regulation of Cardiac APs PSNS (Vagal N) Ach binds M2 rec Increases gK+ Decreases inward Ca & Na Non-Nodal tissue: More rapid depolarization More forceful contraction Pacemaker current suppressed Decreases pacemaker rate Decrease slope of Phase 4 Hyperpolarizes in Phase 4 Longer time to reach threshold voltage
- 14. Atrial Fibrillation & Flutter • Normally, the top chambers (atria) contract & push blood into the bottom chambers (ventricles). • In atrial fibrillation the atria beat irregularly. • In atrial flutter the atria beat regularly, but faster than usual & more often than the ventricles so, you may have 4 atrial beats to every 1 ventricular beat.
- 15. Atrial Fibrillation & Flutter • Atrial flutter is less common than atrial fibrillation • Atrial flutter is less common, but has similar symptoms (feeling faint, tiredness, palpitations, shortness of breath or dizziness). • Some people have mild symptoms, others have none at all.
- 16. Torsade's de pointes (TdP) French for “twisting of the points” is one of several types of life- threatening heart rhythm disturbances. In the case of TdP the heart's 2 lower chambers (ventricles) beat faster than the upper chambers (atria) TdP is associated with a prolonged QT interval which may be congenital or acquired. Torsade usually terminates spontaneously but frequently recurs & may degenerate into ventricular fibrillation.
- 17. 70% of acute MI, 50% of those given GA irregularity in cardiac rhythm Ventricular fibrillation (VF) sudden cardiac death Currently focus on usage of electrical devices Drugs - treatment of AF & prevention of VF 17 7 October 2021 In General
- 18. Rationale for Antiarrhythmic Drugs Restore normal rhythm, rate & conduction or prevent more dangerous arrhythmias Alter conduction velocity (SAN or AVN) Alter slope 0 depolarization Alter excitability of cardiac cells by changing duration of ERP ERP Interrupts tachy caused by reentry Suppress abnormal automaticity
- 19. 19 Vaughan William & Singh Classification Classes 1, 2, 3, 4 – 1970’s Sub classified by Harrison for clinical utility 7 October 2021 DR. BRAMAH N SINGH DR. VAUGHAN WILLIAM
- 20. Vaughan Williams & Singh Classification I • Membrane stabilizing agents (Na+ channel blockers) • Ia-Quinidine, Procainamide, Disopyramide • Ib- Lidocaine, Mexiletine, Phenytoin, Tocainide • Ic- Propafenone, Flecainide, Encainide II • β blockers • Propranolol, Esmolol, Sotalol III • Agents widening Action Potential (K+ channel blockers) • Amiodarone, Dronedarone, Dofetilide, Ibutilide, Bretylium IV • Ca2+ channel blockers • Verapamil, Diltiazem 20 7 October 2021
- 21. Class Ia similar to Class III Propranolol (of class II) has also class I action Sotalol & Bretylium has both class II & class III actions NOTE: Drugs for Paroxysmal Supraventricular Tachycardia (PSVT) Adenosine Digoxin Others Atropine MgSo4
- 22. Phases of AP
- 23. Phases of AP
- 24. Re-entry In normal tissue, if a single Purkinje fibre forms two branches (1 & 2), the AP will travel down each branch. An electrode (*) in a side branch off of branch 1 would record single, normal AP as they are conducted down branch 1 and & into the side branch. If branches 1 & 2 are connected together by a common, connecting pathway (branch 3), the AP that travel into branch 3 will cancel each other out.
- 25. PURKINJE JUNCTION Reentry can occur if branch 2, for e.g., has a unidirectional block. In such a block, impulses can travel retrograde (from branch 3 into branch 2). When this condition exists, an AP will travel down the branch 1, into branch 3, and then travel retrograde through the unidirectional block in branch 2 (blue line). Within the block (gray area), the conduction velocity is reduced because of depolarization. When the AP exits the block, if it finds the tissue excitable, then the AP will continue by travelling down (i.e., reenter) the branch 1. If the AP exits the block in branch 2 & finds the tissue unexcitable, then the AP will die.
- 26. Principles in Treatment of Arrhythmias • Do not treat all arrhythmias • Treatment with antiarrhythmics needed if – Uncomfortable palpitations – Risk to life – Causing hypotension, breathlessness, cardiac failure – Can progress to more serious arrhythmias Restore to sinus rhythm, control ventricular rate, or change to a more desirable pattern of electrical/ mechanical activity
- 27. Phases of AP Reduce rate of Phase 0 depolarization Decrease slope of phase 4 Widens APD or ERP increased Shorten action potential and reduce automaticity
- 28. Class -I Drugs Class IA – Quinidine, Procainamide, Disopyramide & Class IC – Propafenone, Flecainide Block Na+ channel in open state Delay AV conduction Delay recovery of channel Class IB – Lignocaine, Mexiletine Block Na+ channels in inactivated state No effect on AV conduction or recovery Although similar, class IC actions more potent than IA
- 29. Quinidine- D- isomer of quinine Na block Reduce automaticity K block Prolong refractoriness Alpha block Hypotension Antivagal action
- 30. Quinidine- D- isomer of quinine ADR Torsade de pointes, VF, Angioedema, Thrombocytopenia, Cinchonism: ringing in ears, deafness, vertigo, visual disturbances
- 31. Quinidine- D- isomer of quinine Interactions: Increase digoxin levels, Torsade de points in Hypokalemia, Cardiac depression with Beta blockers. Uses: Maintain sinus rhythm after control of AF or Afl, Rarely in ventricular arrhythmias Not preferred due to ADRs Dose: 100 – 200 mg TDS
- 32. Procainamide Similar to quinidine, except that Less effective for ectopics Less depression of AV conduction Less antivagal action; No Alpha blocking action Metabolism: Acetylation metabolite is K blocker & prolong repolarization. Fast and slow acetylators based on metabolism
- 33. Procainamide ADR GI disturbance Confusion Flushing Hypotension Torsades de pointes Hypersensitivity SLE (in slow acetylators) Uses: Monomorphic VT, WPW VT (Not suitable for long term treatment) Dose: 0.5 to 1 gram oral or im
- 34. Disopyramide Similar to quinidine, except that No alpha blocking action Prominent anti cholinergic action Negative inotropic effect on ventricle ADR Dry mouth Constipation Urinary retention Decrease cardiac output
- 35. Disopyramide Uses: Prevention of Ventricular Arrhythmias Maintenance after cardioversion for AF & AFl C/I Sick sinus, Cardiac failure, Prostate hypertrophy Dose: 100 – 150 mg QID or TDS.
