Mastectomía
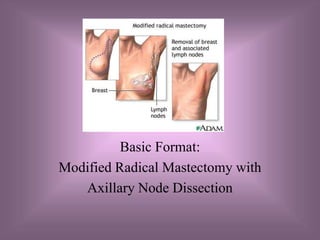
- 1. Procedures Basic Format: Modified Radical Mastectomy with Axillary Node Dissection
- 2. Objectives • Assess the anatomy, physiology, and pathophysiology of the breast • Analyze the diagnostic and surgical interventions for a patient undergoing a Modified Radical Mastectomy w/Axillary Node Dissection • Plan the intraoperative course for a patient undergoing Modified Radical Mastectomy w/Axillary Node Dissection • Assemble supplies, equipment, and instrumentation needed for the procedure.
- 3. Objectives • Choose the appropriate patient position • Identify the incision used for the procedure • Analyze the procedural steps for Modified Radical Mastectomy w/Axillary Node Dissection • Describe the care of the specimen • Discuss the postoperative considerations for a patient undergoing Modified Radical Mastectomy w/Axillary Node Dissection
- 4. Terms and Definitions • Benign vs Malignant • Biopsy • Frozen Section • Gynecomastia • In situ • Mammography • Mammoplasty • Mastectomy • Xeroradiography
- 5. Definition/Purpose of Procedure • Ablative/Treatment: remove diseased tissue • Removal of the breast tissue and lymph nodes under the arm (axillary node dissection), leaving the chest wall muscles intact
- 10. Lumpectomy
- 11. Relevant A & P 1. Mammary glands are between the 3rd and 7th ribs at ant. Chest wall 2. Areola 3. Nipple 4. Cooper’s Ligaments 5. Tail of Spence
- 14. Breast Incisions
- 15. Pathophysiology: Breast CA • Begins as a single transformed cell • Is hormone dependent • Classified: non-invasive (in situ) vs invasive • Categories: CA of mammary ducts, ca of mammary lobules, or sarcoma of the breast • Most: adenocarcinomas • 70% Infiltrating ductal carcinoma • Metastasis to other sites
- 16. Breast Cancer Location by Quadrant
- 17. Pathology: Breast CA Staging Stage 1 Stage II Stage III Stage IV Size Large & fully integrate < 1-2 cm 2-5 cm > 5 cm w/surrounding tissue Location Breast mass w or Breast mass w Distant Metastasis Confined to breast w/o susp palpable, fixed Ax Extension to skin ALNodes &/or subclavicular Lympedema L Nodes. No D Metastasis Surgical Options Modified or Radical or Segmental; Breast Total Radical Extended Rad Conservation Surg Mastectomy Mastectomy Mast for Stages I & II Lumpectomy w/AND & Rad Tx
- 18. Axillary Lymph Node Dissection
- 19. Manifestations of Breast Cancer • Breast mass or thickening • Unusual lump in underarm or above collarbone • Persistent rash near nipple area • Flaking or eruption near the nipple • Dimpling, pulling, or retraction in an area of the breast • Nipple discharge • Change in nipple position • Burning, stinging, or pricking sensation
- 20. Diagnostics • Exams – Initial breast exam or mammography – Chest x-ray – Bone scanning • Preoperative Testing
- 21. Surgical Intervention: Special Considerations • Patient/Family Factors – High Anxiety/Apprehension due to upcoming loss/disfigurement: alert to need for therpeutic communication & alleviation via meds • Room Set-up: Standard – Have mammograms in the OR – Notify pathology if Frozen sections will be required before case begins—ensure pathologist present • Universal Protocol • May use special techniques for Cancer – May prefer to irrigate with sterile water to crenate (shrivel or shrink) cancerous cells.
- 22. Surgical Intervention: Anesthesia • Method: General • Equipment: Typical monitors and machines
- 23. Surgical Intervention: Positioning • Position during procedure – Supine with operative side close to bed edge – Arm on operative side is extended to < 90 degrees on a padded armboard • Supplies and equipment: May place small sandbag or folded sheet under shoulder of affected side; may use special arm table or double it • Special considerations: high risk areas
- 24. Surgical Intervention: Skin Prep • Method of hair removal • Anatomic perimeters – Shoulder, upper arm extending down to the elbow (circumferentially), the axilla, & chest to table line and to the shoulder opposite from affected side—access to underarm for AND and possible extend to fingertips of operative side – Arm on operative side should be draped free using stockinette & drapes that allow free movement of the arm to facilitate access to the axilla • Solution options – Betadine or Hibiclens
- 25. Surgical Intervention: Draping/Incision • Types of drapes: Chest/Breast drape; stockinette • Order of draping – Anticipated area is outlined with adhesive towels or cloth towels & clips – Chest/Breast drape – Draping of arm includes placement of sheet on armboard and appl of stockinette over entire arm • Special considerations: may need 2 set-ups; use of Sterile water intraop irrigation • State/Describe incision: usually elliptical for MRM—see slide
- 26. Surgical Intervention: Supplies • General: Prep set, basic pack, basin set, chest drapes, ESU pencil/holder, gloves, Blades # 10 x 3, drsg: 4 x 4’s & ABDs • Specific – Suture: Silk, Dexon, Nylon for drain – Medications on field (name & purpose) – Catheters & Drains: Closed wound drainage system x 2 (Jackson Pratt vs Hemovac)
- 27. Surgical Intervention: Instruments • General: Major tray • Specific: extra hemostats (Adair breast clamps/large towel clips or Criles ) • Rake retractors • If skin graft anticipated: Brown dermatome w/mineral oil, tongue blades, etc.
