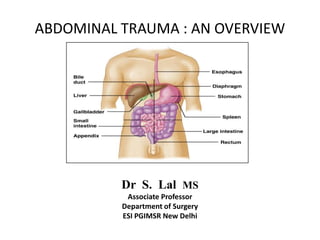
Abdominal trauma : an overview
- 1. ABDOMINAL TRAUMA : AN OVERVIEW Dr S. Lal MS Associate Professor Department of Surgery ESI PGIMSR New Delhi
- 2. Introduction • Abdominal trauma is regularly encountered in the emergency department • One of the leading cause of death and disability • Identification of serious intra-abdominal injuries is often challenging • Many injuries may not manifest during the initial assessment and treatment period
- 3. Epidemiology • Peak incidence Abdominal Trauma 15 - 30yr • More than 1.5 Lac people die every year as a result of injuries by motor vehicle accident , fall, suicide and homicide • Injury accounts for 10% of all deaths • Estimates indicate that by 2020, 8.4 million people will die yearly. • Prevalence: 13%
- 4. Types of Abdominal Trauma 1.Blunt Trauma 2.Penetrating Trauma -Stab -Gun shot Injury
- 5. M.V. Accidents involving high kinetic energy and acceleration or deceleration forces - 60%
- 6. Direct blow to abdomen - 15% Fall- 6-9%
- 7. Blunt Trauma Abdomen (contd.) • Child Abuse • Domestic Violence • Iatrogenic injury -Endoscopic /Laparoscopic surgical procedures -Bag-mask ventilations -Inadvertent esophageal intubation -External cardiac compressions -Heimlich manoeuvre
- 8. Penetrating Trauma Penetrating abdominal trauma has a slightly higher mortality rate Second most common cause of abdominal injury
- 9. Gunshot Injury Gunshot and stab wounds combine to cause 95% of penetrating abdominal injuries.
- 10. Prehospital Care • The goal of prehospital is to deliver the pt to hospital for definitive care as rapidly as possible. „Scoop and Run‟ • Maintain airway & start I V line • Care of spinal cord • Communicate to medical control • Rapid transport of patient to trauma centre
- 11. Initial Assessment and Resuscitation Primary survey Identification & treatment of life threatening conditions • Airway , with cervical spine precautions • Breathing • Circulation • Disability • Exposure
- 12. Emergency Care • I V fluids • Control external bleeding • Dressing of wounds • Protect eviscerated organs with a sterile dressing • Stabilize an impaled object in place • Give high flow oxygen • Immobilize the patient with a fractured pelvis • Keep the patient warm • Analgesics
- 13. Secondary Survey • General &Systemic Examination-to identify all occult injuries . • Special attention to Back, Axilla , Perineum • PR - sphincter tone ,bleeding ,perforation , high riding prostate • Foley‟s catheter- monitor urine out put • Nasogastric tube
- 14. Secondary Survey(contd.) AMPLE History A: Allergy M: Medications P: Past medical history L: Last meal E: Event - What happened
- 15. Examination • Laceration • Abrasion • Entry/Exit wounds • Involvement chest & Head injury • Seat Belt Sign
- 16. Examination Cullen’s Sign:1918 Bluish discoloration around umbilicus Diffusion of blood along periumbilical tissues or falciform ligament Hemoperitoneum Severe pancreatitis
- 17. Examination Grey-Turner’s Sign: (1877-1951) Bluish discoloration of the flanks Retroperitoneal Hematoma hemorrhagic pancreatitis. Kehr’s sign (1862-1916). Referred pain, Right shoulder irritation of the diaphragm (Splenic injury, free air, intra-abdominal bleeding)
- 18. Examination Balance’s Sign Dullness on percussion of the left upper quadrant ruptured spleen Labia and Scrotum : Pooling of blood from abdominal and pelvic cavities.