- 36. Propafenone Potent Na channel blocker also block beta receptors ADR Nausea, vomiting, bitter taste, constipation, blurred vision Caution Can precipitate CHF & Bronchospasm Uses Reserve drug for ventricular arrhythmia, re-entry tachycardia, to maintain sinus rhythm in AF Dose: 150 mg BD to 300 mg TDS
- 37. Flecainide Potent Na channel blocker More proarrhythmic Caution CAST study showed increase mortality in MI patients Uses Resistant recurrent AF, WPW without CHF Moricizine Withdrawn from market
- 38. Proarrhythmic Drugs Class I C Propafenone Beta blocker Sotalol Class III antiarrhythmic drugs Amiodarone Dronedarone Dofetilide Ibutilide
- 39. Lignocaine/ Lidocaine Na block in inactive state reduce automaticity in ectopics No effect on atria; do not affect SA node Suppress re-entrant ventricular arrhythmia Orally Inactive – parenteral action lasts 10 – 20 min
- 40. Lignocaine/ Lidocaine ADR Paresthesia, twitching, fits, disorientation, drowsiness Interactions Propranolol reduce hepatic blood flow & prolong duration of action Uses Ventricular tachyarrhythmias following MI, surgery, digitalis toxicity Dose 50 – 100 mg bolus iv followed by 1 – 3 mg/ min infusion
- 41. Mexiletine Also local anesthetic Active orally as antiarrhythmic. Activity similar to ligoncaine ADR Bradycardia, hypotension, AV block, tremor, neurological symptoms Uses Ventricular tachyarrhythmias following MI; orally used to suppress VT for long term
- 42. Propranolol Suppress adrenergically mediated ectopic activity Direct membrane stabilizing action at high dose only Reduce automaticity if it is high due to adrenergic effect Uses: Sinus tachycardia, Atrial or Nodal Extra Systoles, PSVT, Arrhythmias due to Pheochromocytoma, Halothane anesthesia Caution: Can cause bradycardia in WPW
- 43. Sotalol Beta blocker with K channel blocking action (Class III action too) Prolong ERP, delay AV conduction Suppress adrenergically mediated ectopic activity Direct membrane stabilizing action at high dose only Reduce automaticity if it is high due to adrenergic effect Uses: Polymorphic VT & for maintaining sinus rhythm in AF/ AFl Caution: Risk of Torsade De Pointes; C/I – Patients with long QT interval
- 44. Esmolol Short acting Beta blocker given as i.v. Uses: Supraventricular tachycardia Anesthesia associated arrhythmias
- 45. Amiodarone Blocks inactive Na channel, delayed rectifier K channel, myocardial Ca channels & beta receptors Reduce ectopic automaticity Very long duration of action: 3- 8 weeks half life
- 46. Amiodarone ADR GIT symptoms Photosensitization Pigmentation Corneal microdeposits Pulmonary alveolitis & fibrosis Peripheral neuropathy Hypothyroidism & Hyperthroidism
- 47. Amiodarone Interactions: Increase digoxin & warfarin levels. AV block with beta blockers Uses: Ventricular & supraventricular arrhythmias, VT and VF
- 48. Dofetilide, Ibutilide Newer anti-arrhythmic drugs (Pure Class III drugs) Block delayed rectifier K channels prolong APD & ERP Uses: Maintain sinus rhythm post conversion from AF or AFl Bretylium K channel block; adrenergic neurone blocker Rarely used for reversal of VF
- 49. Verapamil & Diltiazem Block L type calcium channel and delay their recovery Suppress automaticity Prolong AV node ERP Suppress re-entry based on AV node Poor efficacy in ventricular arrhythmias
- 50. Verapamil & Diltiazem Uses: PSVT without hypotension or CHF, AF or Afl to control ventricular rate. Caution: Avoid in re-entry arrhythmia. Avoid in patients with heart block, with digitalis toxicity and VT
- 51. Adenosine SA node, AV node and atria A1 adenosine receptor (GPCR) Activation of A1 - membrane hyperpolarization by Ach sensitive K channels Bradycardia, slowing of conduction, reduced excitability Depress re-entry circuit; Transient coronary dilatation Very short acting (10 sec). Uptake by RBC and endothelial cells Dipyridamole inhibits uptake & Theophylline antagonize A1 R
- 52. Adenosine Uses: PSVT, coronary dilatation in procedures, controlled hypotension in surgery ADR: Dyspnea, chest pain, hypotension, flushing, bronchospasm Dose: Adenosine base 6 – 12 mg; ATP 10 – 20 mg