23 genetic disorders
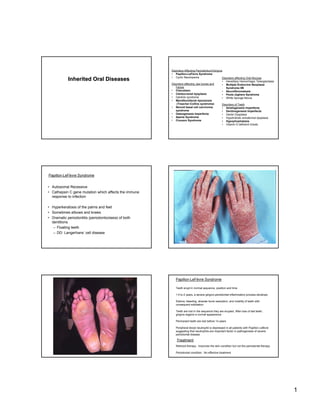
- 1. Disorders Affecting Periodontium/Gingiva • Papillon-LeFèvre Syndrome • Cyclic Neutropenia Inherited Oral Diseases Disorders affecting Oral Mucosa • Hereditary Hemorrhagic Telangiectasia Disorders affecting Jaw bones and • Multiple Endocrine Neoplasia Facies Syndrome IIB • Cherubism • Neurofibromatosis • Cleidocranial dysplasia • Peutz-Jeghers Syndrome • Gardner syndrome • White Sponge Nevus • Mandibulofacial dysostosis (Treacher-Collins syndrome) Disorders of Teeth • Nevoid basal cell carcinoma • Amelogenesis Imperfecta syndrome • Dentinogenesis Imperfecta • Osteogenesis Imperfecta • Dentin Dysplasia • Aperts Syndrome • Hypohidrotic ectodermal dysplasia • Crouzon Syndrome • Hypophophatasia • Vitamin D deficient rickets Papillon-LeFèvre Syndrome • Autosomal Recessive • Cathepsin C gene mutation which affects the immune response to infection • Hyperkeratosis of the palms and feet • Sometimes elbows and knees • Dramatic periodontitis (periodontoclasia) of both dentitions – Floating teeth – DD: Langerhans’ cell disease Papillon-LeFèvre Syndrome Teeth erupt in normal sequence, position and time 1.5 to 2 years, a severe gingivo-periodontal inflammatory process develops Edema, bleeding, alveolar bone resorption, and mobility of teeth with consequent exfoliation Teeth are lost in the sequence they are erupted. After loss of last teeth, gingiva regains a normal appearance Permanent teeth are lost before 14 years Peripheral blood neutrophil is depressed in all patients with Papillon-Lefèvre suggesting that neutrophils are important factor in pathogenesis of severe periodontal disease Treatment Retinoid therapy: Improves the skin condition but not the periodontal therapy Periodontal condition: No effective treatment 1
- 2. Cherubism Cherubism Radiographic features • Autosomal dominant • Multilocular radiolucency with massive expansion • Facial appearance similar to “cherub”-like • Both erupted and unerupted teeth are randomly distributed • 2 – 5 yrs of age • After stabilization, lesions exhibit a “ground glass” appearance • The clinical alterations typically progress until puberty, Histopathology stabilize and slowly regress • Similar to giant cell granuloma • Bilateral involvement of the posterior mandible – most • But clinical and radiographic correlation necessary common appearance – “cherub”-like (all 4 quadrants) • Vascular fibrous tissue and giant cells (smaller and • “Eyes upturned to heaven” appearance – due to involvement more focal) of the infraorbital rim and orbital floor • Eosinophilic cuffing around blood vessels • Painless bilateral expansion of the post. mand. Treatment • Marked widening and distortion of alveolar ridges • Prognosis is unpredictable • Tooth displacement and eruption failure • Delayed till after puberty (curettage) 2
- 3. Cleidocranial Dysplasia Caused by a defect in Cbfa1/Runx2 gene Autosomal dominant and sporadic pattern Bone defects involve the clavicle and skull Clavicles are absent (unilateral or bilateral) – 10% of cases Short stature with large heads; ocular hypertelorism; broad hypertelorism; base of nose and depressed nasal bridge Large heads and parietal bossing Skull sutures show delayed closure and may remain open Dental manifestations include narrow, high-arched palate high- with increased prevalence of cleft palate 3
- 4. Cleidocranial Dysplasia Presence of numerous unerupted permanent and supernumery teeth with many distorted crown and root shapes Prolonged retention of deciduous teeth and delay or complete failure of eruption of permanent teeth Histology: Unerupted permanent teeth lack secondary cementum Treatment: No treatment; full-mouth extractions with denture construction; full- removal of primary and supernumery teeth followed by exposure and orthodontic treatment of permanent teeth Crouzon Syndrome (Craniofacial Dysostosis) Dysostosis) Craniosynostosis: Premature closure of sutures Craniosynostosis: Mutation in FGFR2; 1 in 65,000 births; AD Wide variation in clinical presentation: Brachycephaly; Brachycephaly; scaphocephaly; trigonocephaly; “cloverleaf” skull (kleeblattschädel) scaphocephaly; trigonocephaly; cloverleaf” (kleeblattschädel) Ocular proptosis: blindness and hearing deficit proptosis: Headaches; normal intelligence Underdeveloped maxilla: Midface hypoplasia; crowding of maxillary teeth; bifid uvula “Beaten metal” skull in radiographs metal” Surgical treatment 4
