OPSI Splenectomy by Dr. Aryan
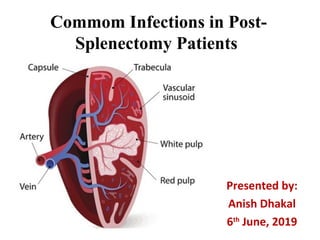
- 1. Commom Infections in Post- Splenectomy Patients Presented by: Anish Dhakal 6th June, 2019
- 2. SPLEEN • Largest lymphoid organ in body • Filtering 10–15% of the body's blood volume per minute. • Major site of early immunoglobulin M production, which is important in the acute clearance of pathogens from the bloodstream. • When its function is absent or reduced, the ability to fight off infection is impaired, particularly from encapsulated bacterial organisms.
- 4. Indications for Splenectomy • Hemolytic anemia • Idiopathic thrombocytopenic purpura. • Bleeds following physical trauma or spontaneous rupture • Hypersplenism • For diagnosing certain lymphomas • The spread of gastric cancer to splenic tissue
- 5. Overwhelming post-splenectomy infection (OPSI) • Is a rare but rapidly fatal infection occurring in individuals following removal of the spleen. • The infections are typically characterized by either meningitis or sepsis, and are caused by encapsulated organisms. • Most infections occur in the first few years following splenectomy, but the risk of OPSI is lifelong. • Once an infection occurs, the mortality rates are high, ranging from 38% to 69%, and fulminant infections frequently develop in patients who are relatively young.
- 6. • Encapsulated organisms are the most virulent pathogens to patients with decreased or absent splenic function – Streptococcus pneumoniae -90% – Haemophilus influenza type B – Neisseria meningitidis – Escherichia coli – Klebsiella pneumoniae – Salmonella typhi Etiology:
- 7. • Coexisting medical conditions, such as malignancy or immunosuppressive disorders, may predispose asplenic patients to infection, further increasing their risk for OPSI.
- 8. Clinical presentation of OPSI • Often begins with mild, nonspecific symptoms • Patients usually have a fever and may complain of headache, chills, malaise, and various GI symptoms • However, this prodrome is usually very brief and progresses rapidly to symptoms of septic shock, including hypotension, oliguria, hypoglycemia, and disseminated intravascular coagulopathy
- 9. Cont.. • Patients may develop concomitant meningitis or pneumonia, or they may experience convulsions or cardiovascular collapse. • Death can occur within 24 to 48 hours of illness onset. • Mortality is high despite aggressive antibiotic therapy and intensive medical care • Patients who survive often have serious long-term sequelae, such as deafness; osteomyelitis; or extensive tissue necrosis, which may potentially require amputation when extremities are involved.
- 10. Investigation • CBC: Long term effect minimal. Initially leukocytosis and thrombocytosis • Blood, urine, and sputum should be cultured on hospital admission. • PBS: Howell-Jolly bodies present in erythrocytes of patients without a spleen • Lumbar puncture is an important tool in diagnosing possible meningitis, especially in small children. • Chest radiographs are indicated anytime pneumonia is suspected
- 11. Management • Initiation of treatment should never be postponed until the results of these tests are available because bacterial proliferation occurs at an accelerated pace. • Empiric oral antibiotics may be started by the patient at home, or antibiotics can be given IM or IV at the primary care provider’s . • The antibiotic of choice for treating OPSI has traditionally been IV penicillin.
- 12. Cont.. • Ceftriaxone 100 mg/kg IV or IM, maximum 2 g per dose. • IV vancomycin 60 mg/kg/d in divided doses every 6 hours, maximum 4 g per day. • Regimens may be adjusted as the results of sensitivity testing become available.
- 13. PREVENTION OF OPSI • Vaccine with pneumococcal, Haemophilus influenzae type B. meningococcal group C and influenza vaccination at least 2-3 wks before elective splenectomy. • Unimmunized patients should receive the vaccine shortly after surgery but may be less effective. • Pneumococcal re- immunisation should be given at least 5 years and influenza annually and must be documented.
- 14. Cont… • Life- long prophylactic penicilline V 500 mg twice daily is recommended. In penicillin- allergic consider macrolide. • Patient should be educated regarding the risk of infection and methods of prophylaxis. • Animal bites should be promptly treated to prevent serious soft tissue infection and septicaemia. • Should also be encouraged to wear an identification bracelet or carry a wallet card notifying others of their condition in emergency situations.
- 15. Referances • Harrison‘s Principles of Internal Medicine, 20th edition • Sandra L. Moffett, PA-C.Overwhelming postsplenectomy infection: Managing patients at risk. Journal of American Physician Assistants 2009; 22(7) • Morgan Tl, Tomich EB. Overwhelming Post-splenectomy Infection (OPSI). J Emerg Med. 2012;43(4):758-763. • Takehiro Okabayashi, Kazuhiro Hanazaki. Overwhelming postsplenectomy infection syndrome in adults - A clinically preventable disease. WorldJournal of gastroenterology 2008 Jan 14; 14(2): 176–179. • Davidson’s Principles of Medicine, 23rd edition