- 28. Surgical Intervention: Equipment • General: Suction, ESU with Dispersive electrode—may need to simultaneously • Specific: may need additional armboard or special armrest
- 29. Surgical Intervention: Procedure Steps Overview • Breast incised elliptically • Incision deepened to encompass entire breast • Breast removed en bloc w/ALNs • Axillary lymph nodes are removed • Wound is closed
- 30. Surgical Intervention: Procedure Steps • Surgeon incises skin around the breast elliptically and deepens w/ESU pencil—lateral extension toward the axilla thru the subcutaneous tissue. Bleeding is controlled w/hemostats and ligatures or ESU • Surgeon dissects the skin from the underlying tissue w/#10 blade on # 3 knife handle and or ESU pencil – Blades dull easily and will need changing—notify Surgeon each time – Crv. Metzenbaum scissors are used to isolate large vessels from the breast tissue when the surgeon extends the incision into the axilla • Beren’s retractors are used to elevate skin flaps. Allis or Kocher clamps are placed along breast tissue edges and retracted up by surgeon or assistant
- 32. Surgical Intervention: Procedure Steps • The margins of skin flaps are covered w/warm moist lap pads and held away w/retractors. • The intercostal arteries and veins are clamped and ligated. • The axillary flap is retracted for complete dissection of the axilla. • Careful attention is directed to preventing injury to the axillary vein & medial and lateral nerves of the pectoralis major muscle • The fascia is dissected from the lateral edge of the pectoralis muscle. Ligation of vessels is performed in the axilla & adjacent to sternum. The fascia is then dissected to the serratus anterior muscle. The thoracic & thoracodorsal nerves are preserved
- 33. Surgical Intervention: Procedure Steps • Be sure to keep exposed tissue moist with lap packs for protection • Surgeon dissects the breast and axillary fascia away from the latissimus dorsi muscle and suspensory ligaments—from near the clavicle to midportion of the sternum. The pectoralis major muscle is left intact. • The specimen is passed to STSR • Wound is inspected for bleeding sites, which are ligated & electrocoagulated, then irrigated (NS).
- 34. Surgical Intervention: Procedure Steps • Surgeon places closed-wound suction drainage tube(s) thru stab wounds and secured to skin w/nonabsorbable suture on a cutting needle • A few absorbable suture may be used in the subcutaneous tissue to approximate the skin edges. • Surgeon closes w/interrupted nonabsorbable sutures or staple, anchors drains, and connects to closed suction reservoir. • The dressing may be one of several: simple gauze, bulky held in place w/Surgi-Bra, or gauze and elastic wrap.
- 35. Counts • Initial: Sponges, Sharps, Instruments, Small items • First closing • Final closing – Sponges – Sharps – Instruments – Small Items
- 36. Dressing, Casting, Immobilizers, Etc. • Types & sizes: 4 x 4’s & Abd pads – May need ACE wraps or Surgical Bra • Type of tape or method of securing—Silk or Paper or Foam compression tape
- 37. Specimen & Care • Identified as Breast and axillary lymph nodes, Left or Right • Handled: Routine/large container – Ask : if estrogen or progesterone receptors studies are to be performed on a specimen, it is saved in Normal Saline or Dry
- 38. Postoperative Care • Destination – PACU • Expected prognosis (Good, Depends on Dx) – Referral to Reach to Recovery rehabilitative Program and Physical Therapy possible
- 39. Postoperative Care • Potential complications – Hemorrhage (vascular breast—watch) – Infection – Other: Damage to…. • Surgical wound classification – Class I
- 40. References • Alexander: pp. 637-655 • Berry & Kohn: pp. 637-641 • Fuller: pp. 321-322 • MAVCC Proc Unit 3 p. 69-70 • STST: pp. 457-461 • Lemone & Burke: pp. 1582-1594