- 5. Aperts Syndrome (Acrocephalosyndactyly) (Acrocephalosyndactyly) Craniosynostosis syndrome Mutation in FGFR2; 1 in 65,000 to 160,000 births, AD Acrobrachycephaly (tower skull); kleeblattschädel (severe cases) kleeblattschä Ocular proptosis; hypertelorism; vision loss; “beaten metal” proptosis; hypertelorism; metal” radiographs Midface hypoplasia; ‘V”-shaped arch “open-mouth” feature; open- mouth” hearing loss SYNDACTYLY of the 2nd, 3rd and 4th digits; MENTAL RETARDATION Pseudo cleft palate due to swellings (accumulation of glycos- glycos- aminoglycans) of the lateral hard palate and crowding of aminoglycans) maxillary teeth; bifid uvula Surgery 5
- 6. Treacher-Collins Syndrome (Mandibulofacial Dysostosis) Treacher- (Mandibulofacial Dysostosis) Defects of 1st and 2nd BA AD; 1 in 25,000 to 50,000 births; 60% new mutations Mutations in the TCOF1 gene Characteristic face: Hypoplastic zygoma causing narrow face with depressed cheeks and downward slanting palpebral fissures Coloboma (notch) at the outer portion of lower eyelid Ears anomalies: Deformed pinnae, extra ear tags, middle ear pinnae, ossicle defects cause hearing loss Underdeveloped mandible; condyle and coronoid hypoplasia Lateral facial clefting and cleft palate No treatment required in most cases; Cosmetic surgery in severe cases 6
- 7. Multiple Nevoid Basal Cell Carcinoma Syndrome (Gorlin Syndrome) • A.D.; high penetrance, variable expressivity • patched mutation, chr. 9 • Chief characteristics: multiple basal cell carcinomas, odontogenic keratocysts, epidermal cysts, palmar/plantar pits, calcified falx cerebri, rib anomalies, hypertelorism • Less common: strabismus, kyphoscoliosis, CNS tumors Multiple Nevoid Basal Cell Carcinoma Syndrome (Gorlin Syndrome) • Face: Frontal and temporoparietal bossing (big head), hypertelorism, mild mandibular prognathism • Skin: Basal cell carcinomas even in children and adolescence, often on non-sun exposed skin, few to hundreds; plantar and palmar pits (retardation of the epithelial growth) • Skeletal: bifid ribs, kyphoscoliosis • More than one odontogenic keratocysts 7
- 8. 8
- 9. Neurofibromatosis (von Recklinghausen disease of the skin) • A.D.; 50% of cases are new mutations; 1:3,000 births • Many forms • NF1 most common; chr. 17 • Malignant transformation Neurofibromatosis Neurofibromatosis (von Recklinghausen disease of the skin) (von Recklinghausen disease of • Diagnostic criteria (2 or more needed) the skin) – Six or more café au lait macules over 5mm in prepubertal and 15mm in postpubertal – Two NFs or one plexiform NF • Oral lesions – Axillary freckles (Crowe’s sign) – NFs anywhere – Optic glioma – Enlargement of fungiform papillae – Lisch nodules (brown pigmented spots of the iris) – Enlargement of mandibular foramen – Distinct osseous lesions (thinning of long bone cortex) – Enlargement of the mandibular canal – 1st degree relative with 2 or more of these findings 9
- 10. 10
- 11. Multiple Endocrine Neoplasia, Type Multiple Endocrine Neoplasia, IIB Type IIB • MEN I: tumors of pancreatic islets, adrenal • A.D.; 50% new mutations cortex, parathyroid glands and pituitary • Mutation of ret proto-oncogene, chr.10 gland • Marfanoid phenotype • Narrow face, thick lips, everted upper eyelid • MEN IIA: Sipple syndrome, • Neuromas on conjuctiva, eyelid margin or cornea pheochromocytomas and medullary • Oral lesions may be the first sign thyroid carcinoma – Lips, anterior tongue, buccal mucosa, gingiva, • MEN IIB: MEN IIA and mucosal neuromas palate, bilateral commissural neuromas Multiple Endocrine Neoplasia, Type IIB • Pheochromocytoma – Secretion of catecholamines – Sweating, diarrhea, headaches, flushing, heart palpitations and hypertension • Medullary carcinoma of the thyroid – Calcitonin production – Highly metastatic 11
- 12. 12
- 13. Peutz-Jeghers syndrome Peutz-Jeghers Syndrome Peutz- Autosomal Dominant Multiple perioral and oral ephelides or melanotic macules Intestinal polyposis Considered hamartomas but have minimal neoplastic potential (2 to 3% adenocarcinoma) adenocarcinoma) Small intestine (jejunum) Abdominal pain, rectal bleeding and diarrhea 13