- 19. Examination Auscultation :1. Bowel sounds in the thoracic cavity (Diaphragmatic rupture) 2. Haemothorax Palpation: -Mass -Tenderness -Signs of peritonitis -# Ribs -Chest & Pelvic compression test
- 20. Investigations • FAST • X-Ray Chest & Abdomen • USG • CT Scan • Paracentasis • Diagnostic Peritoneal Lavage • Diagnostic Laparoscopy
- 21. Focused Assessment with Sonography in Trauma (FAST) • First used in 1996 • Rapid , Accurate • Sensitivity 86- 99% • Can detect 100 mL of blood • Cost effective • Four different views- Pericardiac Perihepatic Perisplenic Peripelvic space • Eliminates unnecessary CT scans • Helps in management plan
- 22. Plain X-Ray Chest & Abdomen • Pneumotharax, Haemothorax • Free air under diaphragm • Nasogastric tube, bowel loops in the chest • Elevation of the both /Single diaphragm • Lower Ribs # -Liver /Spleen Injury • Ground Glass Appearance – Massive Hemoperitoneum • Obliteration of Psoas Shadow –Retroperitoneal Bleeding • #vertebra
- 23. USG Advantage Disadvantage • Easy & Early to Diagnose . Examiner Dependent • Noninvasive • Obesity • No Radiation Exposure • Gas interposition Resuscitation/Emergency • Low Sensitivity for free fluid room less 500 mL Used in initial Evaluation • False –Negative retroperitoneal & Hallow Low cost viscus injury
- 25. Paracentasis • Four quadrant aspiration of abdomen • A Positive tap – blood , air , bile stained fluid • Negative tap doesn‟t rule out injury. • False negatives are as high as 22-60%
- 26. Diagnostic Peritoneal Lavage • First described in 1965 • Rapid & Accurate test used to identify intra-abdominal injuries • Predictive value of greater than 90% • The RBC count for lavage fluid is > 1,00,000/cu m.m. • A WBC count > 500/cu m.m. • Test is highly sensitive to presence of intraperitoneal blood • However specificity is low
- 27. Diagnostic Peritoneal Lavage Indications Contraindications • Clear indication for • Unexplained Shock Exploratory Laparotomy • Altered sensorium (Head • Relative injury , Drug) -Previous Expl. Laparotomy • General anesthesia for extra- -Pregnancy abdominal procedures -Obesity
- 30. CT Scan •Gold Standard •Haemodynamically Stable • Provides excellent imaging of pancreas, duodenum and Genitourinary system •Standard for detection of solid organs injury. • Determines the source and amount of bleeding • Can reveal other associated injuries e.g. Vertebral & Pelvic # & injury in the thoracic cavity . •High Specificity-95%
- 32. CT Scan Contraindication: • Clear indication for Laparotomy • Haemodynamically Unstable • Allergy to contrast media
- 33. DIAGNOSTIC LAPAROSCOPY • Haemodynamically stable patients • Inadequate/equivocal USG • Mild hypotension or persistent tachycardia • Persistent abdominal signs/symptoms • It decreases non-therapeutic laparotomies • Useful in penetrating injury • Limitation :Retroperitoneal Injury
- 34. Solid Organ Injuries • Grading of injured solid organs such as Spleen, Liver & Kidneys are on the basis of subcapsular hematoma ,capsular tear, parenchymal lacerations & avulsion of vascular pedicle • Bleeds significantly and cause rapid blood loss • Difficult to identify injury by physical exam • Repeated assessment is required to make the diagnosis • Slowly oozing blood into peritoneal cavity
- 35. SPLENIC INJURY • Most common intra- abdominal organ to injured (40-55%) • 20% of splenic injuries due to left lower rib fractures • Commonly arterial hemorrhage • Conservative management : -Hemodynamic stability - Negative abdominal examination -Absence of contrast extravasation in CT - Absence of other indication of Laprotomy -Grade 1to 3 (Subcapsular Hematoma ,Laceration <3 cm) Monitoring • Serial abdo. Examinations & Haematocrit are essential • Success rate of conservative m/m is >80%
- 36. Splenic Injuries Operative Management Capsular tears (I)- Compression & topical haemostatic agent Deep Laceration (II)- Horizontal mattress suture or Splenorrhaphy Major Laceration not involving hilum (IV)- Partial Splenectomy Hillar injury (V)–Total Splenectomy Grade IV-V: almost invariably require operative intervention Success rate of Splenic salvage procedure is 40-60%
- 37. Liver injury • Liver is the largest organ in abdomen • 2nd most common organ injured (35- 45%) in BTA • Driving and fighting responsible for 50% of deaths due to liver injury • Usually venous bleeding • 85% of all patients with blunt hepatic trauma are stable • CT is the mainstay of diagnosis in stable pt.
