Medical Banking Brief
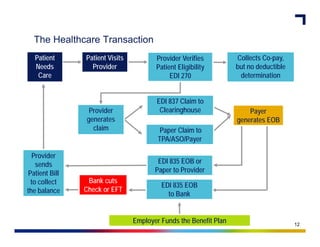
- 1. The Healthcare Transaction Patient Patient Visits Provider Verifies Collects Co-pay, Needs Provider Patient Eligibility but no deductible Care EDI 270 determination EDI 837 Claim to Provider Clearinghouse Payer generates generates EOB claim Paper Claim to TPA/ASO/Payer Provider sends EDI 835 EOB or Patient Bill Paper to Provider to collect Bank cuts EDI 835 EOB the balance Check or EFT to Bank Employer Funds the Benefit Plan 12
- 2. The American “Health” Express Card EMPLOYERS CONSUMERS PROVIDERS Wealth Management Health Management Secure your Wealth | Protect your Health 13
- 3. Win + Win + Win + Win Proposition EMPLOYERS CONSUMERS PROVIDERS Value-added service Transactional ease Speed of claims payment for employees with one card solution Reduction of credit Lower health costs Health and wellness balances Improved wellness Personal health record Real-time patient eligibility data Real-time access to health data BANK Capture all healthcare financial transactions Going beyond co-pay and deductible payments to holding in reserve all health-related funds 14
- 4. CLINICAL CORRELATION NEGOTIATION/SUPNET SERVICES REVIEW CODING REVIEW Kicking off the transactions HY CHARGE ADJUDICATED ELIGIBLE PT PRO ID CARD BENEFITS SERVICES CLAIM PAYER CO-PAY PRECERT BANK DEBIT FSA | HRA | HSA FUNDED PLAN | PREMIUMS ACCOUNT TREASURY | RETIREMENT | SWEEP 15