- 14. Amelogenesis Imperfecta General Information General Information • Classification is impractical for clinicians • Absence of systemic disorder • Problems arise in one or more of the • Can be part of a syndrome three stages of enamel formation • Many types – Elaboration of enamel matrix; hypoplastic – Mineralization; hypocalcified • Different modes of inheritance – Maturation; hypomaturation • Understanding of molecular events • 1:800 – 1:15,000 (clustering) • Both dentitions 14
- 15. Hypoplastic type Hypoplastic type Generalized Pitted • Inadequate deposition of organic matrix • A.D. • Normal mineralization • Pinpoint/head pits in rows or columns • Radiographic contrast • In-between enamel normal • Seven types • Across the surface • Buccal surface more severely affected • Does not correlate with pattern of environmental damage Hypoplastic type Hypoplastic type Generalized Pitted Generalized Pitted Hypoplastic type Diffuse Smooth A.D. • Thin, hard, glossy • Like crown preparations, open bite • Opaque white to brown • X-ray: peripheral thin enamel outline • Unerupted exhibit resorption 15
- 16. Hypoplastic type Hypoplastic type Diffuse Smooth A.D. Diffuse Smooth A.D. Hypomaturation Type Hypomaturation Type Diffuse Pigmented A.D. • Defect in the maturation of enamel • Mottled brown crystals • Chipping from dentin with an explorer • Normal shape • Very uncommon anterior open bite • Mottled appearance • Soft similar to hypocalcified • White, yellow or brown • Calculus • Enamel is soft • Radiodensity similar to dentin Hypomaturation Type Hypomaturation Type Diffuse Pigmented A.D. Diffuse Pigmented A.D. 16
- 17. Hypomaturation Type Hypomaturation Type Snow-capped Teeth Snow-capped Teeth • X-linked, A.D.? • Zone of white opaque enamel on incisal and occlusal surface (1/4 to 1/3 of the surface) • Looks like fluorosis • Anteriors, anteriors/bicuspids, premolars/molars • Both dentitions Hypomaturation Type Snow-capped Teeth Hypocalcified Type • A.D. or A.R. (more severe) • No significant mineralization • Normally shaped teeth at eruption • Enamel very thin and easily lost • Yellow or brown color • Calculus • Open bite Hypocalcified Type Amelogenesis Imperfecta Treatment • Restorations as soon as possible • Dentures (overdentures) • Veneers in mild cases • Glassionomers for better adhesion to dentin 17
- 18. Osteogenesis Imperfecta Osteogenesis Imperfecta Weak bones, blue sclera, altered teeth, hearing loss, Heterogeneous group of disorders characterized by impairment long bone and spine deformity and joint hyperextension of collagen maturation Radiographic features include osteopenia, bowing, Mutations in type I collagen gene deformity of long bones and multiple fractures Most common type of inherited bone disease Oral manifestations are clinically similar to dentinogenesis imperfecta – premature pulpal obliteration Collagen forms a major portion of bone, dentin, sclerae, sclerae, ligaments, and skin Shell teeth can also be noted Autosomal dominant, autosomal recessive hereditary; sporadic However the two are different processes caused by different mutations Severity varies Opalescent teeth if associated with OI Maxillary hypoplasia Osteogenesis Imperfecta Four major types of OI Type I: Most common and mildest form Type II: Most severe; patients die before 4 weeks of age Type III: Most severe form beyond the perinatal age Type IV: Mild to moderate form Treatment: No treatment of OI Varied prognosis 18
- 19. Shell Teeth Hypophosphatasia • Autosomal recessive trait • Decreased alkaline phosphatase • Increased blood and urinary phosphoethanolamine • Bone defects similar to rickets • Premature loss of primary teeth without evidence of inflammatory response – No cementum on teeth Perinatal: most severe Infantile: normal till 6 months; failure to grow after that (severe) Childhood: usually detected at later age; teeth defects with enlarged pulp chambers; open fontanelles with premature fusion of cranial sutures Adult: mild 19
- 20. Vitamin D-Resistant Rickets (Hereditary Hypophosphatemic Rickets) Rickets resistant to vitamin D Inherited as X-linked dominant trait Males affected more severely than females Mutations in PHEX gene Rickets, hypophosphatemia due to decreaed capacity to reabsorb phosphate Teeth with large pulp chambers with pulp horns that extend almost to the DE junction leading to very small pulp exposures leading to multiple Periapical lesions and gingival sinus tracts It will as though periapical lesions on otherwise normal teeth as the exposures are so tiny 20