- 38. Liver Injury • 50% liver injury have stop bleeding spontaneously by the time of surgery Non Operative m/m • Haemodynamically Stable • No other intra-abdominal injury require surgery • < 2 units of BT required • Hemoperitoneum <500 ml on CT • Grade I-III(subcapsular & intr-perenchymal hematoma)
- 39. Liver Injury Operative m/m • Packing - Bleeding can be stopped by packing of abdomen -Pack removed after 48 hr -haemostatic agents -34 % survival in packing only
- 40. Liver Injury Operative Management(Contd.) • Suturing: -Simple suture -Deep mattress suture • Laceration: -Mesh hepatorrhaphy -Omental flap to cover the laceration - Debridement • Lobar Resection • Liver Transplantation • Ligate or repair damaged blood vessels & bile duct • Mortality of liver injury is 10%
- 43. Pancreatic Injury • Rare 10-20% of all abdominal injury • Crush , Direct blow to abdo & Seat belt injury • Associated with abdo. Duodenal injury, Vascular injury & liver injury • Diagnosis – Difficult, High index of suspicion • CECT Scan is helpful • Serum amylase is a poor indicator • Usually diagnose on Laparotomy • Distal Pancreatic injury - Distal resection • Pancreaticojejunostomy – Injury to Ampulla of Vater, Head & Body of Pancreas
- 45. Renal Injury • Clinically not suspected & frequently overlooked • Mechanism: Blunt , Penetrating # lower ribs or spinous process, Crush abdominal Pelvic injury Direct blow to flank or back Fall MVA
- 46. Renal Injury Diagnosis 1.History ,Clinical examination 2. Presentation :Shock, hematuria & pain 3. Urine: gross or microscopic hematuria
- 47. Renal Injury Diagnosis (contd.) 5.X-ray KUB IVP 7. USG 6.CT Scan abdomen 8. Radionuclide Scan The degree of hematuria may not predict the severity of renal injury
- 48. m
- 49. Renal Injury . Classification of Injury • Grade I : Contusion or Subcapsular Hematoma • Grade II: Non Expanding Hematoma, <1 cm deep ,no extravasation • Grade III: Laceration >1cm with urinary Extravasation • Grade IV: Parenchymal Laceration deep to CM Junction • Grade V: Renovascular injury
- 51. Management of Renal Injury About 85% of blunt renal trauma can be manage by conservatively Renal Contusion : Conservatively Renal exploration : Indication • Deep cortico-medullary Laceration with extravasation • Large perinephric Hematoma • Renovascular injury • Uncontrolled bleeding Before Nephrectomy ,Contralateral Kidney should be assessed
- 52. Diaphragmatic Injury • Incidence -0.8%-1.6% in BTA • High index of suspicion required , may be missed. • 40 to 50% are diagnosed immediately • Presentation may be delayed • Imaging Nasogastric tube seen in the thorax Abdominal contents in the thorax Elevated hemidiaphragm (>4 cm Lt vs Rt) Distortion of diaphragmatic margin. • Lt- 69% , Rt -24% B/L- 15%
- 53. Diaphragm Rupture /Hernia • S Lal, Y Kailasia , S Chouhan , APS Gaharwar, GP Shrivastava . Delayed presentation of post traumatic diaphragmatic hernia. JSCR 2011. 7:6
- 55. Diaphragm Rupture /Hernia S Lal, Y Kailasia, S Chouhan, APS Gaharwar, GP Shrivastava. Delayed presentation of post traumatic diaphragmatic hernia. JSCR 2011. 7:6
- 56. Hollow Viscus Injuries Gastric Injury : Penetrating trauma MC Blunt trauma abdomen 1% Causes Penetrating Injury -Crushing Against the Spine -CPR -Vigorous Ventilation with ET Tube in the Esophagus -Heimlich Maneuver Diagnosis : X-Ray chest & Abdomen CT scan Diagnostic Peritoneal Lavage During Surgical Exploration T/t : Expl. Laparotomy with Primary Repair
- 57. Hollow Viscus Injuries (Contd.) Duodenum Isolated Duodenum injury rare Incidence - 3-5% Cause :Penetrating injury: mc Steering wheel injury Assault Fall Associated with other intra-abdominal injury Diagnosis: Plan X-ray –Free air in abdomen -Intraoperative diagnosis Rx : Primary Repair 80% case Roux-en –Y duodenojejunostomy 20%
- 58. Hollow Viscus Injuries Small Intestine& Colonic Injuries Commonly Injured in Penetrating injury Blunt Trauma -Incidence 5% -20% Mechanism : -Crush Injury -At Fixed point DJ & IC Junction Rx : Exploratory Laprotomy
