RCPsychAGM10 - Nurses in nursing and residential care (June 10)
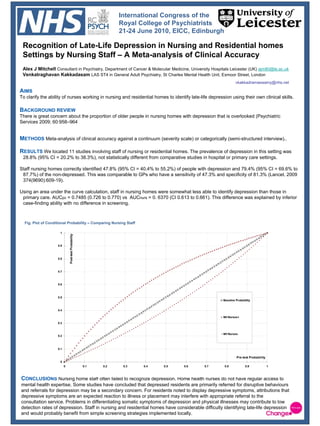
- 1. International Congress of the Royal College of Psychiatrists 21-24 June 2010, EICC, Edinburgh Recognition of Late-Life Depression in Nursing and Residential homes Settings by Nursing Staff – A Meta-analysis of Clinical Accuracy Alex J Mitchell Consultant in Psychiatry, Department of Cancer & Molecular Medicine, University Hospitals Leicester (UK) ajm80@le.ac.uk Venkatraghavan Kakkadasam LAS ST4 in General Adult Psychiatry, St Charles Mental Health Unit, Exmoor Street, London vkakkadramaswamy@nhs.net AIMS To clarify the ability of nurses working in nursing and residential homes to identify late-life depression using their own clinical skills. BACKGROUND REVIEW There is great concern about the proportion of older people in nursing homes with depression that is overlooked (Psychiatric Services 2009; 60:958–964 METHODS Meta-analysis of clinical accuracy against a continuum (severity scale) or categorically (semi-structured interview).. RESULTS We located 11 studies involving staff of nursing or residential homes. The prevalence of depression in this setting was 28.8% (95% CI = 20.2% to 38.3%), not statistically different from comparative studies in hospital or primary care settings. Staff nursing homes correctly identified 47.8% (95% CI = 40.4% to 55.2%) of people with depression and 79.4% (95% CI = 69.6% to 87.7%) of the non-depressed. This was comparable to GPs who have a sensitivity of 47.3% and specificity of 81.3% (Lancet. 2009 374(9690):609-19). Using an area under the curve calculation, staff in nursing homes were somewhat less able to identify depression than those in primary care. AUCpc = 0.7485 (0.726 to 0.770) vs AUCnurs = 0. 6370 (CI 0.613 to 0.661). This difference was explained by inferior case-finding ability with no difference in screening. Fig. Plot of Conditional Probability – Comparing Nursing Staff 1 Post-test Probability 0.9 0.8 0.7 0.6 0.5 Baseline Probability 0.4 NH Nurses+ 0.3 NH Nurses- 0.2 0.1 Pre-test Probability 0 0 0.1 0.2 0.3 0.4 0.5 0.6 0.7 0.8 0.9 1 CONCLUSIONS Nursing home staff often failed to recognize depression. Home health nurses do not have regular access to mental health expertise. Some studies have concluded that depressed residents are primarily referred for disruptive behaviours and referrals for depression may be a secondary concern. For residents noted to display depressive symptoms, attributions that depressive symptoms are an expected reaction to illness or placement may interfere with appropriate referral to the consultation service. Problems in differentiating somatic symptoms of depression and physical illnesses may contribute to low detection rates of depression. Staff in nursing and residential homes have considerable difficulty identifying late-life depression and would probably benefit from simple screening strategies implemented locally.