- 59. Bladder Injury • Commonly in BTA • 70% of bladder Injury are associated with pelvic fracture . • Hematuria Type 1.Extraperitoneal Rupture-by bony fragment • 2. Intraperitoneal Rupture- at dome when blow in distended bladder • Diagnosis -1. Clinical 2. Cystography T/t 1. Intraperitoneal –trans-peritoneal - closure +SPC 2:Extraperitoneal Rupture : Foley‟s catheter -10 -14 days
- 60. Ureteral Injury • Uncommon • Mostly occur after penetrating trauma • Associated with concomitant intra-abdominal or genitourinary injury • Diagnosis -IVP -15-20% Retrograde ureteroscopy - At the time of Laparotomy • Operative procedure Proximal & mid ureter -End to end Anastomosis over DJ Stent Distal –Ureteric Reimplantaion
- 61. Vascular Injury • Incidence 5-10% • Highly lethal. • Associated with extremely rapid rates of blood loss • Exposure is difficult in Laparotomy • Initial Control by digital pressure • Heparinized saline (50U/ml) injected in both end of vessel • Rx Lateral suture ,End to end Anastomosis & Interposition graft • Mortality rate is very high
- 62. Trauma in Pregnancy • Incidence- 10-20% • Causes: 1.Domestic violence 2.Sexual Assault 3. Accident • Third trimester- mc- balance & coordination disturbed • Multidisciplinary team- Obstetrician, surgeon, and neonatologist • Peritoneal sign are delayed • “Supine hypotensive syndrome” > 20 weeks‟ gestation. COMPLICATIONS • Fetal Injury & Death –fetoplacental injury, maternal shock, • Placental Abruption • Rupture of Uterus
- 63. Penetrating abdominal trauma •Gunshot •Stab wound
- 64. Penetrating Abdominal Trauma • Patients with deep penetrating injuries always require surgery • Common Organs –Small int.(29%) liver(28%) Colon(23%)
- 65. EAST Algorithm: Stable Eastern Association for the Surgery of Trauma, 2001
- 66. Penetrating Abdominal Trauma(Contd.) • Multiple in 20% of cases • Most stab wounds do not cause an intraperitoneal injury • A complete Laparotomy is mandatory
- 67. Penetrating Abdominal Trauma(Contd.) Abdominal Evisceration
- 69. Stab wound to right lower quadrant with caecal evisceration. No colon injury at laparotomy
- 70. Penetrating Abdominal Trauma(Contd.) Abdominal Evisceration • Never try to replace organs • Cover with moist gauze, then sterile dressing. • Transport immediately
- 71. Gunshot Injury • Handguns, Rifles, and Shotgun • More dangerous than penetrating injury • The degree of injury depends . Amount of kinetic energy imparted by the bullet to the victim Mass of the bullet and the square of its velocity Distance . • Injury multiple organ
- 72. Injury Prevention 1.Primary: Prevent an injury from its occurrence in the first place: Educational activity such as anti- drink-driving campaigns , speed limit rule -Children should accompanied with parent 2.Secondary: Attempts to lesson the consequences of injury – making road & safer car, anti-locking brakes, air bags , helmets, seat belt 3. Tertiary: Minimize the effect of injury by health care by individuals & system.
- 73. Injury Prevention (Contd.) • Speed is a critical factor ; a 10% increase speed translate into a 40% rise in the case fatality rate. • Use of seat belt reduces the risk of death or serious injury by 45%. • Air Bags reduces the risk of fatal injury by 30% & deaths by 11 %. • Children Below 12yrs should be properly restraints in the back seat. • Motorcycle experience death rate 35 time greater than car.
- 74. Summary • Injuries are Preventable • Trauma is a massive & growing health burden worldwide ,which increasingly afflicts the young & productive age group. • Repeated assessment is required to make the diagnosis • Ultrasonography and peritoneal aspiration are rapid methods of determining or excluding the presence of Hemoperitoneum • Conservative approach in Liver & Renal Injury • Successful m/m of trauma requires integration of Prehospital ,in-hospital ,& rehabilitative care.